Tag Archive for: Clinical Trials
AI team wins international competition to measure pediatric brain tumors

Children’s National Hospital scientists won first place in a global competition to use artificial intelligence (AI) to analyze pediatric brain tumor volumes, demonstrating the team’s ground-breaking advances in imaging and machine learning.
During the International Conference on Medical Image Computing and Computer Assisted Intervention (MICCAI), the Children’s National team demonstrated the most accurate algorithm to study the volume of brain tumors – the most common solid tumors affecting children and adolescents and a leading cause of disease-related death at this young age. The technology could someday help oncologists understand the extent of a patient’s disease, quantify the efficacy of treatments and predict patient outcomes.
“The Brain Tumor Segmentation Challenge inspires leaders in medical imaging and deep learning to try to solve some of the most vexing problems facing radiologists, oncologists, computer engineers and data scientists,” said Marius George Linguraru, D.Phil., M.A., M.Sc., the Connor Family Professor in Research and Innovation and principal investigator in the Sheikh Zayed Institute for Pediatric Surgical Innovation. “I am honored that our team won, and I’m even more thrilled for our clinicians and their patients, who need us to keep moving forward to find new ways to treat pediatric brain tumors.”
Why we’re excited
With roughly 4,000 children diagnosed yearly, pediatric brain tumors are consistently the most common type of pediatric solid tumor, second only to leukemia in pediatric malignancies. At the urging of Linguraru and one of his peers at the Children’s Hospital of Philadelphia, pediatric data was included in the international competition for the first time, helping to ensure that children are represented in medical and technological advances.
The contest required participants to use data from multiple institutions and consortia to test competing methods fairly. The Children’s National team created a method to tap into the power of two types of imaging and machine learning: 3D convolutional neural network and 3D Vision Transformer-based deep learning models. They identified regions of the brain affected by tumors, made shrewd data-processing decisions driven by the team’s experience in AI for pediatric healthcare and achieved state-of-the-art results.
The competition drew 18 teams who are leaders from across the AI and machine learning community. The runner-up teams were from NVIDIA and the University of Electronic Science and Technology of China.
The big picture
“Children’s National has an all-star lineup, and I am thrilled to see our scientists recognized on an international stage,” said interim Executive Vice President and Chief Academic Officer Catherine Bollard, M.D., M.B.Ch.B., director of the Center for Cancer for Immunology Research. “As we work to attack brain tumors from multiple angles, we continue to show our exceptional ability to create new and better tools for diagnosing, imaging and treating these devastating tumors.”
A destination for pediatric oncology care: Children’s National Hospital’s T-cell therapy trials
When children are diagnosed with pediatric cancer, most doctors are forced to reach for the same standard therapies that were available decades ago. Research oncologists at Children’s National Hospital are changing that with clinical trials that will hopefully train the body’s immune system – specifically its T cells – to fight the tumors.
Holly Meany, M.D., and her colleague Amy Hont, M.D., oncologists and research scientists at the Center for Cancer and Immunology Research, have put together a pair of clinical trials that are investigating two pathways for using T cells to go after solid tumors.
“At Children’s National, we have a novel immunotherapy to offer to patients with relapsed or refractory solid tumors,” said Meany, director of the Solid Tumor Program. “This is a patient population who has failed standard therapy, so new technologies and treatments are always needed in this group.”
Where we started
Meany’s trial laid the foundation. She began the center’s research using a patient’s own blood sample to develop a targeted therapy and evaluate the safety and efficacy of this approach. In her study, scientists isolated the T cells, grew millions in a lab and reinfused them into the patient. The cells were replicated in an environment that was rich in three proteins that are commonly found on the surface of solid tumor cancer cells.
“Our hope and hypothesis are that when we give the T cells back to the patient, those T cells circulate and hunt down the cancer cells that have the tumor proteins,” Meany said. “We are hoping to use the patient’s own immune system to attack the cancer in an enduring way.”
Where we are headed
Hont’s phase 1 trial, which is currently recruiting participants, builds on Meany’s work using a healthy donor whose T cells have not been impacted by chemotherapy or other treatments. The cells can be prepared, stored and readily available for patients who need them. They are also matched through specific proteins on the patient’s own cells to bolster their effectiveness. The participants in this trial have Wilms tumors, rhabdomyosarcoma, neurosarcoma, soft tissue sarcoma or neuroblastoma, but conventional therapies including chemotherapy, radiation or surgery were unable to fully treat the disease.
