How EPO saves babies’ brains
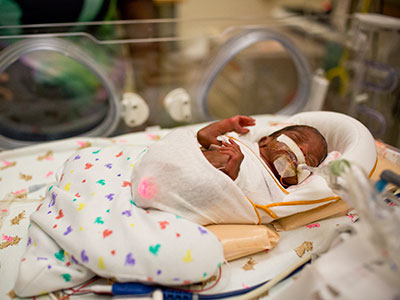
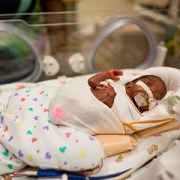
Researchers have discovered that treating premature infants with erythropoietin can help protect and repair their vulnerable brains.
The drug erythropoietin (EPO) has a long history. First used more than three decades ago to treat anemia, it’s now a mainstay for treating several types of this blood-depleting disorder, including anemia caused by chronic kidney disease, myelodysplasia and cancer chemotherapy.
More recently, researchers discovered a new use for this old drug: Treating premature infants to protect and repair their vulnerable brains. However, how EPO accomplishes this feat has remained unknown. New genetic analyses presented at the Pediatric Academic Societies 2018 annual meeting that was conducted by a multi-institutional team that includes researchers from Children’s National show that this drug may work its neuroprotective magic by modifying genes essential for regulating growth and development of nervous tissue as well as genes that respond to inflammation and hypoxia.
“During the last trimester of pregnancy, the fetal brain undergoes tremendous growth. When infants are born weeks before their due dates, these newborns’ developing brains are vulnerable to many potential insults as they are supported in the neonatal intensive care unit during this critical time,” says An Massaro, M.D., an attending neonatologist at Children’s National Health System and lead author of the research. “EPO, a cytokine that protects and repairs neurons, is a very promising therapeutic approach to support the developing brains of extremely low gestational age neonates.”
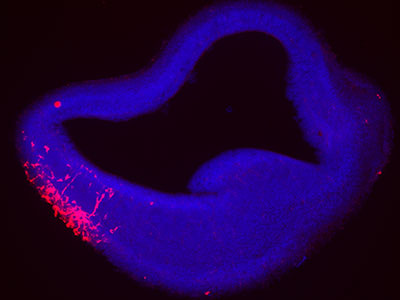
The research team investigated whether micro-preemies treated with EPO had distinct DNA methylation profiles and related changes in expression of genes that regulate how the body responds to such environmental stressors as inflammation, hypoxia and oxidative stress. They also investigated changes in genes involved in glial differentiation and myelination, production of an insulating layer essential for a properly functioning nervous system. The genetic analyses are an offshoot of a large, randomized clinical trial of EPO to treat preterm infants born between 24 and 27 gestational weeks.
The DNA of 18 newborns enrolled in the clinical trial was isolated from specimens drawn within 24 hours of birth and at day 14 of life. Eleven newborns were treated with EPO; a seven-infant control group received placebo.
DNA methylation and whole transcriptome analyses identified 240 candidate differentially methylated regions and more than 50 associated genes that were expressed differentially in infants treated with EPO compared with the control group. Gene ontology testing further narrowed the list to five candidate genes that are essential for normal neurodevelopment and for repairing brain injury:
- Neurogenin 1, a transcription factor that governs the progression of neurogenesis
- FOS like 1, implicated in development of cognitive deficits after oxygen depravation (hypoxia)
- Mitogen-activated protein kinase 8 interacting protein 2, encodes a scaffolding protein broadly expressed in the brain. Experimental models that lack this protein display autistic tendencies.
- Resistance to inhibitors of cholinesterase 8 homolog A, an essential player in generating new brain cells and
- Major histocompatibility complex, class II, DR alpha, a central player in proper immune system function.
“These findings suggest that EPO’s neuroprotective effect may be mediated by epigenetic regulation of genes involved in the development of the nervous system and that play pivotal roles in how the body responds to inflammation and hypoxia,” Dr. Massaro says.
In addition to Dr. Massaro, study co-authors include Theo K. Bammler, James W. MacDonald, biostatistician, Bryan Comstock, senior research scientist, and Sandra “Sunny” Juul, M.D., Ph.D., study principal investigator, all of University of Washington.