Breaking free of illness: Experts explore solutions for chronic pediatric disorders
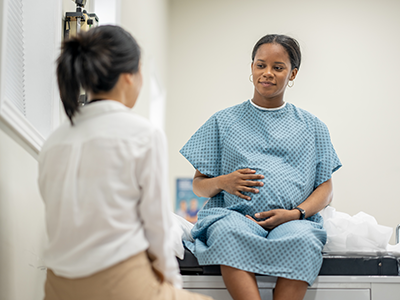
When new patients with chronic illnesses come to Roberta DeBiasi, M.D., M.S., division chief of Infectious Diseases, they are often drained of energy, far behind in school and fatigued by the lack of coordinated care among multiple specialists. She envisions a better way to care for these children: a data-driven, multidisciplinary clinic that can help diagnose and treat disorders facing chronically ill children.
In a keynote address, Dr. DeBiasi laid out her vision for improving care during the 7th annual symposium hosted by Children’s National Hospital and the National Institute of Allergy and Infectious Diseases (NIAID): “A new paradigm: Infection-associated chronic illnesses (IACI) affecting children.” Experts from across the country came together to discuss these IACIs, the importance of finding biomarkers to diagnose and monitor them, data-driven therapeutics to treat them, and the urgent need for protocols to guide physicians.
The patient benefit
A range of IACIs – including long COVID, Lyme disease, postural orthostatic tachycardia syndrome (POTS), dysautonomia and more – are stealing normal, active lifestyles from children. Dr. DeBiasi said patients need researchers who understand disease pathogenesis and have standardized disease classification to diagnose and treat these disorders. Because of the complexity of these cases, care delivery and coordination also need to change. Patients, she said, would best be served by beginning with a three-hour appointment in a multidisciplinary clinic with experts from behavioral health, rehabilitative medicine and other specialties.
“When one of these patients comes to us, we feel helpless as physicians,” Dr. DeBiasi said. “There’s no diagnostic, and we don’t know how to treat them…. It is, to me, very energizing that we’re going to be able to have a coordinated way to help these families. But to do that, we have to have standardized disease classification.”
Moving the field forward
In 2017, NIAID and Children’s National launched a clinical research partnership devoted to advancing the health of children with allergic, immunologic, auto-inflammatory and infectious diseases through collaborative research and education. The partnership — co-led by H. Clifford Lane, M.D., NIAID’s deputy director for Clinical Research and Special Projects, and Catherine Bollard, M.D., M.B.Ch.B., director of the Center for Cancer and Immunology Research at Children’s National — promotes the prevention, diagnosis, treatment and cure of these childhood diseases. Every year, the partnership organizes and funds a symposium to explore cutting-edge research and pressing issues in pediatric care.
At this year’s gathering, experts examined the specifics of various disorders, including Alexandra Yonts, M.D. She provided new data from the Children’s National Post-Covid Program and explained that patients “are clamoring” for help with symptom management.
“There have been virtually no randomized, controlled trials and very little evidence on any sort of aggressive treatments, or pharmaceutical management options, especially in the pediatric population,” Dr. Yonts said. “Upon recent attendance at some long COVID meetings, there is an expressed concern, especially among pediatric providers, about trying medications off-label in these long COVID patients.”
Miss the symposium? You can learn more about the science they explored in the symposium’s recording on topics including:
- Potential overarching mechanisms of disease, including pathogen- and host-mediated factors.
- Identifying potential biomarkers for chronic illnesses
- Treatments and multidisciplinary approaches for patients with IACIs
- Patient advocacy







































 The Children’s National Research Institute released its
The Children’s National Research Institute released its 