In both studies, Hont said that the T cells have been given in an outpatient setting with fewer side effects compared to other cancer treatments aimed at high-risk malignancies.
“This allows patients to really maintain a good quality of life during a particularly hard time,” Hont said. “Also, these T cells are designed to act in the body the way that our immune system acts in a physiologic way. This means patients typically don’t have the severe side effects that we think of with chemotherapy or other therapies.”
Children’s National leads the way
The team at Children’s National is one of the few in the country to offer this kind of T-cell therapy for solid tumors. “Immunotherapy has been challenging for this patient population because the tumors are adept at finding out ways to evade treatment,” Hont said. “Giving patients a chance to receive a targeted T-cell therapy, while also maintaining a high quality of life, is something that’s special here.”
AI: The “single greatest tool” for improving access to pediatric healthcare

The daylong event drew experts from the Food and Drug Administration, Pfizer, Oracle Health, NVIDIA, AWS Health and elsewhere to start building a community aimed at using data for the advancement of pediatric medicine.
The future of pediatric medicine holds the promise of artificial intelligence (AI) that can help diagnose rare diseases, provide roadmaps for safer surgeries, tap into predictive technologies to guide individual treatment plans and shrink the distance between patients in rural areas and specialty care providers.
These and dozens of other innovations were contemplated as scientists came together at the inaugural symposium on AI in Pediatric Health and Rare Diseases, hosted by Children’s National Hospital and the Fralin Biomedical Research Institute at Virginia Tech. The daylong event drew experts from the Food and Drug Administration, Pfizer, Oracle Health, NVIDIA, AWS Health and elsewhere to start building a community aimed at using data for the advancement of pediatric medicine.
“AI is the single greatest tool for improving equity and access to health care,” said symposium host Marius George Linguraru, D.Phil., M.A., M.Sc., principal investigator at the Sheikh Zayed Institute for Pediatric Surgical Innovation. “As a population, kids are vastly underrepresented in scientific research and resulting treatments, but pediatric specialties can use AI to provide medical care to kids more efficiently, more quickly and more effectively.”
What they’re saying
Scientists shared their progress in building digital twins to predict surgical outcomes, enhancing visualization to increase the precision of delicate interventions, establishing data command centers to anticipate risks for fragile patients and more. Over two dozen speakers shared their vision for the future of medicine, augmented by the power of AI:
- Keynote speaker Subha Madhavan, Ph.D., vice president and head of AI and machine learning at Pfizer, discussed various use cases and the potential to bring drugs to market faster using real-world evidence and AI. She saw promise for pediatrics. “This is probably the most engaging mission: children’s health and rare diseases,” she said. “It’s hard to find another mission that’s as compelling.”
- Brandon J. Nelson, Ph.D., staff fellow in the Division of Imaging, Diagnostics and Software Reliability at the Food and Drug Administration, shared ways AI will improve diagnostic imaging and reduce radiation exposure to patients, using more advanced image reconstruction and denoising techniques. “That is really our key take-home message,” he said. “We can get what … appear as higher dose images, but with less dose.”
- Daniel Donoho, M.D., a neurosurgeon at Children’s National, introduced the audience to the potential of “Smart ORs”: operating rooms where systems can ingest surgery video and provide feedback and skill assessments. “We have to transform the art of surgery into a measurable and improvable scientific practice,” he said.
- Debra Regier, M.D., chief of Genetics and Metabolism at Children’s National, discussed how AI could be used to diagnose and treat rare diseases by conducting deep dives into genetics and studying dysmorphisms in patients’ faces. Already, Children’s National has designed an app – mGene – that measures facial features and provides a risk score to help anyone in general practice determine if a child has a genetic condition. “The untrained eye can stay the untrained eye, and the family can continue to have faith in their provider,” she said.
What’s next
Linguraru and others stressed the need to design AI for kids, rather than borrow it from adults, to ensure medicine meets their unique needs. He noted that scientists will need to solve challenges, such as the lack of data inherent in rare pediatric disorders and the simple fact that children grow. “Children are not mini-adults,” Linguraru said. “There are big changes in a child’s life.”
