New guidance to optimize blood sugar monitoring in cerebral malaria
A Children’s National Hospital research team based in Malawi pinpointed the optimal duration and frequency for monitoring the blood glucose in children with cerebral malaria, providing a roadmap to improve the treatment and outcomes for young patients diagnosed with the life-threatening disease.
Published in the American Journal of Tropical Medicine and Hygiene, the findings analyzed data from 1,674 pediatric cases to recommend the best schedule for periodic bedside point-of-care laboratory testing in children with cerebral malaria (CM). Currently, World Health Organization (WHO) guidelines state that blood glucose should be monitored in all forms of severe malaria, but they do not include advice on the timing or duration of the measurements.
Children’s National neurologist Douglas Postels, M.D., M.S., led a team of trainees from Howard University, The George Washington University, the University of Washington and Children’s National to collect and analyze patient data that led to the creation of evidence-based recommendations for glucose monitoring.
“If blood glucose in children with severe malaria is too low, the child is at high risk of death,” Dr. Postels said. “What we found in this research study is both interesting and important, and we hope our study results will help the WHO in creating evidence-based guidelines for blood glucose monitoring in children with cerebral malaria.”
The big picture
In 2021, 247 million people contracted malaria worldwide, killing some 619,000 primarily in Africa. Almost 80% were children under 5 years old, making it one of the most virulent pediatric diseases in the world. Many who survive experience significant neurologic, cognitive and behavioral morbidities.
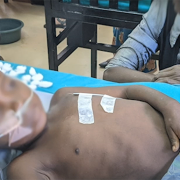
Dr. Postels works at Queen Elizabeth Central Hospital in Blantyre, Malawi, caring for patients on the Pediatric Research Ward and conducting research aimed at improving outcomes. The clinical team works without access to many medical tools that are considered standard throughout more advanced economies. Yet this team has one of the lowest mortality rates for cerebral malaria across Africa, thanks to their ongoing research to better understand the pathophysiology of malaria and improve its treatment.
The challenges are immense: During COVID-19, they battled supply chain issues that frustrated repairs on an aging MRI scanner. After the second tropical cyclone struck in the last two years, Blantyre was left without power for a week and without water for a month.
“You can imagine trying to run a hospital with no water,” Dr. Postels said. “During Cyclone Freddy, it was raining like crazy, and people were collecting water in bins—anything they could collect it in — to use for handwashing, as well as trying to clean instruments and supplies.”
What they’re saying
Using evidence-based guidelines to optimize care becomes important in sub-Saharan Africa, where resources are scarce. Running laboratory-based blood studies frequently is an inefficient use of supplies and laboratory reagents. Results of point-of-care testing are also available more rapidly and at less cost than studies performed in hospital labs.
An accompanying editorial in the journal said the new research on glucose monitoring in cerebral malaria “provides valuable data that could help clinicians in resource-limited settings improve CM management with more efficient use of available resources.” The work is increasing calls for further study and updates to international guidelines.
The bottom line
According to the team’s analysis, blood glucose should be measured in children with CM on admission and every six hours for the first 24 hours. If all results in the first 24 hours are normal, clinicians can stop testing. If any blood sugar levels in the first 24 hours are low, the patient’s blood glucose should be checked for another 24 hours.
“This testing strategy captures 100% of the children who have a glucose level of 2.2 mmol/L or less, the definition of hypoglycemia in severe malaria,” Dr. Postels said. “We want to do enough, but not too much.”
The overarching goal for Dr. Postels and the trainees who join him in Blantyre is improving care. “If we can help clinicians better care for children with cerebral malaria, then hopefully we can make a small contribution to decreasing the death rate and improve neurologic outcomes of the children who survive,” he said. “That’s my hope.”