School entry neurodevelopmental outcomes of Zika-exposed Colombian children

The Children’s National Hospital Zika Research Team and collaborators from Biomelab, in Barranquilla, Colombia take a picture after a study visit in Sabanalarga, Colombia following the neurodevelopmental outcomes of children who had in utero exposure to Zika virus. Pictured from Children’s National Hospital: Dr. Sarah Mulkey, Regan Andringa-Seed, Margarita Arroyave-Wessel, and Dr. Madison Berl.
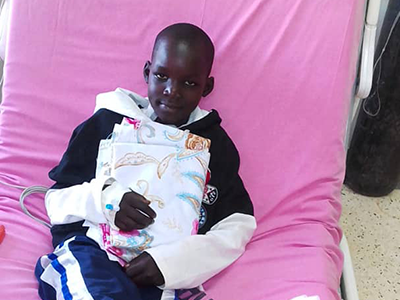
The long-term neurodevelopmental effects of antenatal Zika virus (ZIKV) exposure in children without congenital Zika syndrome (CZS) remain unclear, as few children have been followed to the age of starting primary school.
In a new study published in Pathogens, researchers found children with in utero ZIKV exposure appear to have an overall positive developmental trajectory at 4 to 5 years of age but may experience risks to neurodevelopment in areas of emotional regulation and adaptive mobility.
The hold up in the field
Children who were born during the ZIKV epidemic and who had in utero exposure to ZIKV are only now at the age to start school. Child neurodevelopmental outcome data has not been reported at the age of school entry for children with antenatal ZIKV exposure who do not have the severe birth defects of CZS.
“As these children approach the early school-age years, we aim to examine whether there are neurodevelopmental differences in executive function, motor ability, language development or scholastic skills as compared to a group of unexposed control participants from the same communities in Colombia,” says Sarah Mulkey, M.D., Ph.D., prenatal-neonatal neurologist in The Zickler Family Prenatal Pediatrics Institute at Children’s National Hospital and lead author of the study.
Moving the field forward
Building on previous findings, this study presents the longitudinal outcomes of a well-characterized Colombian cohort of ZIKV-exposed children without CZS at ages 4 to 5 years. These children have been seen for neurodevelopmental follow-up as infants and toddlers at approximately 6 months, 18 months and 3 years of age as part of an international collaboration between researchers in Barranquilla, Colombia and at Children’s National beginning in 2016. The objective of this study was to assess the multi-domain neurodevelopmental outcomes in 4 to 5-year-old children with antenatal ZIKV exposure without CZS compared to unexposed controls in Colombia.
Why we’re excited
Many of the children who had antenatal ZIKV exposure are making good progress in multiple areas of their neurodevelopment. However, the researchers found that children with antenatal ZIKV exposure have differences in areas of emotional regulation, executive function, mood and behavior which may relate to virus exposure during their early brain development.
“These areas of brain function are important for future academic achievement, employment, mental health and social relationships,” says Dr. Mulkey. “So, it will be important to continue to follow these children at older ages when they start school.”
Children’s National leads the way
Children’s National is a leader in conducting outcome studies of children born following antenatal ZIKV exposure. This study follows children in Colombia who are now 5 years old who were first studied while they were in the womb. These children have contributed unique longitudinal understanding to early child neurodevelopment following in utero exposure to ZIKV.
Dr. Mulkey is committed to studying the long-term neurodevelopmental impacts that viruses like Zika and SARS-CoV-2 have on infants born to mothers who were infected during pregnancy through research with the Congenital Infection Program at Children’s National and in collaboration with colleagues in Colombia.
Additional Children’s National authors include Meagan Williams M.S.P.H., C.C.R.C., senior research coordinator; Regan Andringa-Seed, clinical research coordinator, Margarita Arroyave-Wessel, clinical research coordinator; L. Gilbert Vezina, M.D., director, Neuroradiology Program; Dorothy Bulas, M.D., chief, Diagnostic Imaging and Radiology; Robert Podolsky, biostatistician.

Dr. Sarah Mulkey and Children’s National clinical research coordinators in the Prenatal Pediatrics Institute and the Division of Pediatric Infectious Diseases display their paintings of the Zika virus. Pictured from left to right: Manuela Iglesias, Elizabeth Corn, Dr. Sarah Mulkey, Emily Ansusinha and Meagan Williams.







 Advanced MRI visualization techniques to follow blood flow in the hearts of cardiac patients. Gene therapy for pediatric patients with Duchenne muscular dystrophy. 3D-printed casts for treating clubfoot. These were among the most popular articles we published on Innovation District in 2023. Read on for our full list.
Advanced MRI visualization techniques to follow blood flow in the hearts of cardiac patients. Gene therapy for pediatric patients with Duchenne muscular dystrophy. 3D-printed casts for treating clubfoot. These were among the most popular articles we published on Innovation District in 2023. Read on for our full list.
 The hospital will advocate for the unique needs of children as part of nationwide network working to accelerate transformative health solutions.
The hospital will advocate for the unique needs of children as part of nationwide network working to accelerate transformative health solutions.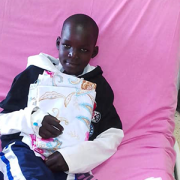




 Children’s National Hospital in Washington, D.C., was ranked #5 in the nation on the U.S. News & World Report 2023-24 Best Children’s Hospitals annual rankings. This marks the seventh straight year Children’s National has made the Honor Roll list. The Honor Roll is a distinction awarded to only 10 children’s hospitals nationwide.
Children’s National Hospital in Washington, D.C., was ranked #5 in the nation on the U.S. News & World Report 2023-24 Best Children’s Hospitals annual rankings. This marks the seventh straight year Children’s National has made the Honor Roll list. The Honor Roll is a distinction awarded to only 10 children’s hospitals nationwide.







 A clinical trial testing a new drug to increase growth in children with short stature. The first ever high-intensity focused ultrasound procedure on a pediatric patient with neurofibromatosis. A low dose gene therapy vector that restores the ability of injured muscle fibers to repair. These were among the most popular articles we published on Innovation District in 2022. Read on for our full top 10 list.
A clinical trial testing a new drug to increase growth in children with short stature. The first ever high-intensity focused ultrasound procedure on a pediatric patient with neurofibromatosis. A low dose gene therapy vector that restores the ability of injured muscle fibers to repair. These were among the most popular articles we published on Innovation District in 2022. Read on for our full top 10 list.