The landscape will require thoughtfulness. Naren Ramakrishnan, Ph.D., director of the Sanghani Center for Artificial Intelligence & Analytics at Virginia Tech and symposium co-host, said that scientists are heading into an era with a new incarnation of public-private partnerships, but many questions remain about how data will be shared and organizations will connect. “It is not going to be business as usual, but what is this new business?” he asked.
Kids’ headaches can be disruptive. We need solutions.
 Experts leading the Headache Program at Children’s National Hospital recognize how common these disorders are. They also know how disruptive they can be in the day-to-day of children.
Experts leading the Headache Program at Children’s National Hospital recognize how common these disorders are. They also know how disruptive they can be in the day-to-day of children.
Marc DiSabella, D.O., is the director of the program. He is currently leading five pediatric headache trials. In this Q&A, he tells us about the ongoing trials, offering insight into innovative solutions and how he’s carving a new path to improve the quality of life of his patients.
Q: How has your team advised other neurologists on innovative care for patients with headaches that have been refractory to medicines?
A: We receive referrals from outside institutions when they need additional input for diagnostic and management options. We receive patient consult requests from around the country – and sometimes out of the country – to help improve symptoms. In most instances, these headaches tend to be difficult to control and do not respond to available medications. We really try to take a holistic approach to their care, and use treatments in parallel. For example, diagnostic, lifestyle techniques, medications, pain focused cognitive behavioral therapy and physical therapy. We also use complementary medicine as needed, such as acupuncture, injections and infusions.
Q: It is unusual for neurology divisions to run multiple pediatric trials focused on headaches. You are currently leading five that are open. How does this work move the field forward?
A: The medications we offer through our trials allow us to offer treatments that would otherwise not be available to pediatric patients. We do this in hopes of providing them relief while advancing the field. We are hopeful that these new therapies are as effective in pediatrics as they have shown to be in adults. But it is necessary to complete randomized clinical trials to prove this is the case. Historically, pediatric patients in clinical trials investigating painful conditions like migraines have had a disproportionately high placebo response rate. This means even the patients receiving a benign placebo have a high chance of symptom improvement. The newer medications show much better tolerability to the drugs used historically.
Q: What excites you about this work?
A: Pediatric pain disorders are unbelievably gratifying to treat because we take a mysterious disorder that waxes and wanes with no clear reason and give patients back control of their lives. It is extremely frustrating for a patient and their family to know that their day-to-day life can be abruptly derailed by a pain crisis. We work to provide them with several tools they can use daily to take back their lives.
Q: How is this work unique?
A: Our program was created organically over the years through our experiences with our patients. First, we noticed the disruption to patients’ personal and school performance from having untreated pain and recognized the need for pain psychology. Then, we expanded to have physical therapy to recondition patients and perform desensitization. Finally, we recognized our patients need additional medication options not offered through the standard of care. So, we expanded to open our various clinical trials, including those with pharma and internal protocols. As a result, we incorporated the use of Botox injections, for example, and soon will use a novel remote electro-neuromodulatory device.
A melanoma drug shows promise for NF1 plexiforms
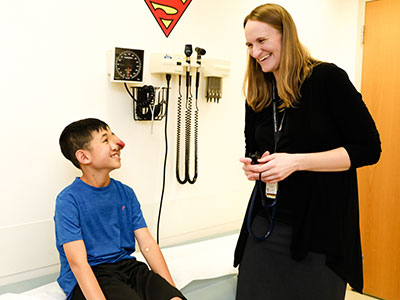
Dr. Bornhorst talks with her patient Maddox Gibson, who is part of the compassionate use trial of selumentinib for which she serves as site principal investigator.
A class of drugs originally approved for stopping tumor growth in adult cancers including melanoma and small cell lung cancer may be the key to treating plexiform neurofibromas in neurofibromatosis type 1 (NF1), too. If effective, doctors will finally have a treatment to offer for children with complicated plexiform neurofibromas that can’t be removed via surgery.
These drugs, including selumentinib, work by inhibiting the activity of the mitogen-activated protein kinase enzymes MEK1 and MEK2. The enzymes have a direct impact on the activity of the cellular signaling pathway MAPK/ERK, which can be overactive some cancers.
