Think tank improves care for Malawian children with seizures, epilepsy
Global health leaders from Children’s National Hospital joined Malawian clinical experts in a two-day think tank to improve the care of children with seizures in the southern African nation. Details were published recently in a perspective in the American Journal of Tropical Medicine and Hygiene.
“The meeting was eye-opening,” said Douglas Postels, M.D., a pediatric neurologist and faculty member with the Center for Translational Research at Children’s National. “Outcomes are changed when we collaborate directly and work through the best solutions for clinical care in low-resource settings. You must weigh what clinics need, what they can implement, and the impact on public health.”
The big picture
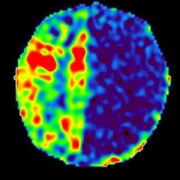
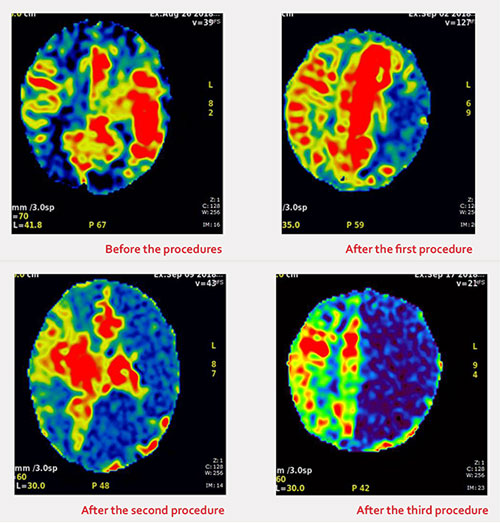
Dr. Postels does research and provides clinical care at Queen Elizabeth Central Hospital (QECH), the largest public hospital in Malawi. “Queen’s” is the only medical setting in a country of over 20 million people where an electroencephalogram (EEG) and specialty pediatric neurology services are available. QECH is an essential — and often overtaxed — component of neurological care in Malawi. Cerebral malaria, epilepsy and seizures from birth asphyxia drive the need for neurological evaluations.
EEG is available at QECH for all hospitalized children and is principally used to evaluate for subclinical seizures in those who are comatose. One of three trained technicians acquires the EEG, which is electronically sent to the United States for interpretation. Under best-case scenarios, the turnaround time between EEG collection and interpretation from a neurologist in the U.S. is about two hours. However, many obstacles can slow results, including misaligned schedules across time zones, internet outages and other complications.
With the support of the Center for Translational Research, Dr. Postels brought five U.S.-based colleagues to Africa to meet with Malawian clinicians to better understand local clinical care needs. A think tank of U.S. and Malawian clinicians worked together to consider research directions and priorities for neurology care and EEG services. Their conversation focused extensively on integrating technology in the places where it will be most clinically useful.
The fine print
Dr. Postels’ research group aims to aid in the clinical care of Malawian children with epilepsy and to make EEG accessible outside of Queen’s hospital. They hope to eventually create a point-of-care EEG system, linking a method of EEG acquisition that requires little training to apply with a software-based interpretation system.
Expanding the use of EEG in Malawi and throughout Africa has numerous clinical applications. Malawian clinicians hoped that EEG could be made available at their local hospitals and folded into a more comprehensive care algorithm for children at risk of seizures — “one aspect of a ‘packet of care’ that included better overall understanding of seizures, criteria for administration of antiseizure medications, and transfer to the central hospital,” according to the journal article.
Malawian clinicians were also interested in using EEG to detect increased intracranial pressure after head trauma, as neuroimaging services are nearly as rare as EEG in Malawi. One pediatrician also wanted to use EEG to guide the treatment of neonatal seizures, which are common in children with birth asphyxia, and to use EEG as a prognostic biomarker.
“We hope to empower Malawian clinicians with clinical research skills and experiences so that they can lead and direct future discussions with patients, parents and stakeholders to advance neurologic care and research in their country,” Dr. Postels and his team wrote.
To dive deeper, read the complete perspective — “Establishing Priorities for Epilepsy Care and Electroencephalogram Use in Low-Resource Settings” — in the American Journal of Tropical Medicine and Hygiene.