The best of 2022 from Innovation District
 A clinical trial testing a new drug to increase growth in children with short stature. The first ever high-intensity focused ultrasound procedure on a pediatric patient with neurofibromatosis. A low dose gene therapy vector that restores the ability of injured muscle fibers to repair. These were among the most popular articles we published on Innovation District in 2022. Read on for our full top 10 list.
A clinical trial testing a new drug to increase growth in children with short stature. The first ever high-intensity focused ultrasound procedure on a pediatric patient with neurofibromatosis. A low dose gene therapy vector that restores the ability of injured muscle fibers to repair. These were among the most popular articles we published on Innovation District in 2022. Read on for our full top 10 list.
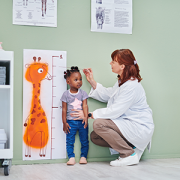
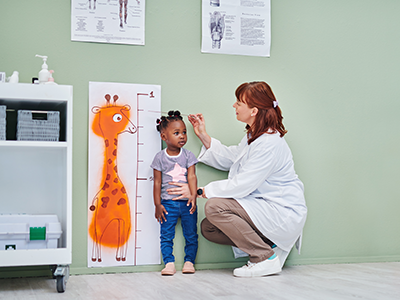
1. Vosoritide shows promise for children with certain genetic growth disorders
Preliminary results from a phase II clinical trial at Children’s National Hospital showed that a new drug, vosoritide, can increase growth in children with certain growth disorders. This was the first clinical trial in the world testing vosoritide in children with certain genetic causes of short stature.
(2 min. read)
2. Children’s National uses HIFU to perform first ever non-invasive brain tumor procedure
Children’s National Hospital successfully performed the first ever high-intensity focused ultrasound (HIFU) non-invasive procedure on a pediatric patient with neurofibromatosis. This was the youngest patient to undergo HIFU treatment in the world.
(3 min. read)
3. Gene therapy offers potential long-term treatment for limb-girdle muscular dystrophy 2B
Using a single injection of a low dose gene therapy vector, researchers at Children’s National restored the ability of injured muscle fibers to repair in a way that reduced muscle degeneration and enhanced the functioning of the diseased muscle.
(3 min. read)
4. Catherine Bollard, M.D., M.B.Ch.B., selected to lead global Cancer Grand Challenges team
A world-class team of researchers co-led by Catherine Bollard, M.D., M.B.Ch.B., director of the Center for Cancer and Immunology Research at Children’s National, was selected to receive a $25m Cancer Grand Challenges award to tackle solid tumors in children.
(4 min. read)
5. New telehealth command center redefines hospital care
Children’s National opened a new telehealth command center that uses cutting-edge technology to keep continuous watch over children with critical heart disease. The center offers improved collaborative communication to better help predict and prevent major events, like cardiac arrest.
(2 min. read)
6. Monika Goyal, M.D., recognized as the first endowed chair of Women in Science and Health
Children’s National named Monika Goyal, M.D., M.S.C.E., associate chief of Emergency Medicine, as the first endowed chair of Women in Science and Health (WISH) for her outstanding contributions in biomedical research.
(2 min. read)
7. Brain tumor team performs first ever LIFU procedure on pediatric DIPG patient
A team at Children’s National performed the first treatment with sonodynamic therapy utilizing low intensity focused ultrasound (LIFU) and 5-aminolevulinic acid (5-ALA) medication on a pediatric patient. The treatment was done noninvasively through an intact skull.
(3 min. read)
8. COVID-19’s impact on pregnant women and their babies
In an editorial, Roberta L. DeBiasi, M.D., M.S., provided a comprehensive review of what is known about the harmful effects of SARS-CoV-2 infection in pregnant women themselves, the effects on their newborns, the negative impact on the placenta and what still is unknown amid the rapidly evolving field.
(2 min. read)
9. Staged surgical hybrid strategy changes outcome for baby born with HLHS
Doctors at Children’s National used a staged, hybrid cardiac surgical strategy to care for a patient who was born with hypoplastic left heart syndrome (HLHS) at 28-weeks-old. Hybrid heart procedures blend traditional surgery and a minimally invasive interventional, or catheter-based, procedure.
(4 min. read)
10. 2022: Pediatric colorectal and pelvic reconstructive surgery today
In a review article in Seminars in Pediatric Surgery, Marc Levitt, M.D., chief of the Division of Colorectal and Pelvic Reconstruction at Children’s National, discussed the history of pediatric colorectal and pelvic reconstructive surgery and described the key advances that have improved patients’ lives.
(11 min. read)













 Children’s National Hospital in Washington, D.C., was ranked No. 5 nationally in the U.S. News & World Report 2022-23 Best Children’s Hospitals annual rankings. This marks the sixth straight year Children’s National has made the list, which ranks the top 10 children’s hospitals nationwide. In addition, its
Children’s National Hospital in Washington, D.C., was ranked No. 5 nationally in the U.S. News & World Report 2022-23 Best Children’s Hospitals annual rankings. This marks the sixth straight year Children’s National has made the list, which ranks the top 10 children’s hospitals nationwide. In addition, its