Ongoing pre-clinical studies made possible by national and international neurofibromatosis research collaborations demonstrated that this same pathway is overactive in children with NF1 who have plexiform neurofibromas. The compelling findings from these studies set the stage for clinical trials to test the safety and efficacy of selumetinib and other MEK inhibitors as a therapy for pediatric NF1 patients with inoperable plexiform neurofibromas.
At Children’s National, these studies are run by clinicians such as Miriam Bornhorst, M.D., clinical director of the Gilbert Family Neurofibromatosis Institute and AeRang Kim, M.D., Ph.D. Children’s is one of only four sites in the United States to participate in a National Institutes of Health-led clinical trial to study the use of selumetinib in NF1. Dr. Kim is the site principal investigator and Dr. Bornhorst serves as co-principal investigator on phase 2 of the trial.
“Any time we find a medication that works with NF1, we’re excited, especially because for so many years, we didn’t have any of these options for these families,” Dr. Bornhorst says. “We’re offering something these families have never had before – a treatment that may stop growth and maybe even keep these tumors from returning. It means we’re doing more than managing symptoms – we’re really treating them.”
NF1 affects a relatively small number of people, particularly children. However, researchers and clinicians who are dedicated to the condition have banded together via collaborations and consortia to fuel research and development of new therapies across multiple institutions in the U.S. and abroad.
“Patients come to see me who’ve been at our clinic for years and I’ll talk about MEK inhibitors, and they are just shocked to hear there may be a new option,” Dr. Bornhorst says.
The NIH trial continues to collect data at four U.S. centers, with the ultimate goal of submitting the results for FDA review. Additional data is also collected from patients who didn’t qualify for the trial but who received the drug for compassionate use, an effort led by Dr. Bornhorst. The information collected from that compassionate use trial also helps investigators make the case to broaden the eligibility criteria for future trials.
“The medications are showing that they work,” Dr. Bornhorst notes. “Now we need to determine how to identify the patients who we know will need these therapies.”
To meet that need, other studies, led by both Dr. Bornhorst and Dr. Kim, seek radiographic and blood biomarkers that will identify children with NF1 who are more likely to develop plexiform neurofibromas, and whose plexiforms may progress to something malignant.
Roger Packer, M.D., elected Pediatric Co-Chair by the National Cancer Institute’s Brain Malignancies Steering Committee

Roger J. Packer, M.D., Senior Vice President, Center for Neuroscience & Behavioral Health at Children’s National Health System, has been elected by the National Cancer Institute’s Brain Malignancies Steering Committee (BMSC) as the committee’s new Pediatric Co-Chair.
One of 16 steering committees formed in response to the recommendations of the Clinical Trials Working Group mandated by the National Cancer Advisory Board (NCAB), the BMSC’s goal is to promote the best clinical and translational research for patients with brain cancer by critically reviewing Phase 2 and Phase 3 clinical trial concepts.
Dr. Packer also directs the Brain Tumor Institute and is principal investigator for the Pediatric Brain Tumor Consortium (PBTC), formed under the auspices of the National Cancer Institute (NCI). He has worked closely with the NCI and the National Institute of Neurological Disorders and Stroke (NINDS), and has served on multiple committees setting the directions for neurologic clinical and basic science research for the future. Much of Dr. Packer’s clinical research has been translational in nature. He has been part of studies evaluating the molecular genetics of childhood and adult neurologic diseases, and has also coordinated the first gene therapy study for children with malignant brain tumors in the U.S.
Enhancing pediatric nephrology clinical trial development

Fewer than 50 percent of pharmaceuticals approved by federal authorities are explicitly approved for use in kids, and even fewer devices are labeled for pediatric use.
When children develop kidney disease, it can play out in dramatically different ways. They can experience relatively mild disorders that respond to existing treatments and only impact their lives for the short term. Children also can develop chronic kidney disease that defies current treatments and can imperil or end their lives.
Fewer than 50 percent of pharmaceuticals approved by federal authorities are explicitly approved for use in kids, and even fewer devices are labeled for pediatric use. Congress has offered incentives to manufacturers who study their treatments in children, but the laws do not require drug makers to demonstrate statistical significance or for the clinical trial to improve or extend children’s lives.
To overcome such daunting obstacles, the American Society of Pediatric Nephrology established a Therapeutics Development Committee to forge more effective public-private partnerships and to outline strategies to design and carry out pediatric nephrology clinical trials more expeditiously and effectively.
