Concussion treatments for children need more priority

Concussion treatments for children have continued to evolve but ultimately, need more priority.
The Sport Concussion Assessment Tool (SCAT) tools are used worldwide for children, adolescents and adults to assist in the evaluation and management of sport-related concussions (SRC). The SCAT tools have evolved over time based on clinical findings, clinician input, scientific investigations and systematic reviews of the literature, as recently noted in a paper published by the British Journal of Sports Medicine. It is critically important to identify and diagnose a concussion as early as possible and track its recovery with reliable and valid tools across the full age span from young child to adult.
This systematic review occurs only every four years to summarize the current literature on concussions. A team of leading researchers including Gerard Gioia, Ph.D., director of Safe Concussion Outcome, Recovery and Education (SCORE) Program at Children’s National Hospital and co-author of the paper, found that the SCAT measure has been used mostly with adult and adolescent SRCs but not with children ages 5-12 years.
The tools are helpful to diagnose and track recovery in children, adolescents and adults only up to three days post-injury. Their lack of sensitivity after this time resulted in the recommendation for a new complementary tool, the Sport Concussion Office Assessment Tool (SCOAT), which Dr. Gioia assisted in developing. One of the SCOAT measures – known as SCOAT6 – is the PACE-Self Efficacy Scale, developed by Dr. Gioia, Christopher Vaughan, Psy.D., neuropsychologist, and other colleagues at Children’s National. This measure assesses and tracks the confidence of children and adolescents in managing their recovery, an important component that underlies successful recovery.
We spoke more with Dr. Gioia about the recent advancements in concussion recommendations.
Q: What’s been the hold-up in the field with respect to children and adolescents?
A: A specific hold-up is that the venues where a sport-related concussion can occur do not have the athletic health professionals or researchers available to identify the injuries early or conduct specific research on their manifestations. Pre-adolescent children are typically seen in emergency rooms or their primary care physicians’ offices and are, therefore, not available to be studied and monitored. The venues for older athletes include high schools, colleges and professional sports stadiums with designated athletic health professionals. We need to find better ways to identify pre-adolescent athletes to understand their diagnostic and recovery needs.
Q: Why is it important to update the literature?
A: The periodic work of the Concussion in Sport Group helps to provide an updated understanding of the injury and improve the tools used to diagnose and treat SRC early in the process and to develop the necessary tools beyond this initial period. Its results have made recommendations for improvement given that some measures are not as sensitive to the injury and need to be modified. For example, tools that need further study and revision include the balance exam, word-list learning and memory measures. It calls for improvements in these assessment tools, which will better define and diagnose the injury.
Q: How will this work benefit patients?
A: Improved sensitivity of the acute measure and a new follow-up assessment measure will result in improved treatment recommendations for patients. Recognition of the dearth of data on SRC in children ages 5-12 will hopefully stimulate efforts to generate this research. The team at Children’s National plans to address this need through our research.
Q: What are some of the new updates that excite you about the future of concussion care?
A: Being able to define the current state of the literature and identify the needs, particularly with children, is exciting. It also stimulates our work at Children’s National to continue to improve our understanding and clinical care of children and adolescents with sport-related concussions.
I have been an active member of the Concussion in Sport Group since 2008 as one of the few pediatric concussion specialists involved for this long. We continue to lead in our clinical research that builds better measures and tools to identify, diagnose and treat these injuries in children.






 Children’s National Hospital announced a $96 million investment from an anonymous donor family to transform rare childhood brain tumor research and care. The donation, which strengthens our globally recognized leadership in the field, is one of the largest in the hospital’s history.
Children’s National Hospital announced a $96 million investment from an anonymous donor family to transform rare childhood brain tumor research and care. The donation, which strengthens our globally recognized leadership in the field, is one of the largest in the hospital’s history.
 Children’s National Hospital in Washington, D.C., was ranked #5 in the nation on the U.S. News & World Report 2023-24 Best Children’s Hospitals annual rankings. This marks the seventh straight year Children’s National has made the Honor Roll list. The Honor Roll is a distinction awarded to only 10 children’s hospitals nationwide.
Children’s National Hospital in Washington, D.C., was ranked #5 in the nation on the U.S. News & World Report 2023-24 Best Children’s Hospitals annual rankings. This marks the seventh straight year Children’s National has made the Honor Roll list. The Honor Roll is a distinction awarded to only 10 children’s hospitals nationwide.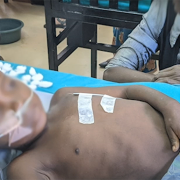

 Children’s National Hospital named
Children’s National Hospital named 









 A new validated self-report tool called the Gender Self-Report provides researchers a way to characterize the gender of research participants beyond their binary designated sex at birth.
A new validated self-report tool called the Gender Self-Report provides researchers a way to characterize the gender of research participants beyond their binary designated sex at birth.