Nathan Kuppermann introduces Holden Thorp during REI Week.

Nathan Kuppermann, Richard Childs and Catherine Bollard during REI Week.

CNRI leadership with Adam Carroll.

Pamela Hinds presents Lauren Clark during REI Week programming.
Kelly Gebo presents during REI Week.

Presenters of the joint AI lecture during REI Week with Nathan Kuppermann.

Jill Joseph delivers a lecture during REI Week.

Howard Bauchner presents during REI Week.

Holden Thorp delivers remarks during REI Week.

Panel discussion focused on drug and device development during REI Week.

Matthew Bramble presents during REI Week.

Catherine Bollard speaks during REI Week programming.

Nathan Kuppermann and colleagues view posters during a REI Week poster session.
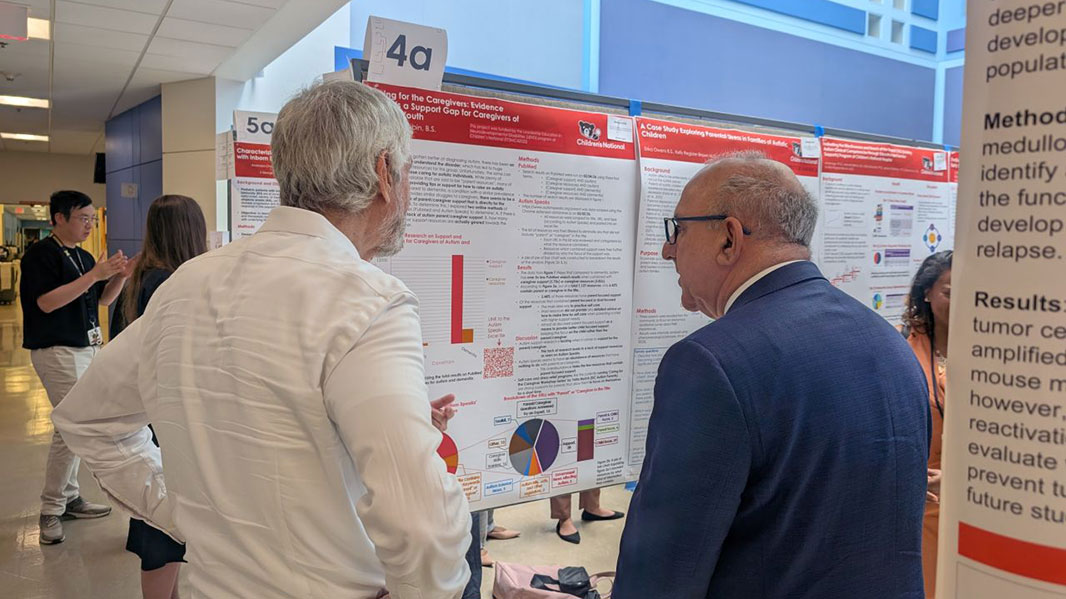
REI Week staff on Tuesday of the event.

Attendees gather for the REI Week awards ceremony.

The auditorium during the REI Week awards ceremony.

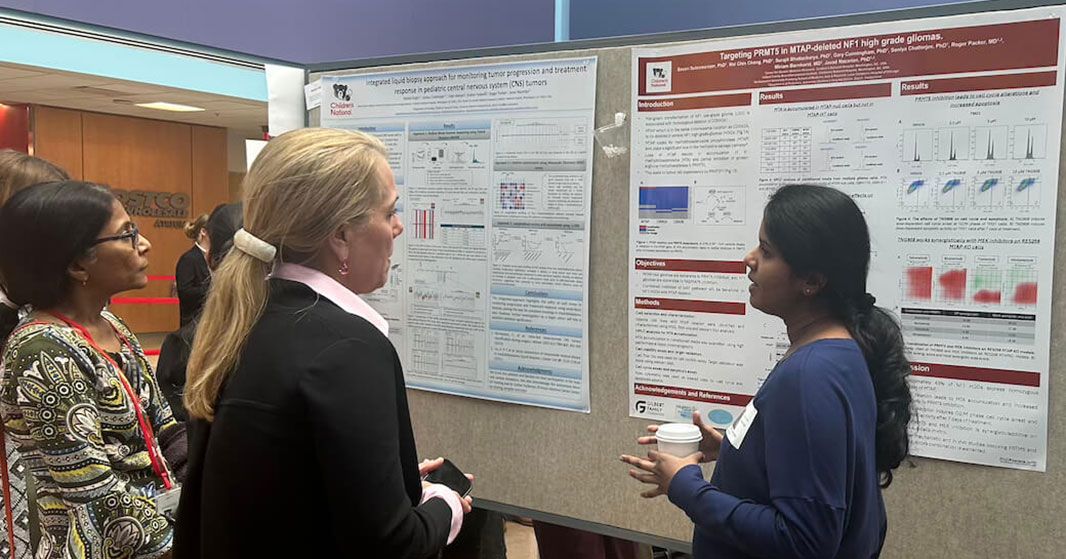
Poster session held on Tuesday during REI Week.

