Horizon Pharma gifts $3M to establish Horizon Pharma Clinical Care Endowment at Children’s National Rare Disease Institute

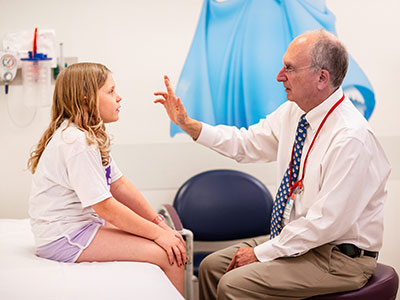
“Patients and families with rare conditions deserve to be treated in a place with the medical knowledge to provide quick, clear answers and the expert care they need,” says Marshall Summar, M.D., director of the CNRDI.
Children’s National Health System and Horizon Pharma plc are pleased to announce the creation of the Horizon Pharma Clinical Care Endowment, the first clinical team endowment at the Children’s National Rare Disease Institute (CNRDI). The endowment is made possible by a generous six-year, $3 million commitment from Horizon Pharma USA, Inc., a wholly owned subsidiary of Horizon Pharma plc –a biopharmaceutical company dedicated to improving the lives of people living with rare diseases.
“Patients and families with rare conditions deserve to be treated in a place with the medical knowledge to provide quick, clear answers and the expert care they need,” says Marshall Summar, M.D. , director of the CNRDI. “We are grateful for Horizon and their support of our mission to make the Children’s National Rare Disease Institute that place. This endowment will support a dedicated team that can provide optimal, comprehensive care to more patients and ensure that families have a trusted source for all aspects of their health care.”
The Horizon Pharma Clinical Care Endowment will generate revenue annually, providing stable support for an expert care team at the CNRDI. Each team will be comprised of a clinical geneticist and support team members – such as genetic counselors, nutritionists and social workers – all specializing in the care of children with rare disease.
The long-term support provided by the Horizon Pharma Clinical Care Endowment will give the CNRDI a firm foundation for treating patients earlier, more consistently and over the course of their lifetime. Horizon’s commitment marks the first donor-funded endowment at the CNRDI.
Currently, it is estimated that one in 10 Americans has a rare disease – approximately 80 percent of which are genetically based. Additionally, the NIH reports that more than 80 percent are childhood diseases, and more than 25 percent of children admitted to pediatric hospitals have a rare disease.
The CNRDI is a first-of-its-kind center focused exclusively on advancing the care and treatment of children and adults with rare genetic diseases. It is the first National Organization for Rare Disorders (NORD) Center of Excellence and aims to provide a medical home for patients and families seeking the most advanced care and expertise for rare genetic conditions that remain largely unknown to the general medical community.