Can complex pediatric surgery interventions be standardized to facilitate telementoring?
The study’s authors write, “These discussions are particularly relevant to surgeons in small or rural practices who provide much-needed care to underserved populations and have decreased exposure to these index cases. Conversely, in some developing countries where prevalence of rare congenital surgical conditions is higher, there is a shortage of adequately trained pediatric surgeons. Each of these scenarios involves a mismatch in experience and exposure, which can result in poor patient outcomes and inadequate healthcare delivery.”
How does a surgeon-in-training get enough exposure to rare or complex cases to serve the patients who need them? How does a practicing surgeon perform enough cases each year to maintain proficiency at such index cases?
The authors of a study in the Journal of Pediatric Surgery, including Marc Levitt, M.D., chief of the Division of Colorectal and Pelvic Reconstruction at Children’s National Hospital, write that, “These discussions are particularly relevant to surgeons in small or rural practices who provide much-needed care to underserved populations and have decreased exposure to these index cases. Conversely, in some developing countries where prevalence of rare congenital surgical conditions is higher, there is a shortage of adequately trained pediatric surgeons. Each of these scenarios involves a mismatch in experience and exposure, which can result in poor patient outcomes and inadequate healthcare delivery.”
Telementoring is one strategy being explored by the American College of Surgeons’ Telementoring Task Force initiative. Pediatric anorectal malformations (ARM), pediatric colorectal surgical procedure, posterior sagittal anorectoplasty (PSARP) were the “index” areas for the pilot study. Once the expert established the areas of great need, they will test the feasibility of a curriculum and training program using telementoring in pediatric surgery. The ACS Task Force notes that these conditions are relatively rare and require a particular skill level to manage appropriately, making them good candidates for the study.
The Journal of Pediatric Surgery study presents a process for mapping out a standardized curriculum for these procedures. First, the authors sought expert consensus on three interoperative checklists that form a de facto curriculum for teaching, learning and performing ARM and PSARP procedures. Second, a multidisciplinary team of medical educators and pediatric surgery experts drafted the checklists. The authors then sought review and input from pediatric colorectal surgery experts at 10 institutions worldwide, who comprised the study’s colorectal pediatric surgery subject matter expert panel. To be considered “expert,” participants had to meet or exceed several strict inclusion criteria related to years in practice and experience with these case types.
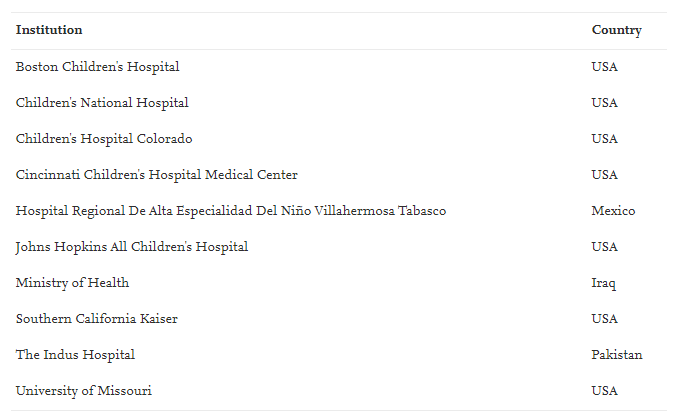
Institutions of the colorectal pediatric surgery subject matter expert panel.
The process led to a successful set of consensus documents. “To our knowledge, this is the first study to establish and standardize key intraoperative objectives using a modified-Delphi method in pediatric surgery,” the authors write. “Although this process can be quite time consuming, it provides an incredible opportunity to standardize intraoperative teaching and expectations of trainees. Future studies will expand these checklists into developing a competency assessment tool involving assessment for validity and reliability in a clinical setting to ultimately improve patient safety through standardization.”
Dr. Levitt says the overarching goal of this work is “to improve the surgical technique everywhere [to] thereby help as many kids as we can, even those we will never meet.”