Members of the Academic Research Operations team during REI Week.

Members of the Academic Research Operations team at Children’s National.

Aaron Carroll presents during REI Week 2026.

Poster session held on Wednesday during REI Week.

Panel discussion focused on media and communication during REI Week.

Nathan Kuppermann participates in a Safe Kids event during REI Week.

Poster session held on Thursday during REI Week.
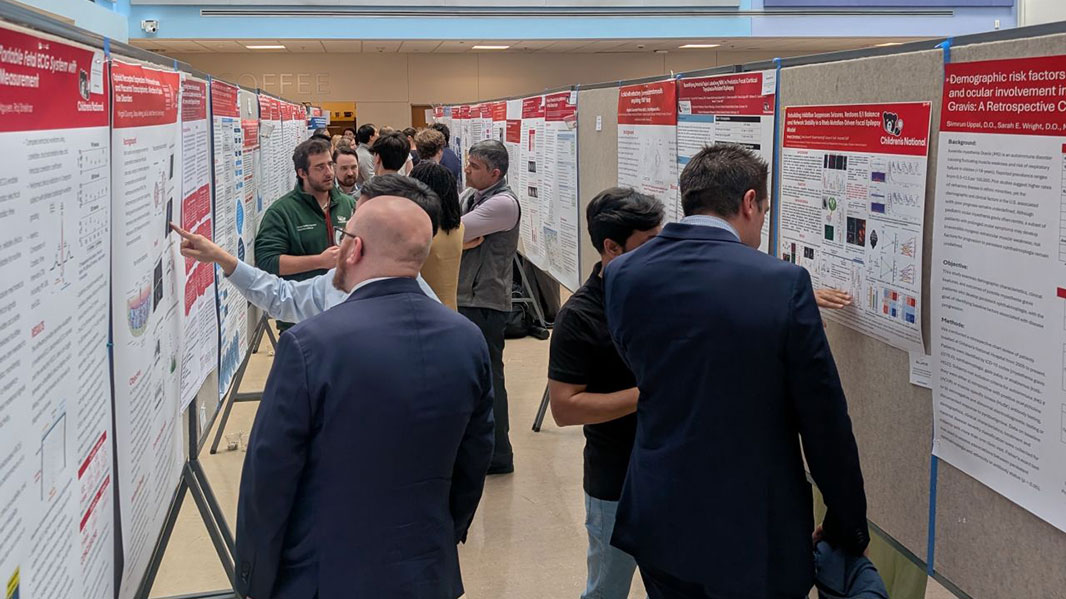
Research Sponsored Projects and Business Services staff with Nathan Kuppermann during REI Week.

REI Week staff members during the event.

Peter Hotez presents during REI Week.

Nam Tran presents during REI Week.

Nathan Kuppermann speaks during REI Week.

