Children’s National designated Center of Excellence by Focused Ultrasound Foundation

“This designation provides a high level of recognition and legitimacy to the work our Children’s National team has done with MR-HIFU over many years,” says Karun Sharma, M.D., PhD, director of Interventional Radiology and associate director of clinical translation at the Sheikh Zayed Institute for Pediatric Surgical Innovation.
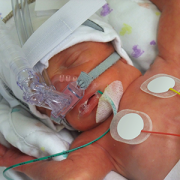
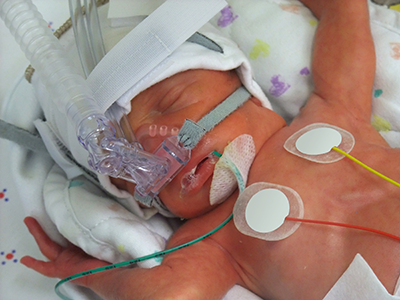
More precise, less invasive and less painful surgery with lower risk of complications and no radiation exposure – these are some of the benefits of treating pediatric tumors with Magnetic Resonance Guided High Intensity Focused Ultrasound (MR-HIFU). And now the Focused Ultrasound Foundation has designated Children’s National Hospital as the first global pediatric Center of Excellence (COE) for using this technology to help patients with specific types of childhood tumors.
“This designation provides a high level of recognition and legitimacy to the work our Children’s National team has done with MR-HIFU over many years,” says Karun Sharma, M.D., PhD, director of Interventional Radiology and associate director of clinical translation at the Sheikh Zayed Institute for Pediatric Surgical Innovation (SZI) at Children’s National. “This will allow our focused ultrasound program to expand to other areas of interest and become more cohesive while continuing to uncover additional clinical indications for pediatric patients.”
At Children’s National, radiologists use MR-HIFU to focus an ultrasound beam into lesions, usually tumors of the bone and soft tissues, to heat and destroy the tissue in that region. There are no incisions at all. In 2015, Children’s National doctors became the first in the U.S. to use MR-HIFU to treat pediatric osteoid osteoma, a painful, but benign, bone tumor that commonly occurs in children and young adults. The trial, led by Dr. Sharma, demonstrated early success in establishing the safety and feasibility of noninvasive MR-HIFU in children as an alternative to the current, more invasive approaches to treat these tumors. The team also conducted another clinical trial, led by AeRang Kim, M.D., Ph.D., a pediatric oncologist, to treat relapsed soft tissue tumors such as sarcomas.
Since then, the Children’s National team has built an active clinical trials program and become a leader in translation of focused ultrasound for the treatment of pediatric solid tumors. The center is currently investigating the treatment of malignant solid tumors with focused ultrasound alone and combined with chemotherapy.
“Focused ultrasound offers a number of important benefits over traditional therapies, which are especially paramount for the pediatric population,” said Focused Ultrasound Foundation Chairman Neal F. Kassell, M.D. “The team at Children’s National has an exemplary track record in using this technology to pioneer new treatment options for their patients, and we look forward to collaborating and supporting their future research.”
As a designated COE, Children’s National has the necessary infrastructure to support the ongoing use of this technology, especially for carrying out future pediatric clinical trials. This infrastructure includes an ethics committee familiar with focused ultrasound, a robust clinical trials research support team, a data review committee for ongoing safety monitoring and annual safety reviews, and a scientific review committee for protocol evaluation.
The program also features a multidisciplinary team of clinicians and investigators from SZI, radiology, oncology, surgery and orthopedics. With the new designation and continued expansion, we will expand MR-HIFU to other areas such as neuro-oncology, neurosurgery, and urology. Ongoing and future work will investigate a rational combination of MR-HIFU with local tumor drug delivery, immunotherapy and cellular therapy.
“This recognition sets us apart as a premier pediatric institution, and will allow us to pave the way to make pediatric surgery more precise and less invasive,” says Dr. Sharma.