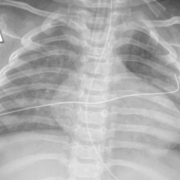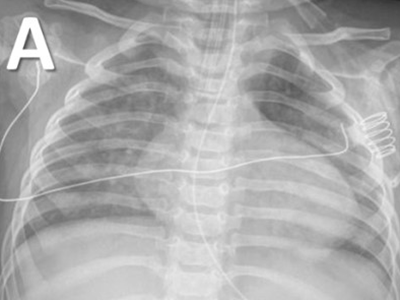
Asthma, which is the most common chronic pediatric lung disease, has traditionally been defined as a syndrome of airway inflammation characterized by clinical symptoms of cough, wheezing, and shortness of breath. The complex and diverse nature of asthma has led to its classification as a syndrome or a constellation of symptoms and signs rather than a single diagnosis.
A review article published last month in Pediatric Research summarizes recent advances in defining asthma as a disease in children and demonstrates the need for even more nuanced definitions of an illness that affects an estimated 6 million youngsters in the United States.
More precise definitions of asthma will lead to more accurate diagnoses, better care for patients, and thereby fewer visits to the emergency department, says senior author Deepa Rastogi, M.D., M.S., co-director of Children’s National Hospital’s Severe Asthma Program and Associate Professor, Pediatrics and Genomics and Precision Medicine, George Washington University School of Medicine and Health Sciences.
The review — “Defining pediatric asthma: phenotypes to endotypes and beyond” — details current knowledge of asthma phenotypes and endotypes and recommends an approach to endotyping asthma that may be useful for defining asthma for clinical care as well as for future research studies in the realm of personalized medicine for asthma.
Asthma, which is the most common chronic pediatric lung disease, has traditionally been defined as a syndrome of airway inflammation characterized by clinical symptoms of cough, wheezing, and shortness of breath. The complex and diverse nature of asthma has led to its classification as a syndrome or a constellation of symptoms and signs rather than a single diagnosis.
The review summarizes key biomarkers that distinguish childhood asthma subtypes. While atopy and its severity are important features of childhood asthma, there is evidence to support the existence of a childhood asthma endotype distinct from the atopic endotype.
The article also summarizes a clinical approach that includes existing measures of airway-specific and systemic measures of atopy, coexisting morbidities, and disease severity and control, in the definition of childhood asthma, to empower health care providers to better characterize the disease burden in children.
“For health care providers, asking the right set of questions and doing the right testing will define the disease severity and control, which may get 90% of the disease under control,” says Rastogi. “This approach will allow health care providers to identify those children with severe asthma who would benefit from specialty intervention by a pediatric allergist or pulmonologist.”
At the Children’s National IMPACT DC Asthma Clinic, a team of providers that includes Rastogi, is practicing cutting-edge medicine that incorporates several concepts summarized in the review. The award-winning pediatric program is improving care and outcomes for children with severe asthma who have recently been to the emergency room, have been hospitalized for asthma, or generally have trouble controlling the disease.
When a child and their parents visit the clinic, they meet with clinicians who conduct a detailed medical consultation and provide a unique care plan for the patient. The team then coordinates treatment with the child’s primary care provider, school nurse and others involved in their care.
“Identifying the labile child using the endotyping tools allows us to intervene in a timely manner,” says Rastogi. “The article highlights the need to define asthma at the clinical level utilizing tools that already exist while also detailing areas where more research is needed.”
In its examination of how the definition of asthma has evolved over time, the review notes that the 2007 National Heart Lung and Blood Institute Guidelines for the Diagnosis and Management of Asthma introduced severity and control classifications. But in 2010, the World Health Organization (WHO) identified the lack of standardized use of the classifications, noting that the terms were being used interchangeably.
The WHO also emphasized the need for a uniform definition for severe asthma that would differentiate treatment-resistant severe asthma from difficult-to-treat severe asthma, based on the high doses of inhaled corticosteroids and systemic corticosteroids required to achieve asthma control.
In 2019, the Global Initiative for Asthma (GINA) report included umbrella definitions of asthma — “a heterogeneous disease, usually characterized by chronic airway inflammation defined by the history of respiratory symptoms such as wheeze, shortness of breath, chest tightness, and cough that vary over time and in intensity, together with variable expiratory airflow limitations.”
While these definitions of asthma account for the varied disease presentation, they are again limited in defining early childhood asthma, since tests of airflow obstruction, such as spirometry (which measures lung function) cannot be reliably performed prior to the age of 5.
In the review, Rastogi and her co-authors encourage clinicians to uniquely define asthma for each child based on:
- the age of onset (early vs. late)
- the severity and control of disease (per the latest NHLBI guidelines as intermittent, mild, moderate or severe persistent)
- the predominant form of immune response (allergic vs. nonallergic)
- the inciting trigger (exercise vs. viral induced)
- the pattern of pulmonary function deficits and
- the presence of comorbidities
Better controlling childhood asthma could lead to reduced rates of adult asthma, says Rastogi.
“I’d love to be in a place where we can phenotype pediatric asthma with genetic, molecular, and biomarker details that directly guide targeted therapy,” says Rastogi. “That’s where oncology is now. That’s where I’d like to be with childhood asthma.”