For five days in April, the hallways, auditoriums and virtual platforms of Children’s National Hospital became a space for the kind of honest and necessary conversations that move pediatric science forward. Research, Education & Innovation (REI) Week 2026, held April 13–17, brought together investigators, clinicians, trainees and partners across disciplines to grapple with the theme: reimagining a brighter future for children through bold research and novel collaborations. REI Week remains a cornerstone of the institution’s academic mission 16 years in and this year’s edition made clear that progress in pediatric health demands not just discovery, but clarity of purpose and the courage to push forward.
Making the case for pediatric-first development
Innovation Day opened the week at the Research & Innovation Campus with a panel discussion on drug and device development. Panelists were clear that making pediatric drug and device development a genuine priority is essential to delivering safe, effective care.
A media and social media panel pushed researchers toward another uncomfortable question: why should anyone outside this building care about what we do? Speakers explored how to frame research so it resonates beyond academic circles, making the case that storytelling and audience awareness are not soft skills but a part of the job.
A Shark Tank-style session showcased diverse artificial intelligence (AI) project proposals aimed at advancing pediatric care and research, with teams presenting bold ideas in a competitive format.
Standing up for science and innovation
Holden Thorp, PhD, editor-in-chief of Science, set a defining tone for the week in his Monday keynote, speaking frankly about the importance of resisting external pressures and standing up for scientific integrity. His message — that science must hold its ground even when it’s difficult — echoed throughout the days that followed.
Richard Childs, MD, assistant U.S. surgeon general and scientific director of the National Heart, Lung and Blood Institute, reinforced why sustained investment matters, highlighting how resources and infrastructure at the National Institutes of Health (NIH) enable the kinds of accomplishments that transform care. Kelly Gebo, MD, MPH, dean of the Milken Institute School of Public Health at George Washington University, grounded leadership in something simpler: “Listen before acting. Stay grounded in values. Adapt to change. Explore new funding. Communicate clearly. Lead with empathy.”
A trust problem, not a knowledge problem
Midweek programming zeroed in on research communication and didn’t flinch. Howard Bauchner, MD, vice chairman of pediatrics at the Boston University School of Medicine, delivered the Larrie Greenberg Grand Rounds Lecture with a call for a cultural shift: quality, not quantity, of publications must become the norm for the research enterprise to regain credibility.
The Jill Joseph Grand Rounds Lecture with Aaron Carroll, MD, MS, president and CEO of AcademyHealth, reframed how the field thinks about science dissemination. The problem, Dr. Carroll argued, is not that the public lacks knowledge, it is that they lack trust. He urged a shift toward solutions-based research and challenged researchers to understand the difference between relative and absolute risk, noting that headlines almost always reach relative figures. If science wants to grab attention responsibly, it has to understand how attention actually works.
Peter Hotez, MD, PhD, professor of pediatrics and molecular virology and microbiology at Baylor College of Medicine, co-director of the Texas Children’s Hospital Center for Vaccine Development and dean of the National School of Tropical Medicine, brought the stakes into sharp relief in his lecture on vaccines and immunizations in an era of anti-science, describing his personal and professional journey, including writing “Vaccines Did Not Cause Rachel’s Autism”, as part of an ongoing effort to counter misinformation and advocate for the families most affected by it.
Lauren Clark, PhD, RN, FAAN, professor and Shapiro Family Endowed Chair in Developmental Disability Studies at UCLA’s Joe C. Wen School of Nursing, closed the communication thread with a pointed observation: if researchers never leave their own scientific community, they are missing the boat. She emphasized that plain language is a strategy, not a compromise.
From global health to the clinic floor
Matthew Bramble, PhD, assistant professor and data sciences faculty member at Children’s National, delivered the Global Health Sponsored Lecture on ending the scourge of Konzo in the Democratic Republic of Congo. His work in this isolated environment — where populations depend heavily on cassava — could unlock information relevant far beyond Konzo itself, potentially shedding light on diseases like ALS.
The joint Lecture on AI featured two complementary perspectives on machine learning’s growing role in care delivery. Hooman Rashidi, MD, MS, associate dean of AI in medicine, professor and endowed chair of Lombardi-Shinozuka Experimental Pathology Research at the University of Pittsburgh School of Medicine proposed a mixed approach with a human in the loop as the responsible path forward. Nam Tran, PhD, MS, professor of pathology, associate dean of biobanking and medical director of Point of Care Testing at the University of Pittsburgh, highlighted AI’s potential in austere settings, field medicine, military contexts and disaster response, where speed and limited resources put a premium on intelligent decision support.
What the abstracts reveal
This year’s poster sessions drew more than 450 abstracts spanning 46 research categories — a record number that reflects both the depth of work underway at Children’s National and the range of challenges the institution has committed to tackling. Oncology, neuroscience and neuroprotection, cancer immunology and bone marrow transplantation represented some of the largest clusters of work, with investigators exploring everything from gene therapy for beta-thalassemia to advanced neuroimaging frameworks for fetal and neonatal populations. Digital innovation, data science and AI also drew a strong showing, with studies applying machine learning to EEG-based cognitive assessment, predictive modeling and clinical decision support, reflecting the institution’s growing investment in responsible, data-driven care.
Equally notable was how questions of access and reach have woven themselves into categories that might not have carried that framing in prior years. Research on firearm violence, pathways to mental health care and the downstream effects of social conditions on pediatric outcomes appeared across multiple categories. Community research submissions highlighted school-based telehealth programs and outreach initiatives that extend Children’s National’s reach into underserved communities across the Washington region. Psychology and wellness, quality improvement and treatment compliance rounds out a body of work that asks not just what works scientifically, but who benefits and whether they can actually access what works.
Global and climate health emerged as a distinct and growing area, with submissions connecting environmental conditions to pediatric disease burden and mortality. Taken together, this year’s abstracts capture a field that is translating molecular discoveries into clinical applications, integrating technology with intention and making sure research translates to care for children who need it most.
This year’s honorees
REI Week concluded Thursday with an awards ceremony honoring outstanding contributions across research, education and innovation.
Award winners:
POSTER SESSION AWARDS
Basic & Translational Research
Faculty: Yingshi Ouyang, PhD
“Opioid Receptor Expression in the Human Placenta and Placental Transcriptomic Alterations in Opioid Use Disorders”
Postdocs/Fellows/Residents: Margaret Hines, PhD
“Understanding the Role of Cranial Mesenchyme in Neural Tube Closure”
Postdocs/Fellows/Residents: Khatereh Khorsandi, PhD
“Reprogramming the Immunosuppressive Microenvironment to Enhance CAR T‑Cell Therapy in Diffuse Intrinsic Pontine Glioma”
Staff: Zara Hasnani
“Evaluation of Virus‑Specific T Cell Immunity in Pediatric Inflammatory Bowel Disease Patients on Biologic Therapy”
Graduate Students: Elton VanNoy
“Modulating DNA Methylation During CAR T Manufacturing to Enhance Immunotherapy for Pediatric Glioma”
