Children’s National leads first system-wide asthma social needs screening

Children’s National launches the first system-wide asthma social needs screening program, asking families directly about the support they need most.
Asthma is one of the most common chronic conditions in children. While medications and inhalers are essential, many families face challenges that make managing asthma even harder. Problems like housing instability, lack of transportation or difficulty paying for medications can all affect a child’s ability to stay healthy and avoid emergency visits.
A new study from Children’s National Hospital is transforming the way hospitals think about asthma care. Led by Rachel Margolis, PhD, LICSW, the project introduced the first health system-wide screening program focused specifically on the social needs of children with asthma. Unlike traditional social risk screenings that rely on general checklists, this new approach centers on what families say they need most.
The team created a “social needs checklist” to ask families directly what they need help with, rather than just identifying potential risks. This might sound like a small change, but it represents a major shift in how hospitals support families. By putting family voices at the center of care, the program empowers parents and caregivers to share their priorities and receive help that is most meaningful to them.
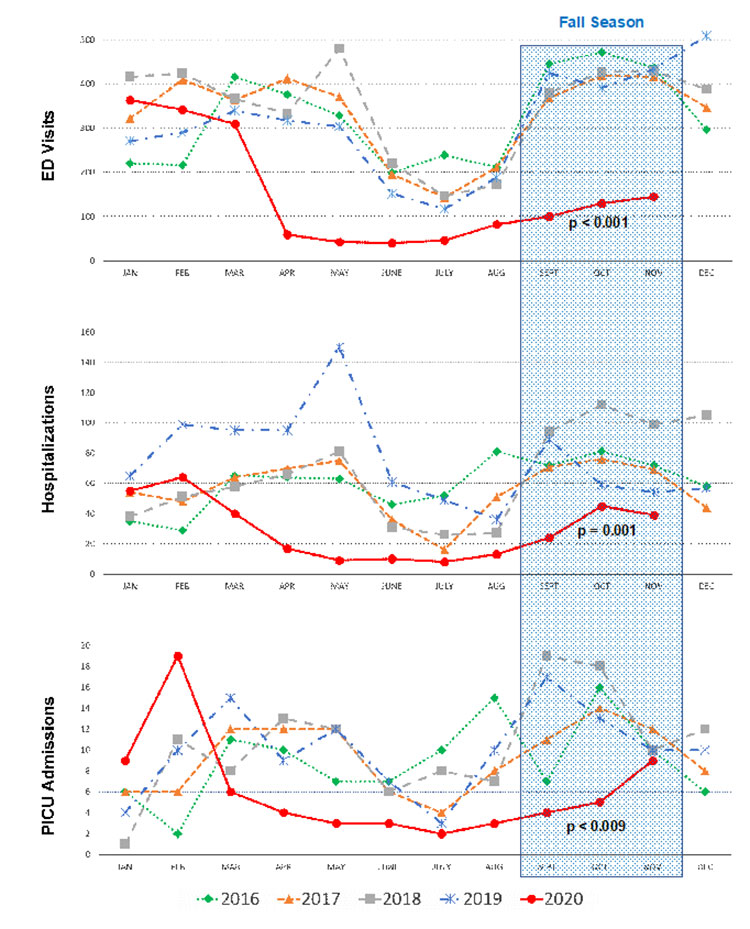
To test this new tool, the team expanded screening into three key areas at Children’s National: the Pediatric Intensive Care Unit (PICU), the severe asthma clinic and the emergency department at United Medical Center. These are places where children with the most severe asthma symptoms often go for care. The study set out to understand how screening could work in each setting, whether families and staff would accept it and what kinds of social needs families would report.
The results were eye opening. Families across all settings were open to sharing their needs and felt comfortable discussing them with care teams. In the PICU, the program was especially successful because of strong support from leadership and dedicated staff who helped keep the screening process running smoothly. Perhaps most important, the study found that 42.3% of families requested help with at least one social need. This high level of need highlights just how many families are facing serious challenges with potential impacts on a child’s asthma and overall health.
Social factors play a powerful role in asthma management. Where a child lives, whether a family can afford medications and how easily they can get to follow-up appointments can all affect whether asthma stays under control or turns into an emergency. By focusing on what families identify as their top needs, hospitals can connect them to the right community resources, improve asthma outcomes and help keep children healthier at home.
Children’s National is leading the way with this asthma-specific, system-wide approach to social needs screening. This program sets a new standard by listening directly to families and acting on their priorities. The interdisciplinary Asthma Social Support and Intervention Screen Tool (ASSIST) workgroup that launched this study continues to meet regularly, working on ways to improve and expand the program even further. Their efforts include strengthening partnerships with community organizations and finding new ways to support families beyond the hospital walls.
Looking ahead, the team hopes this model will inspire other hospitals to adopt similar strategies for asthma and other chronic conditions. By putting families at the center and addressing social needs as part of medical care, hospitals can help more children breathe easier and live healthier, more stable lives.
Read the full study, “A Health System-Wide Approach to Addressing Unmet Social Needs Among Children With Asthma”, in the American Academy of Pediatrics publication, Hospital Pediatrics.
Additional authors from Children’s National include Shayla Stringfield, MPH, CHES; Taylor Brewer, MD; Andrea Williams, BSW; Terry Dean, MD, PhD; Kitman Wai, MD; Gayle Gilmore, MSSA, LICSW; Parisa Kaviany, MD; Kavita Parikh, MD, MSHS and Shilpa J. Patel, MD, MPH.