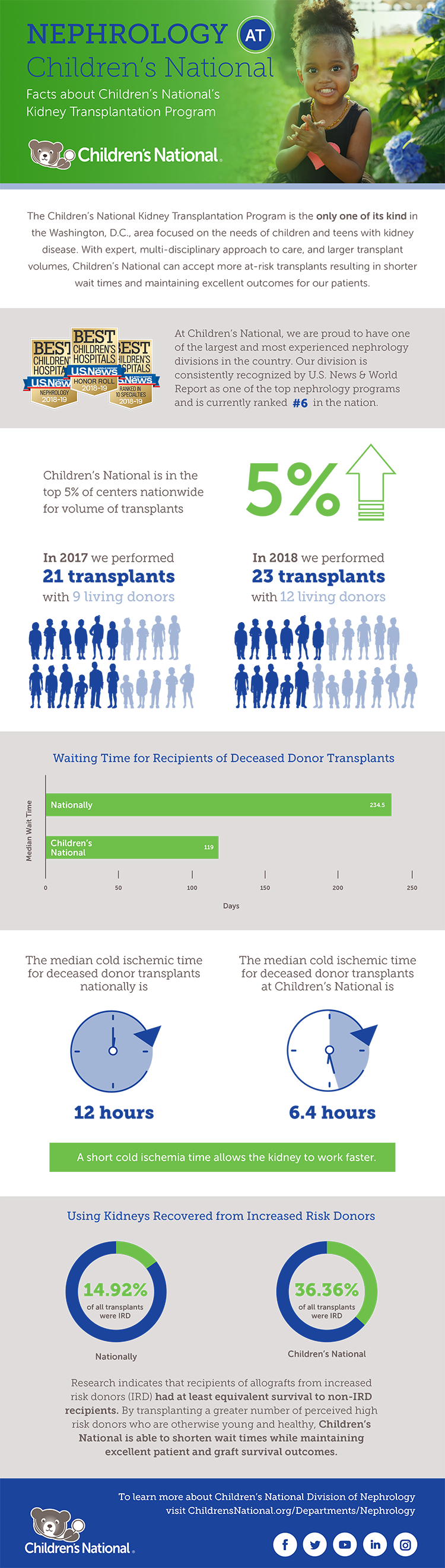
Kofi Essel, M.D., M.P.H. and Ankoor Shah, M.D., M.B.A., M.P.H., named among 40 Under 40 Leaders in Minority Health

Ankoor Shah, M.D., M.B.A., M.P.H., and Kofi Essel, M.D., M.P.H., were named 40 Under 40 Leaders in Minority Health.
Two doctors from Children’s National Health System are among the recipients of the 40 Under 40 Leaders in Minority Health award by the National Minority Quality Forum (NMQF) for 2019. Kofi Essel, M.D., M.P.H., is a pediatrician, Ankoor Shah, M.D., M.B.A., M.P.H., is the medical director of the IMPACT DC Asthma Clinic and also a pediatrician at Children’s National.
Founded in 1998, the NMFQ is dedicated to ensuring that high-risk racial and ethnic populations and communities receive optimal health care. The 40 individuals selected for this award represent the next generation of thought leaders in reducing health disparities.
Dr. Kofi Essel is a pediatrician at the Children’s Health Center Anacostia. His focus and research has been around health equity, obesity, food insecurity and nutrition.
“Hunger strikes so many of our families,” says Dr. Essel, “In D.C., we were number one in the nation for having the highest rate of food hardship in households with children.”
Dr. Essel is involved with many organizations and initiatives that raise awareness about hunger and how much of an issue it is. He strives to be a partner for the families that he serves, many of whom are in the fight against obesity, and works alongside them to improve their overall health.
“It’s a huge honor to receive recognition from this national organization,” says Dr. Kofi Essel, “Ultimately, it allows us to have a bit more of a platform to continue to advance some of the great work we’re doing with health disparities.”
Dr. Ankoor Shah is the medical director for IMPACT DC asthma clinic and a pediatrician at the Children’s Health Center at THEARC. His focus includes improving pediatric population health and reducing child health asthma disparities.
“Through the coordination of the best in class care at Children’s National with amazing on the ground community partners, we have been able to transform the lives of the most at-risk children with asthma” says Dr. Shah.
Dr. Shah collaborates with organizations to improve the outcomes of kids with asthma by targeting intervention in high-risk areas.
“This award is recognition of the great work we’re doing in terms of improving asthma health in high-risk child populations throughout the District of Columbia.”
Both Dr. Essel and Dr. Shah are from Arkansas, attended Emory University and they did their residency together at Children’s National.
Congratulations to these wonderful doctors and leaders for receiving this award.
The 40 Under 40 recipients received their awards at the 2019 NMQF Leadership Summit on Health Disparities and CBC Spring Health Braintrust Gala Dinner on April 9.