Graduate Students: Woudasie Admasu
“Identification of Druggable Host Factors to Prevent RSV Infection Using CRISPR‑Cas9”
High School/Undergraduate Students: Akhil Chada
“Designing of PepMLM‑Based Peptide Binders to Target Tumor‑Specific Splice Event‑Derived Proteoforms in Pediatric High‑Grade Gliomas”
Clinical Research
Faculty: Matthew Bramble, PhD
“Pathways Involving Oxidative Damage Mitigation is Likely the Biological Risk Factor for the Development of Konzo”
Postdocs/Fellows/Residents: Maria Triantafyllou, MD
“Plasma Metabolomic Signatures for Diagnosis and Risk Stratification of Pediatric Sepsis in the Emergency Department”
Staff: Pooneh Roshanitabrizi, PhD
“Synthetic Dual‑Channel Color Doppler Echocardiography for Rheumatic Heart Disease Detection in Low‑Resource Settings”
Graduate Students: Jasmine Nguyen
“The Relationship Between Cloacal Complexity and Early Vaginal Stenosis After Cloaca Repair”
Graduate Students: Maria Straker Brito, MD
“High Airway Type‑III IFN Levels by Airway Epithelial Cells are Associated with Increased Pro‑Inflammatory Cytokines Production in the Airways”
Graduate Students: Artur Aharonyan, MS
“Automating AMPs: An AI Pipeline for Generating 3D‑Printable BioAMP Plates in Unilateral Cleft Lip and Palate”
Graduate Students: Jaisimar Singh
“Mechanical versus Non‑Mechanical Bowel Management in Children with Spina Bifida: A Cross‑Sectional Comparison of Patient‑Reported Symptoms”
High School/Undergraduate Students: Medha Pappula
“Integrating Multimodal Clinical Data with Large Language Models to Predict Outcomes in Pediatric Metabolic and Bariatric Surgery”
High School/Undergraduate Students: Keertana Senthilkumar
“Diagnostic Utility of Vascular Catheter Tip Cultures”
Community‑Based Research
Faculty: Katie Donnelly, MD, MPH
“Evaluating the Propagation of Firearm Violence After an Incident Event”
Postdocs/Fellows/Residents: Brittany Fitzpatrick, MD, MPH
“Walking Towards Equity: Enhancing Pediatric Pedestrian Safety Through Data‑Driven Solutions”
Postdocs/Fellows/Residents: Krithika Iyer, PhD
“Predicting Early Cognitive Risk Using Ultra‑Low‑Field MRI Brain Volumetry and Demographic Measures in Low‑Resource Settings”
Staff: Megan Lau
“A Longitudinal Examination of Social Support as a Mechanism of Change in Executive Function in a School‑Delivered Intervention for Adolescents with ADHD”
Graduate Students: Preeyanka Rao, MPH
“Comparison of Asthma Utilizations Across Different Medicaid Insurance Plans in the District of Columbia”
High School/Undergraduate Students: Riya Mehta
“Availability and Knowledge of Naloxone Distribution in an Urban Area”
Education, Training and Program Development
Faculty: Amy Wolfe, MD, MEd
“A Missed Conversation: Spirituality as a Persistent Gap in PCCM Communication Training”
Postdocs/Fellows/Residents: Taylor Goodman, MD
“The POCUS Pathway: A Novel Point‑of‑Care Ultrasound Longitudinal Curriculum for Pediatric Residents”
Postdocs/Fellows/Residents: Jennifer Bertollo, PhD
“Online Educator Training for an Executive Function Intervention: Mixed Methods Educator Feedback and Impact on Adoption”
Staff: Tininka Rahman, MHA
“Establishing a Community Engaged Research and Training (CERT) Hub at Children’s National”
Graduate Students: Novelle Leach
“PCIT and SPACE Parenting Interventions: Are They Meeting the Needs of Young Children with Neurodevelopmental Disabilities and Their Families?”
Quality and Performance Improvement
Faculty: Jessica Lazerov, MD, MBA
“Using LEAN Methodology to Improve Immunization Reconciliation and Vaccination Rates”
Postdocs/Fellows/Residents: Maya Gibson, MD
“Evaluating Blood Product Utilization on ECMO Following Implementation of Restrictive Transfusion Strategies”
Staff: Abhijeet Parida, MS
“HOPE4KIDS: AI‑Based Webtool for Neuro‑Oncology Segmentation and Volumetrics”
Graduate Students: Benjamin Upbin
“Caring for the Caregivers: Evidence Reveals a Support Gap for Caregivers of Autistic Youth”
High School/Undergraduate Students: Safinabonu Juraeva, MPS
“Diagnosing Primary Bottlenecks in the PICU‑to‑Floor Transfer Process to Improve Transfer Efficiency”
AI SHARK TANK EVENT WINNERS
Smart AI for Environments (SAFE) Kids App
Team:
Christopher Gable, DO
Sadiqa Kendi, MD, MPH
Fatemeh Naghiloo, MArch, MPH
Pooneh Roshanitabrizi, PhD
Nishad Prakash Kulkarni, MEng
Syed Muhammad Anwar, PhD
Youness Arjoune, PhD
StrepApp: AI‑Based Strep Throat Diagnosis from Smartphone Images
Team:
Raj Shekhar, PhD
Jeffrey Dome, MD, PhD
Rana Hamdy, MD, MSCE, MPH
Youness Arjoune, PhD
Trong N. Nguyen, PhD
INAUGURAL PLANET‑POSITIVE PIONEER AWARD
Demilade Haastrup, PharmD, RPh
“Decreasing Single‑Use Plastic Within the Pneumatic Tube System During Medication Transport Through a QI Initiative”
MENTORSHIP AWARDS (16th Annual)
Translational Research
Michael Keller, MD
Panagiotis Kratimenos, MD, PhD
Clinical Research
Eleanor R. Mackey, PhD
CHU FAMILY FOUNDATION AWARD
Katherine Ottolini, MD
“BOOST‑Milk Study: Bringing Oura Optimization Support to Milk”
Kristen Johnson, MD
“Exploring the Impact of AI‑Generated Plain Language Clinical Summaries on Caregiver Understanding”
THE SUZANNE FEETHAM NURSING RESEARCH SUPPORT AWARD
Olivia Miller, MA, BCBA, LABA
“Using Video Prompting to Teach Tracheostomy Tie Changes to Caregivers”
Shripriya Mohan‑Oneill, MSN, CPNP
“Artificial Intelligence Integration into Advanced Practice Nursing”
EXPLORATIONS IN GLOBAL HEALTH PILOT AWARDS
Sarah Mulkey, MD, PhD
“Understanding Environmental and Community Factors in Children with Prenatal Zika Virus Exposure in Colombia”
Meleah Boyle, PhD, MPH and Ann Mead, MPH
“Protecting Children’s Health in Local and Global Communities Through Environmental Sustainability Education”
ELDA ARCE TEACHING SCHOLAR AWARD
John Berger III, MD
Cardiac Critical Care Medicine
Sivabalaji Kaliamurthy, MD
Child and Adolescent Psychiatry
RESEARCH RANGERS
Winner: Sebastian
Fourth‑grade patient participant in REI Research Rangers
Looking ahead at a brighter future
The conversations held during REI Week 2026 continue throughout the year. They carry forward into labs, clinics and classrooms, and ultimately into the lives of the children and families this institution exists to serve.
That dialogue also extended online through The Lead in Peds Unplugged episodes featuring notable speakers from the week and leaders at Children’s National talking about the ideas, challenges and collaborations shaping pediatric health. These conversations included Dr. Holden Thorp, Dr. Kelly Gebo, Dr. Hooman Rashidi and Dr. Nam Tran, Dr. Patrick Hanley and Dr. Matthew Bramble.
REI Week also highlighted the teams and programs that support research across its full lifecycle, with the Clinical Research Unit, Innovation and Technology Transfer Office and Research Sponsored Projects and Business Services maintaining a visible presence throughout the week to engage investigators and answer questions. Opportunities for connection extended beyond formal sessions through events such as the “global health mix & mingle”, sponsored by the Global Health Initiative, which brought participants together to engage around Children’s National’s work in local and global communities. Educational programming continued through Children’s Academy of Pediatric Educators sessions that explored how research and teaching intersect in practice, including discussions on the effectiveness of case-based teaching, pathways in medical education and the value of embracing failure as a driver of growth in academic medicine. Beyond the lecture halls, community engagement remained central, with a Safe Kids Worldwide event on Friday focused on fostering safety education and training for children and families. Supported by executive sponsors Nathan Kuppermann, MD, MPH; Catherine Bollard, MBChB, MD; Stella Ghattas, Esq; Elizabeth Wells, MD; and Cicely (CC) Brooks, DNP-ENL, MSN, RN, NE-BC, FAB, Children’s National continues to build the conditions where that kind of science can thrive.
REI Week 2027 takes place the week of April 5, and what happens between now and then matters just as much as what happens during that week. Every study advanced, every collaboration forged and every trainee who finds their footing in this community is part of the same long effort to reimagine what pediatric health can look like. That work doesn’t happen without investment in people, in ideas and in the infrastructure that turns discovery into care. If this week moved you, consider supporting what comes next.


































