Children’s National Hospital ranked #5 in the nation on U.S. News & World Report’s Best Children’s Hospitals Honor Roll
 Children’s National Hospital in Washington, D.C., was ranked #5 in the nation on the U.S. News & World Report 2023-24 Best Children’s Hospitals annual rankings. This marks the seventh straight year Children’s National has made the Honor Roll list. The Honor Roll is a distinction awarded to only 10 children’s hospitals nationwide.
Children’s National Hospital in Washington, D.C., was ranked #5 in the nation on the U.S. News & World Report 2023-24 Best Children’s Hospitals annual rankings. This marks the seventh straight year Children’s National has made the Honor Roll list. The Honor Roll is a distinction awarded to only 10 children’s hospitals nationwide.
For the thirteenth straight year, Children’s National also ranked in all 10 specialty services, with eight specialties ranked in the top 10 nationally. In addition, the hospital was ranked best in the Mid-Atlantic for neonatology, cancer, neurology and neurosurgery.
“Even from a team that is now a fixture on the list of the very best children’s hospitals in the nation, these results are phenomenal,” said Kurt Newman, M.D., president and chief executive officer of Children’s National. “It takes a ton of dedication and sacrifice to provide the best care anywhere and I could not be prouder of the team. Their commitment to excellence is in their DNA and will continue long after I retire as CEO later this month.”
“Congratulations to the entire Children’s National team on these truly incredible results. They leave me further humbled by the opportunity to lead this exceptional organization and contribute to its continued success,” said Michelle Riley-Brown, MHA, FACHE, who becomes the new president and CEO of Children’s National on July 1. “I am deeply committed to fostering a culture of collaboration, empowering our talented teams and charting a bold path forward to provide best in class pediatric care. Our focus will always remain on the kids.”
“I am incredibly proud of Kurt and the entire team. These rankings help families know that when they come to Children’s National, they’re receiving the best care available in the country,” said Horacio Rozanski, chair of the board of directors of Children’s National. “I’m confident that the organization’s next leader, Michelle Riley-Brown, will continue to ensure Children’s National is always a destination for excellent care.”
The annual rankings are the most comprehensive source of quality-related information on U.S. pediatric hospitals and recognizes the nation’s top 50 pediatric hospitals based on a scoring system developed by U.S. News.
“For 17 years, U.S. News has provided information to help parents of sick children and their doctors find the best children’s hospital to treat their illness or condition,” said Ben Harder, chief of health analysis and managing editor at U.S. News. “Children’s hospitals that are on the Honor Roll transcend in providing exceptional specialized care.”
The bulk of the score for each specialty service is based on quality and outcomes data. The process includes a survey of relevant specialists across the country, who are asked to list hospitals they believe provide the best care for patients with the most complex conditions.
The eight Children’s National specialty services that U.S. News ranked in the top 10 nationally are:
- Neonatology (No. 2), led by Division Chief Billie Lou Short, M.D.
- Neurology and Neurosurgery (No. 3), led by Division Chiefs William D. Gaillard, M.D., and Robert F. Keating, M.D.
- Cancer (No. 4), led by Division Chief Jeffrey S. Dome, M.D., Ph.D.
- Nephrology (No. 6), led by Division Chief Marva Moxey-Mims, M.D.
- Orthopedics (No. 7), led by Division Chief Matthew Oetgen, M.D., M.B.A.
- Diabetes and Endocrinology (No. 7), led by Division Chief Andrew Dauber, M.D., MMSc.
- Gastroenterology and GI surgery (No. 8), led by Division Chief Ian Leibowitz, M.D.
- Pulmonology and Lung Surgery (tied for No. 9), led by Division Chief Anastassios Koumbourlis, M.D., M.P.H.
The other two specialties ranked among the top 50 were cardiology and heart surgery, and urology.









 A clinical trial testing a new drug to increase growth in children with short stature. The first ever high-intensity focused ultrasound procedure on a pediatric patient with neurofibromatosis. A low dose gene therapy vector that restores the ability of injured muscle fibers to repair. These were among the most popular articles we published on Innovation District in 2022. Read on for our full top 10 list.
A clinical trial testing a new drug to increase growth in children with short stature. The first ever high-intensity focused ultrasound procedure on a pediatric patient with neurofibromatosis. A low dose gene therapy vector that restores the ability of injured muscle fibers to repair. These were among the most popular articles we published on Innovation District in 2022. Read on for our full top 10 list.

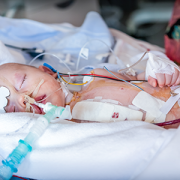
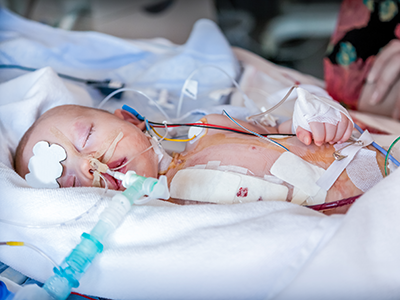









 In 1984, Children’s National Hospital became the first children’s hospital to offer Extracorporeal Membrane Oxygenation (ECMO) and remains one of the largest ECMO programs in the nation, led by
In 1984, Children’s National Hospital became the first children’s hospital to offer Extracorporeal Membrane Oxygenation (ECMO) and remains one of the largest ECMO programs in the nation, led by