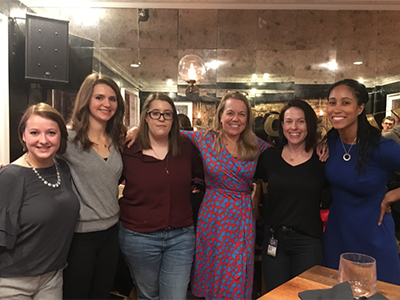The new laboratory space includes floor-to-ceiling windows and brand new, state-of-the-art GMP lab suites.
Since Children’s National Hospital began its pediatric cellular therapy program in 2013, it has received more than $5 million in annual funding, treated over 200 patients, manufactured more than 400 cell-based products and supported over 25 clinical trials.
One of the in-house programs supporting this work is the Good Manufacturing Practices (GMP) facility. Patrick Hanley, Ph.D., chief and director of the cellular therapy program at Children’s National and leader of the GMP laboratory, explained that the first patient received a dose of less than 10 million cells in May 2014. Fast forward to now, the lab uses liters of media, automated bioreactors and multiple staff, making upwards of 12 billion cells per run — a growing production scale that enables many different options. Using cells as an off-the-shelf technology is one of those.
The cell therapy program exports these off-the-shelf products beyond Children’s National to make them available for kids across the country. Catherine Bollard, M.D., MBChB., director of the Center for Cancer and Immunology Research at Children’s National, and Michael Keller, M.D., director of the Translational Research Laboratory in the Program for Cell Enhancement and Technologies for Immunotherapy (CETI) at Children’s National, each led clinical trials with hospitals across the United States, including the first-ever cellular therapy clinical trial run through the Children’s Oncology Group.
To meet the high demand for cell therapy trials at Children’s National, the GMP lab moved to a larger space, doubling the team’s capacity to produce alternative treatment options for patients and facilitate the lab’s ability to support clinical divisions throughout the hospital.
The GMP lab is exploring how to make cell products more consistent — regardless of patient-to-patient variability. They are also hoping to delineate the characteristics that ensure quality cell products, educate other facilities, enhance the overall knowledge of how to safely manufacture these products and make these technologies more available and affordable to the patients who need them.
Among Hanley’s many goals for the GMP lab, one is to improve the transition from when an investigator discovers a product in the translational research lab to when it is manufactured for patients.
“To improve this transition, we have started a process development team that will learn the process alongside the research team, replicate it, and then train the staff who manufacture the product for patients,” said Hanley. “In addition to providing a better training opportunity for the manufacturing staff, it allows us to work with the investigators earlier on to identify changes that will need to be made to translate the products to patients, ultimately resulting in safer, more potent immunotherapy products.”
While cell therapy has seen increased interest in the last 10 years, there are still some challenges in the field, given that it is not as mature as other scientific areas. The lack of trained staff, scalability of cell and gene therapy, the variability between patients and products, delayed FDA approvals and rejection of licensing applications for cell therapy products — are barriers that scientists and companies often face.
“Each of us has a unique immune system, and that means that if we try and make a product from it, it will not behave like any other, so the number of cells, the potency the alloreactivity — it is all different,” said Hanley. “T-cells are a living drug that expand in the body at different rates, are composed of different types of T-cells, and release different cytokines and in different amounts.”
This all ties back to the process development and basic research. The better researchers can characterize the products under development, the more they will know about how the products work and the easier it will be to tie these products to patient outcomes.
Meet some of the Children’s National multidisciplinary experts who join forces to lead the cell therapy space.
Jay Tanna, M.S., quality assurance manager, has extensive experience with drug development at Children’s National as well as Sloan Kettering, another premier cell therapy institution. He has a Masters in Pharmaceutical Manufacturing and a Regulatory Affairs Certification (RAC) in U.S. FDA drugs and biologics regulations from the Regulatory Affairs Professional Society (RAPS).
Kathryn Bushnell, M.T. (ASCP), the cell therapy lab manager, oversees Stem Cell Processing. She has 20 years of experience with hematopoietic progenitor cells and cellular therapy, starting her career as a medical technologist at MD Anderson Cancer Center.
Nan Zhang, Ph.D., assistant director of manufacturing at Children’s National, has worked at Wake Forest and the National Institutes of Health developing various cellular therapies. Zhang chaired the cell processing session at the annual meeting of the American Society of Hematology in 2020.
Abeer Shibli, M.T., is a specialist in the cellular therapy laboratory with extensive experience in the processing of cellular therapy products. She has over 10 years of experience as a medical technologist, is specialized in blood banking and transfusion medicine and is one of the senior technologists in the lab.
Chase McCann, M.S.P.H., Ph.D., is the cell therapy lab lead for manufacturing at Children’s National Hospital. He recently completed his Ph.D. training in Immunology and Microbial Pathogenesis at Weill Cornell Medicine in New York. Much of his graduate research focused on developing and enhancing cellular therapies for HIV while identifying common mechanisms of escape, shared by both HIV and various cancers, which limit the efficacy of current cell therapies. Previously, McCann worked as the laboratory coordinator for the HIV Prevention Trials Network, and now oversees the manufacturing of many cell therapies supporting the many clinical trials currently underway at Children’s National.
Anushree Datar, M.S., the cell therapy lab lead for immune testing and characterization, oversees the release testing of products manufactured in the GMP for safety and function before they can be infused in patients. She also leads a part of the research team investigating the improvement in immune function after cell infusion.
Dr. Bollard is also the director of the Program for Cell Enhancement and Technologies for Immunotherapy and president of the Foundation for the Accreditation for Cellular Therapy (FACT). Additionally, in 2019, she became a member of the Frederick National Laboratory Advisory Committee (FNLAC) for the NIH and an ad hoc member of the Pediatric Oncologic Drugs Advisory Committee (ODAC) for the FDA. She has been an associate editor for the journal Blood since 2014 and in 2020 was appointed editor-in-chief of Blood Advances (starting Fall 2021). Dr. Bollard has 21 years of cell therapy experience as a physician, sponsor and principal investigator.
Dr. Hanley serves as the commissioning editor of the peer-reviewed journal Cytotherapy, as the vice-president-elect (North America) of the International Society of Cell and Gene Therapy (ISCT), and board of directors member at FACT, which provides him visibility into various cell and gene therapies, manufacturing approaches, and other intangibles that make Children’s National facility one of the leaders in the field.
To find the full research program list and their experts, click here.

Lab members celebrate the expansion of the GMP Laboratory.