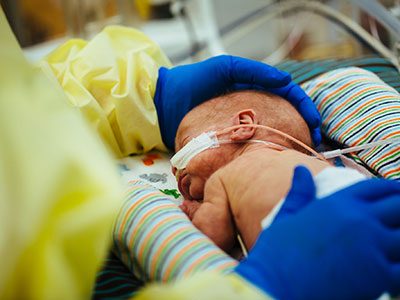
Ten-year-old Angioletta was clinically diagnosed with rheumatic heart disease in 2014 (severe leakage of her mitral valve). She’s been medically managed at the clinic Children’s helps support and conducts research at in Gulu, and she is a very active participant in the support group led by Children’s National research assistant, Amy Scheel. Angioletta hasn’t had any major complications, but her only hope for long-term survival is to undergo open heart surgery to replace her abnormal valve. Experts are looking towards the research from the new Center to help prevent future generations of children like Angioletta from developing RHD.
Known as the ‘world’s forgotten disease,’ Rheumatic Heart Disease (RHD) is caused by untreated streptococcal throat infections that progress into acute rheumatic fever (ARF) and eventually weaken the valves of the heart. It is the most common cardiovascular disease in children and young adults globally – affecting nearly 33 million people and causing 345,000 deaths annually – yet, it is preventable with early detection and access to penicillin.
To help end the epidemic, Children’s National Health System has been awarded a $3.7 million grant from the American Heart Association (AHA) to launch a Rheumatic Heart Disease Center, with the goal of developing innovative strategies and economic incentives to improve the prevention and diagnosis of RHD in high-risk, financially disadvantaged countries and low-income communities across the United States.
Children’s National is one of four centers in the AHA’s Strategically Focused Children’s Research Network, which is dedicated to improving children’s heart health and reducing the global burden of cardiovascular disease and stroke. AHA selected Children’s for the grant based on its proven record of global collaboration to solve complex health issues and the potential impact of this research. The program will use Children’s robust telemedicine infrastructure to connect co-collaborators around the world, as well as train the next generation of globally minded cardiovascular researchers.
“While it’s often thought that we’ve already beaten rheumatic heart disease, data shows there’s nearly no decrease in mortality rates in low-income countries. The disease is endemic in Sub-Saharan Africa, and some poverty-stricken communities in the U.S. are hit nearly as hard,” said Craig Sable, M.D., associate division chief of cardiology. “We are thrilled to receive this funding from the AHA, which will help us close the research gap for this neglected disease and change the plight of millions of children around the world.”
About the center and research focus areas
Over the next four years, the Rheumatic Heart Disease Center, led by Children’s National Heart Institute experts Dr. Sable and Andrea Beaton, M.D., cardiologist, along with RHD leaders around the globe, will develop evidence-based strategies to strengthen the health system’s response to RHD through synergistic basic, clinical and population science research along the entire spectrum of the disease.

The Rheumatic Heart Disease Center, led by Children’s National Heart Institute experts Andrea Beaton, M.D., and Craig Sable, M.D., along with RHD leaders around the globe, will develop evidence-based strategies to strengthen the health system’s response to RHD.
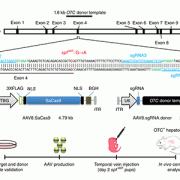
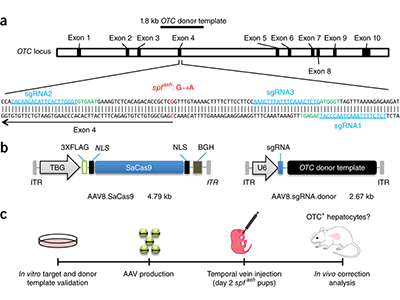
The basic research project, led by James Dale, M.D., chief of the division of infectious disease at the University of Tennessee in Memphis, will work to better define the immune system response to Group A Streptococcal (GAS) infection, or strep throat, paving the way for vaccine development. In collaboration with a partner site in Cape Town, South Africa, experts will recruit 300 children ages 5-15 to participate for 24 months in a study capturing and classifying various strains of the GAS bacteria. Similar to the common flu, the strains of GAS bacteria vary from region to region and year to year. By identifying immune system targets, or how our bodies fight GAS, the research can inform the creation of effective and long-lasting vaccines.
Dr. Beaton will lead the clinical project that will work to improve understanding and detection of ARF, the precursor to RHD. According to Dr. Beaton, the current, outdated paradigm is that patients with RHD at one point experienced a full-blown episode of ARF – including fever, severe joint pains and rash. These symptoms should be unmistakable and prompt treatment, but in truth the disease remains vastly underdiagnosed in high-risk regions. Through an on-the-ground partnership with experts at Mulago National Referral Hospital in Uganda, the clinical project will work to enroll over 1,000 children ages 3-18 with more subtle symptoms, potentially suggestive of ARF, in order to paint a more accurate picture of the disease in Africa today.
“The gap between the low number of children diagnosed with ARF and the high number of young adults with advanced RHD remains one of the most challenging mysteries and barriers to improved RHD prevention,” said Dr. Beaton. “For the first time, we will systematically characterize the clinical, laboratory and echocardiographic features of ARF in low-resource settings, with the goal of developing a biological signature for ARF that can be translated into a diagnostic test and improve detection.”
Dr. Beaton expects that this research could benefit other related diseases too, such as kidney disease or serious skin infections.
The population research project, led by David Watkins, M.D., M.P.H., an expert in epidemiological and economic modeling at the University of Washington in Seattle, will work to build an economic case for prevention around the world, using the data from the basic and clinical work. The goal is to identify local gaps in delivery of health services for disease prevention and treatment and to measure the cost-effectiveness of RHD interventions, as well as the cost of inaction – especially as patients suffering from advanced RHD are often in the prime of their productive, adult lives. Researchers anticipate the findings will provide effective tools for addressing RHD in other endemic countries too.