Autonomic nervous system appears to function well regardless of mode of childbirth

Late in pregnancy, the human body carefully prepares fetuses for the rigors of life outside the protection of the womb. Levels of cortisol, a stress hormone, ramp up and spike during labor. Catecholamines, another stress hormone, also rise at birth, helping to kick start the necessary functions that the baby will need to regulate breathing, heartbeat, blood pressure and energy metabolism levels at delivery. Oxytocin surges, promoting contractions for the mother during labor and stimulating milk production after the infant is born.
These processes also can play a role in preparing the fetal brain during the transition to life outside the womb by readying the autonomic nervous system and adapting its cerebral connections. The autonomic nervous system acts like the body’s autopilot, taking in information it needs to ensure that internal organs run steadily without willful action, such as ensuring the heart beats and eyelids blink at steady intervals. Its yin, the sympathetic division, stimulates body processes while its yang, the parasympathetic division, inhibits them.
Infants born preterm have reduced autonomic function compared with their full-term peers and also face possible serious neurodevelopmental impairment later in life. But is there a difference in autonomic nervous system function for full-term babies after undergoing labor compared with infants delivered via cesarean section (C-section)?
A team from the Children’s National Inova Collaborative Research Program (CNICA) – a research collaboration between Children’s National in Washington, D.C., and Inova Women’s and Children’s Hospital in Virginia – set out to answer that question in a paper published online July 30, 2019, in Scientific Reports.
They enrolled newborns who had experienced normal, full-term pregnancies and recorded their brain function and heart performance when they were about 2 days old. Infants whose conditions were fragile enough to require observation in the neonatal intensive care unit were excluded from the study. Of 167 infants recruited for the prospective cohort study, 118 newborns had sufficiently robust data to include them in the research. Of these newborns:
- 62 (52.5%) were born by vaginal delivery
- 22 (18.6%) started out with vaginal delivery but ultimately switched to C-section based on failure to progress, failed labor induction or fetal intolerance to labor
- And 34 (28.8%) were born by elective C-section.
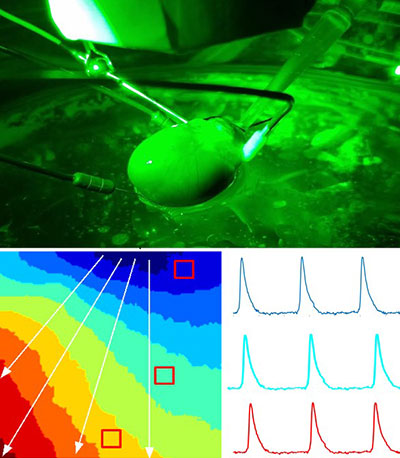
The CNICA research team swaddled infants for comfort and slipped electrode nets over their tiny heads to simultaneously measure heart rate variability and electrocortical function through non-invasive techniques. The team hypothesized that infants who had been exposed to labor would have enhanced autonomic tone and higher cortical electroencephalogram (EEG) power than babies born via C-section.
“In a low-risk group of babies born full-term, the autonomic nervous system and cortical systems appear to function well regardless of whether infants were exposed to labor prior to birth,” says Sarah B. Mulkey, M.D., Ph.D., a fetal–neonatal neurologist in the Division of Fetal and Transitional Medicine at Children’s National and the study’s lead author.
However, infants born by C-section following a period of labor had significantly increased accelerations in their heart rates. And the infants born by C-section during labor had significantly lower relative gamma frequency EEG at 25.2 hours old compared with the other two groups studied.
“Together these findings point to a possible increased stress response and arousal difference in infants who started with vaginal delivery and finished delivery with C-section,” Dr. Mulkey says. “There is so little published research about the neurologic impacts of the mode of delivery, so our work helps to provide a normal reference point for future studies looking at high-risk infants, including babies born preterm.”
Because the research team saw little differences in autonomic tone or other EEG frequencies when the infants were 1 day old, future research will explore these measures at different points in the newborns’ early life as well as the role of the sleep-wake cycle on heart rate variability.
In addition to Dr. Mulkey, study co-authors include Srinivas Kota, Ph.D., Rathinaswamy B. Govindan, Ph.D., Tareq Al-Shargabi, MSc, Christopher B. Swisher, BS, Laura Hitchings, BScM, Stephanie Russo, BS, Nicole Herrera, MPH, Robert McCarter, ScD, and Senior Author Adré J. du Plessis, M.B.Ch.B., MPH, all of Children’s National; and Augustine Eze Jr., MS, G. Larry Maxwell, M.D., and Robin Baker, M.D., all of Inova Women’s and Children’s Hospital.
Financial support for research described in this post was provided by the National Institutes of Health National Center for Advancing Translational Sciences under award numbers UL1TR001876 and KL2TR001877.