 Children’s National is ranked one of the top 10 pediatric hospitals in the nation by U.S. News & World Report. Our faculty and staff are proud of the impact made on the lives of children and families in our community. Your participation in the U.S. News & World Report annual reputational survey validates the quality of care we provide and reflects the mutual respect and trust we share as healthcare professionals.
Children’s National is ranked one of the top 10 pediatric hospitals in the nation by U.S. News & World Report. Our faculty and staff are proud of the impact made on the lives of children and families in our community. Your participation in the U.S. News & World Report annual reputational survey validates the quality of care we provide and reflects the mutual respect and trust we share as healthcare professionals.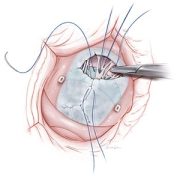
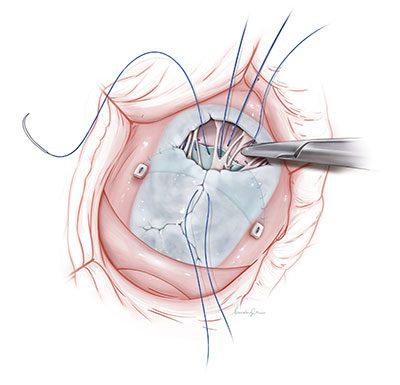



