Children’s National Hospital and NIAID launch large study on long-term impacts of COVID-19 and MIS-C on kids
Up to 2,000 children and young adults will be enrolled in a study from Children’s National Hospital in collaboration with the National Institute of Allergy and Infectious Diseases (NIAID) that will examine the long-term effects of COVID-19 and multisystem inflammatory syndrome in children (MIS-C) after these patients have recovered from a COVID-19 infection.
This $40 million multi-year study will provide important information about quality of life and social impact, in addition to a better understanding of the long-term physical impact of the virus, including effects on the heart and lung. The researchers hope to detail the role of genetics and the immune response to COVID-19, so-called “long COVID” and MIS-C, including the duration of immune responses from SARS-CoV-2, the virus that causes COVID-19. It is fully funded by a subcontract with the NIH-funded Frederick National Laboratory for Cancer Research operated by Leidos Biomedical Research, Inc.
“We don’t know the unique long-term impact of COVID-19 or MIS-C on children so this study will provide us with a critical missing piece of the puzzle,” says Roberta DeBiasi, M.D., M.S., chief of the Division of Pediatric Infectious Diseases at Children’s National and lead researcher for this study. “I am hopeful that the insights from this enormous effort will help us improve treatment of both COVID-19 and MIS-C in the pediatric population both nationally and around the world.”
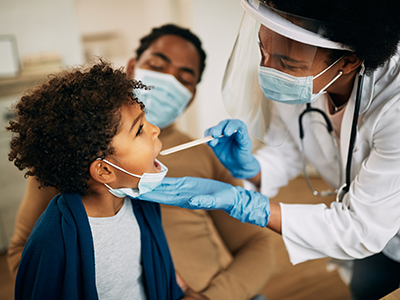
Over the past year, more than 3.6 million children have tested positive for SARS-CoV-2 and over 2,800 cases of MIS-C have been reported throughout the U.S. While the vast majority of children with primary SARS-CoV-2 infection may have mild or no symptoms, some develop severe illness and may require hospitalization, including life support measures. In rare cases, some children who have previously been infected or exposed to someone with SARS-CoV-2 have developed MIS-C, a serious condition that may be associated with the virus. MIS-C symptoms can include fever, abdominal pain, bloodshot eyes, trouble breathing, rash, vomiting, diarrhea and neck pain, and can progress to shock with low blood pressure and insufficient cardiac function. Long COVID is a wide range of symptoms that can last or appear weeks or even months after being infected with the virus that causes COVID-19.
The study is designed to enroll at least 1,000 children and young adults under 21 years of age who have a confirmed history of symptomatic or asymptomatic SARS-CoV-2 infection or MIS-C. Participants who enroll within 12 weeks of an acute infection will attend study visits every three months for the first six months and then every six months for three years. Participants who enroll more than 12 weeks after acute infection will attend study visits every six months for three years. The study will also enroll up to 1,000 household contacts to serve as a control group, and up to 2,000 parents or guardians (one parent per participant) will complete targeted questionnaires.
“The large number of patients who will be enrolled in this study should provide us with a truly comprehensive understanding of how the virus may continue to impact some patients long after the infection has subsided,” says Dr. DeBiasi.
The study primarily aims to determine incidence and prevalence of, and risk factors for, certain long-term medical conditions among children who have MIS-C or a previous SARS-CoV-2 infection. The study will also evaluate the health-related quality of life and social impacts for participants and establish a biorepository that can be used to study the roles of host genetics, immune response and other possible factors influencing long-term outcomes.
Children’s National was one of the first U.S. institutions to report that children can become very ill from SARS-CoV-2 infection, despite early reports that children were not seriously impacted. In studies published in the Journal of Pediatrics in May of 2020 and June of 2021, Children’s National researchers found that about 25% of symptomatic COVID patients who sought care at our institution required hospitalization. Of those hospitalized, about 25% required life support measures, and the remaining 75% required standard hospitalization. Of patients with MIS-C, 52% were critically ill.
Study sites include Children’s National Hospital inpatient and outpatient clinics in the Washington, D.C. area, and the NIH Clinical Center in Bethesda, Maryland.
Those interested in participating should submit this form. You will then be contacted by a study team member to review the study details and determine whether you are eligible to participate.
You can find more information about the study here.