With COVID-19, artificial intelligence performs well to study diseased lungs
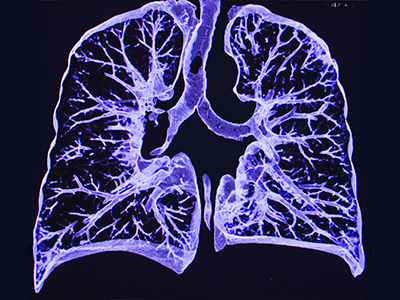
New research shows that artificial intelligence can be rapidly designed to study the lung images of COVID-19 patients.
Artificial intelligence can be rapidly designed to study the lung images of COVID-19 patients, opening the door to the development of platforms that can provide more timely and patient-specific medical interventions during outbreaks, according to research published this month in Medical Image Analysis.
The findings come as part of a global test of AI’s power, called the COVID-19 Lung CT Lesion Segmentation Challenge 2020. More than 2,000 international teams came together to train the power of machine learning and imaging on COVID-19, led by researchers at Children’s National Hospital, AI tech giant NVIDIA and the National Institutes of Health (NIH).
The bottom line
Many of the competing AI platforms were successfully trained to analyze lung lesions in COVID-19 patients and measure acute issues including lung thickening, effusions and other clinical findings. Ten leaders were named in the competition, which ran between November and December 2020. The datasets included patients with a range of ages and disease severity.
Yet work remains before AI could be implemented in a clinical setting. The AI models performed comparably to radiologists when analyzing data similar to what the algorithms had already encountered. However, the AI was less valuable when trained on fresh data from other sources during the testing phase, indicating that systems may need to study larger and more diverse data sets to meet their full potential. This is a challenge with AI that has been noted by others too.
What they’re saying
“These are the first steps in learning how we can quickly and accurately train AI for clinical use,” said Marius George Linguraru, D.Phil., M.A., M.Sc., principal investigator at the Sheikh Zayed Institute for Pediatric Surgical Innovation at Children’s National, who led the Grand Challenge Initiative. “The global interest in COVID-19 gave us a groundbreaking opportunity to address a health crisis, and multidisciplinary teams can now focus that interest and energy on developing better tools and methods.”
Holger Roth, senior applied research scientist at NVIDIA, said the challenge gave researchers around the world a shared platform for developing and evaluating AI algorithms to quickly detect and quantify COVID lesions from lung CT images. “These models help researchers visualize and measure COVID-specific lesions of infected patients and can facilitate timelier and patient-specific medical interventions to better treat COVID,” he said.
Moving the field forward
The organizers see great potential for clinical use. In areas with limited resources, AI could help triage patients, guide the use of therapeutics or provide diagnoses when expensive testing is unavailable. AI-defined standardization in clinical trials could also uniformly measure the effects of the countermeasures used against the disease.
Linguraru and his colleagues recommend more challenges, like the lung segmentation challenge, to develop AI applications in biomedical spaces that can test the functionality of these platforms and harness their potential. Open-source AI algorithms and public curated data, such as those offered through the COVID-19 Lung CT Lesion Segmentation Challenge 2020, are valuable resources for the scientific and clinical communities to work together on advancing healthcare.
“The optimal treatment of COVID-19 and other diseases hinges on the ability of clinicians to understand disease throughout populations – in both adults and children,” Linguraru said. “We are making significant progress with AI, but we must walk before we can run.”




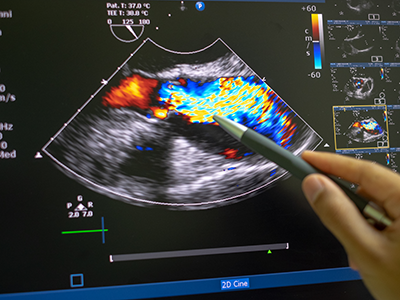





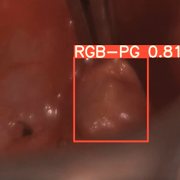
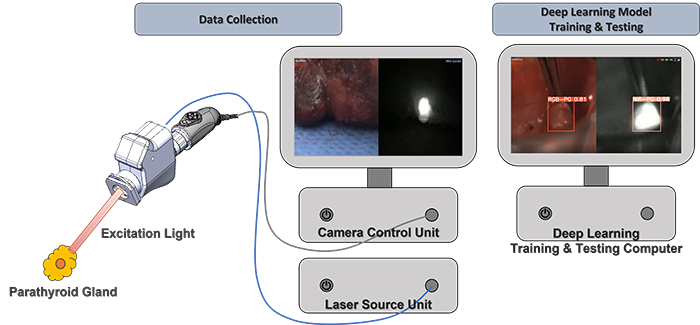
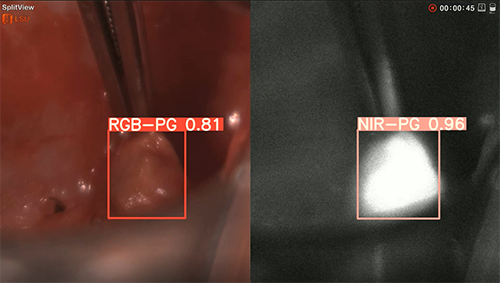 Surgeons perform approximately 150,000 thyroidectomies in the United States. Post-surgical complications from this procedure frequently occur due to the misidentification or accidental removal of healthy parathyroid glands. On average, 27% of these patients suffer from transient or permanent hypocalcemia, a condition in which the blood has too little calcium, leading to lifelong complications and socioeconomic burden.
Surgeons perform approximately 150,000 thyroidectomies in the United States. Post-surgical complications from this procedure frequently occur due to the misidentification or accidental removal of healthy parathyroid glands. On average, 27% of these patients suffer from transient or permanent hypocalcemia, a condition in which the blood has too little calcium, leading to lifelong complications and socioeconomic burden.