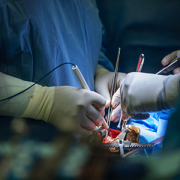
 In 2025, Children’s National Hospital was featured in major national news outlets for pioneering advances in pediatric care, groundbreaking clinical research and powerful human stories of healing and hope. From gene therapy for sickle cell disease and innovative pacemakers for newborns to breakthrough transplants, cancer trials and emerging mental health concerns like AI psychosis, these stories highlight the hospital’s leadership across the full spectrum of pediatric medicine. The following ten highlights showcase the patients, families and experts behind this impact, as reported by outlets including NBC News, The Washington Post, Good Morning America, USA Today, Healio, ABC News and ESPN.
In 2025, Children’s National Hospital was featured in major national news outlets for pioneering advances in pediatric care, groundbreaking clinical research and powerful human stories of healing and hope. From gene therapy for sickle cell disease and innovative pacemakers for newborns to breakthrough transplants, cancer trials and emerging mental health concerns like AI psychosis, these stories highlight the hospital’s leadership across the full spectrum of pediatric medicine. The following ten highlights showcase the patients, families and experts behind this impact, as reported by outlets including NBC News, The Washington Post, Good Morning America, USA Today, Healio, ABC News and ESPN.



 Children’s National Hospital in Washington, D.C., was ranked as a top hospital in the nation by the U.S. News & World Report 2025-26 Best Children’s Hospitals annual rankings. This marks the ninth straight year Children’s National has made the Honor Roll list. The Honor Roll is a distinction awarded to only 10 children’s hospitals nationwide.
Children’s National Hospital in Washington, D.C., was ranked as a top hospital in the nation by the U.S. News & World Report 2025-26 Best Children’s Hospitals annual rankings. This marks the ninth straight year Children’s National has made the Honor Roll list. The Honor Roll is a distinction awarded to only 10 children’s hospitals nationwide.