“We have seen how other pediatric subspecialties, such as cancer and arthritis, have leveraged similar consortia to address mutual concerns and to facilitate development of new therapeutics specific to those diseases,” says Marva Moxey-Mims, M.D., chief of the Division of Nephrology at Children’s National Health System and a founding committee member. “As a group, we aim to collectively identify and remedy the most pressing needs in pediatric nephrology. As just one example, the committee could help to increase the number of sites that host research studies, could expand the pool of potential study volunteers and could lower the chances of duplicating efforts.”
A paper summarizing their efforts thus far, “Enhancing clinical trial development for pediatric kidney diseases,” written by Dr. Moxey-Mims and 15 co-authors, was published online Aug. 30 by Pediatric Research. The journal’s editors will feature the review article in the “Editor’s Focus” of an upcoming print edition of the publication.
The committee is comprised of academic pediatric nephrologists, patient advocates, private pharmaceutical company representatives and public employees at the Food and Drug Administration and the National Institutes of Health. But it is likely to grow in size and in stakeholder diversity.
Already, committee members have learned that they achieve better results by working together. Early communication can avoid flaws in designing clinical trials, such as overestimating the volume of clinical samples that can feasibly be collected from a small child, or that could misinterpret the type of data needed to secure federal approval.
While public and private investigators took similar approaches to clinical trial design, academic investigators were more conceptual as they summarized their study design Road Map. Industry representatives, by contrast, included more granular detail about study organization and milestones along the path toward regulatory approval.
According to the study authors, both groups understand the critical role that patients and families can play in early research study design, such as accelerating patient recruitment, bolstering the credibility of research and helping to translate research results into actual clinical practice.
“We are pleased to have created a forum that allows participants to share valuable viewpoints and concerns and to understand how regulations and laws could be changed to facilitate development of effective medicines for children with kidney disease,” says Dr. Moxey-Mims. “We hope the relationships and trust forged through these conversations help to speed the development and approval of the next generation of therapies for pediatric renal disease.”
Children’s National Heart Institute experts partner with FDA and nation’s leading cardiology organizations to advance pediatric drug development
New joint health policy statement offers roadmap for immediate changes in clinical trial design to save children’s lives
Families with children suffering from rare and difficult-to-treat cardiovascular diseases may soon have better access to drugs to treat their often life-threatening conditions. For the first time, experts from the U.S. Food and Drug Administration (FDA), the American College of Cardiology, the American Heart Association and the American Academy of Pediatrics are working together to describe the challenges and opportunities to improve pediatric drug research as shared in a joint statement published online June 29 in the Journal of the American College of Cardiology and Circulation: Cardiovascular Quality and Outcomes.
“Children should have access to the latest advances in treatment and the best care. By challenging the status quo and designing new, safe and effective alternative study designs, we can give them the best opportunity to grow up stronger,” notes David Wessel, M.D., executive vice president and chief medical officer, Hospital and Specialty Services at Children’s National Health System. Dr. Wessel is internationally recognized for his pioneering work in caring for children with heart disease. As the senior author of the new joint statement and principal investigator of the STARTS-1 trial, which is the catalyst for this collaboration, he says he is “optimistic about this forward progress.”
According to the statement, less than 50 percent of drugs approved for use in the United States have sufficient data to support labeling for dosing, safety and efficacy in children. Additionally, a 2008 report by Pasquali et al, which reviewed more than 30,000 records of hospitalized children with cardiovascular disease, found that 78 percent received at least one off-label medication and 31 percent received more than three.
There are numerous challenges in the development and approval of medications for children – especially those with rare diseases – but the paper’s lead author, Craig Sable, M.D., associate division chief of cardiology at Children’s National, says we can and need to do better.
“While randomized clinical drug trials remain the gold standard in advancing care for adults with cardiovascular disease, relying solely on these types of trials for children unnecessarily limits the drugs approved for use in children,” says Dr. Sable. “Through this unique collaboration that unifies the voice of leaders in pediatric cardiology and the FDA, our goal is to provide a framework to better define which drugs are needed and how we can create novel study designs to overcome the current trial barriers.”
To read more about the barriers and ideas presented, please find the full statement here.