First-of-its-kind study on impacts of Lyme disease in pregnancy and infant development
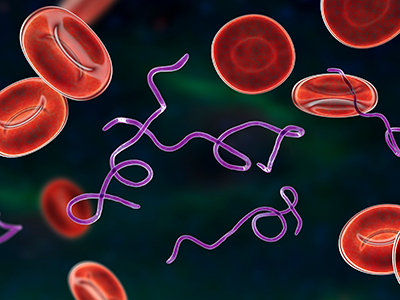
Lyme disease is caused by the bacterium Borrelia burgdorferi.
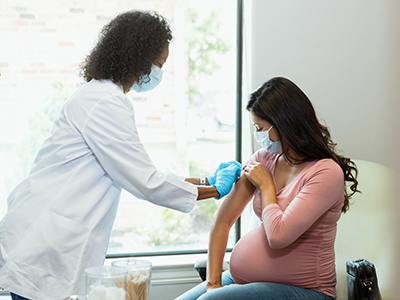
Understanding the effects of Lyme disease on the developing fetal brain is essential to ensure timely prenatal and postnatal treatments to protect the fetus and newborn. In response to this need, Children’s National Hospital is leading a pilot study to establish the groundwork needed for a larger study to determine the effect of in utero exposure to Lyme disease on pregnancy and early childhood neurodevelopmental outcomes.
Why it’s important
“Insect-borne illnesses have more than doubled during the last twenty years as a result of multiple factors including environmental changes,” says Sarah Mulkey, M.D., Ph.D., principal investigator of the study and prenatal-neonatal neurologist at Children’s National Hospital. Dr. Mulkey is the Co-Director of the Congenital Infection Program at Children’s National Hospital and has led a long-term child outcome study of the mosquito-borne Zika virus infection in pregnancy and impacts on child neurodevelopment. She is now adding Lyme disease to her work on pregnancy and child outcomes. Lyme disease is transmitted to humans via an infected tick and can be acquired throughout much of the United States. “Very little is known about Lyme disease in pregnancy and if and how it may affect the fetus and impact child neurodevelopment,” said Dr. Mulkey.
This pilot study is funded by the Clinical Trials Network for Lyme and other Tickborne Diseases (CTN), supported by the Steven and Alexandra Cohen Foundation. Roberta DeBiasi, M.D., M.S., division chief of infectious diseases at Children’s National, is a CTN Node Principal Investigator. The study team at Children’s National works closely with members of the CTN as well as other Lyme disease-focused organizations and nonprofits to make sure that the pilot study addresses Lyme disease advocates’ research priorities in a scientifically rigorous way. “This is an important opportunity for us to engage with advocacy groups and others who have been stressing the need for this type of research for decades,” says Meagan Williams, M.S.P.H., C.C.R.C., the senior research coordinator for the study. “We know how important it is to maintain a patient-centered and trauma-sensitive lens in our work with families impacted by Lyme disease during pregnancy. We’ve been working hard to build this study in a way that centers our participants’ lived experiences and focuses on the topics they find important. We’re very grateful to have the support of Lyme disease focused organizations and advocates as we embark on this study because they know and have expressed exactly where the gaps are in the literature. It’s our job to do the work to fill those gaps.”
The big picture
This pilot study aims to build upon existing research, case studies and advocacy to assess developmental and other family impacts of Lyme disease exposure during pregnancy.
Especially as tick season begins in Washington, D.C., and surrounding regions, the investigators are determined to make sure that all eligible people diagnosed with Lyme disease during their pregnancy are aware of the study and have the opportunity to participate. Pregnant volunteers can sign up for participation in the study here. Volunteers may be eligible to join if they are currently pregnant, live in the U.S. or Canada and were diagnosed with Lyme disease during pregnancy or have post-treatment Lyme disease syndrome (PTLDS).
Anyone interested in sharing information about the study with their clients or colleagues may email mewilliams@childrensnational.org for access to the team’s recruitment toolkit that includes flyers, FAQs and other resources. “We have resources available for clinicians, public health professionals, friends and family members and anyone else who may be able to help us identify participants and spread the word about this important study,” Williams says.
The study is registered on ClinicalTrials.gov (NCT06026969). If you have questions about the study, please reach out to Meagan at mewilliams@childrensnational.org or email cnhlymestudy@gmail.com.