Wellness wins! Strengthening school and health partnerships across the nation

A day of learning and collaboration at the MUSC Boeing Center for Children’s Wellness
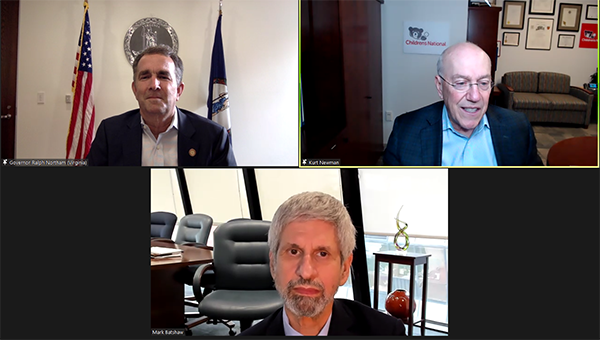
Cross-institution collaboration is accelerating efforts to create healthier school environments nationwide. In February 2026, Cara Biddle, MD, MPH, Danielle Dooley, MD, MPhil, Torine Creppy and other Children’s National Hospital community and school health leaders visited The Boeing Center for Children’s Wellness (BCCW) at the Medical University of South Carolina (MUSC) in Charleston, South Carolina. During the visit, they learned about the BCCW’s evidence-based approach to creating sustainable, health-promoting schools. The initiative weaves wellness into curriculum, policies, food services, physical and social environments, and community partnerships. Children’s National presented on the School-Friendly Health Systems framework and efforts to reduce school absenteeism, operate school-based health centers and collaborate through IMPACT DC to improve asthma control and keep kids in school.
How does this work move the field forward?
Since over 90% of children spend most of their day in school settings, it’s vital for pediatric hospitals to partner with schools. The MUSC BCCW School-based Wellness Initiative helps schools create healthy physical, social and emotional environments that support learning. Research shows that health-promoting school environments are linked to better grades, improved attendance and lower risk of chronic disease.
“In our Washington, D.C., Goldberg primary care centers, we care for nearly 50% of all children in DC. These are the same children that our colleagues in DC schools are teaching and connecting with every day. It is critical that we keep schools at the forefront of our partnerships and this site visit sparked collaboration and shared learning that will enable us to strengthen our school partnerships,” said Cara Biddle, MD, MPH, interim senior vice president, Community Health and division chief of General Pediatrics at Children’s National.
“At Children’s National, we’re committed to helping families thrive in their communities. Partnering with schools is an essential part of this work. Being able to do a hands-on site visit with another health system is invaluable for the exchange of ideas and for scaling up innovations in school partnerships,” said Torine Creppy, president of Safe Kids Worldwide and vice president of Community Engagement and Impact at Children’s National.
What did you find that excites you?
For more than 15 years, the MUSC BCCW School-based Wellness Initiative has demonstrated improvements in school absenteeism, high school graduation rates, and student BMI percentiles in participating schools. The site visit included tours of two high performing schools in Charleston, C.E. Williams North Middle School and Stono Park Elementary Schools, who recently received the MUSC BCCW grand prize wellness awards for creating healthier learning environments. Participating schools were evaluated using a wellness checklist and those who met criteria received a monetary award reinvested to sustain and expand their efforts.
The site visit was funded by The Boeing Company, which has supported community-oriented work at both Children’s National and MUSC. This support will elevate, expand and leverage the Children’s National School-Friendly Health Systems Learning Collaborative to disseminate the MUSC BCCW School-based Wellness Initiative to children’s hospitals nationwide through the Children’s National-led collaborative. The MUSC BCCW model provides direct support for more than 20 school districts and 316 schools in South Carolina and Pennsylvania and implements universal wellness strategies targeting improved nutrition, increased physical activity and enhanced social-emotional wellness for students and staff.
“This grant supports the next generation of leaders and innovators. This initiative is about helping kids be happier and healthier in school and life,” said Jessica Williford, senior director of State Advocacy and Global Engagement at Boeing South Carolina.
Children’s National led the development of the School-Friendly Health Systems guiding principles and a roadmap for scaling the framework in partnership with more than 15 other children’s hospitals and partners. Becoming school-friendly means that hospitals and health systems have made a commitment to actively help children achieve optimal health and reach their full academic potential.
Children’s National will host virtual SFHS webinars beginning March 2026 and an in-person School Health Wellness Symposium on June 9, sponsored by The Boeing Company. For more information on the SFHS Learning Collaborative, contact School Partnerships@childrensnational.org.