 Children’s National Hospital affiliates will participate in this year’s
Children’s National Hospital affiliates will participate in this year’s 
 Children’s National Hospital is proud to share that it has earned URAC accreditation for specialty pharmacy — its second recognition of this kind. The hospital previously received
Children’s National Hospital is proud to share that it has earned URAC accreditation for specialty pharmacy — its second recognition of this kind. The hospital previously received 












 In 2024, Children’s National Hospital continued to make remarkable strides across diverse areas of pediatric medicine, from groundbreaking technological innovations to critical health advocacy. The following compilation showcases ten significant stories that demonstrate the breadth and depth of the hospital’s impact, as featured in major national news outlets including NBC Nightly News, CNN, The Washington Post, The New York Times, NPR, The Today Show, Healio, and POLITICO. Delve into our 2024 news highlights for more.
In 2024, Children’s National Hospital continued to make remarkable strides across diverse areas of pediatric medicine, from groundbreaking technological innovations to critical health advocacy. The following compilation showcases ten significant stories that demonstrate the breadth and depth of the hospital’s impact, as featured in major national news outlets including NBC Nightly News, CNN, The Washington Post, The New York Times, NPR, The Today Show, Healio, and POLITICO. Delve into our 2024 news highlights for more.




 Children’s National Hospital in Washington, D.C., was ranked as a top hospital in the nation by the
Children’s National Hospital in Washington, D.C., was ranked as a top hospital in the nation by the 