Fueling pediatric breakthroughs through collaboration

Teams from HoloUS, CM-eX and Bearables were selected as winners.
At the latest research and innovation mixer hosted at Children’s National Hospital’s Research & Innovation Campus, the energy in the room felt more like a startup demo day than a hospital meeting. In tandem with the hospital’s Innovation Acceleration Network (IAN), an initiative designed to connect clinicians, researchers and engineers who might not otherwise collaborate, the mission of the event was to support pediatric innovators and accelerate early-stage technologies that often struggle to find funding or institutional backing.
Through small pilot awards and a pitch competition, funded by the Alliance for Pediatric Device Innovation’s FDA P50 grant, innovators can receive between $20,000 and $50,000 to push their projects forward. Since its inception, more than 300 devices and concepts have moved through the initiative at various stages of development.
This year, six finalists represented a range of specialties that took the stage before a panel and audience, including engineers, researchers and director of the Fischell Institute of Biomedical Devices. Each presenter had a few minutes to make their case and take questions about their devices and market strategy. Projects pitched included:

Dr. Julia Finkel speaks to kick off the pitch competition at the Children’s National Research and Innovation campus on Thursday, February 19th, 2026
- HoloUS, a device that projects live ultrasound images directly into a proceduralist’s line of sight. Rather than glancing back and forth between a patient and a screen, clinicians can see imaging data seamlessly integrated into their field of vision. Early clinical studies suggest the approach could improve speed, safety and ergonomics. Though competitors exist in the ultrasound visualization space, the HoloUS team emphasized what sets them apart: a simpler, broader visualization strategy designed specifically for procedural use. Still in the research phase, the device is already gaining traction.
- OtoBud, a non-invasive intracranial pressure monitoring system. Monitoring brain pressure traditionally requires invasive procedures — something especially concerning in pediatric populations. Forearm fractures are among the most common injuries in children, yet determining the right treatment plan can be time-consuming and inconsistent. OtoBud aims to offer a low-burden, trendable alternative that requires minimal training while delivering meaningful clinical insights.
- FFAIRS,the Forearm Fracture AI-Driven Recommendation System, a prototype designed specifically for pediatric patients. Unlike many competitors that focus primarily on diagnosis, FFAIRS concentrates on treatment recommendations. The tool is currently in development, and the team is applying for NIH STTR Phase II funding. Outpatient clinics, urgent care centers and primary care practices are among the intended users.
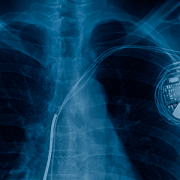
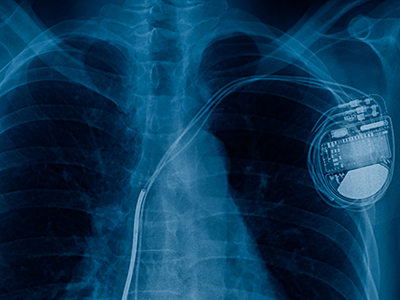
- CM-eX, a tool that safely removes insertable cardiac monitors (ICMs). Long-term heart rhythm monitoring is critical for some pediatric patients, but no dedicated tool currently exists for efficient device extraction. CM-eX aims to reduce procedure time and tissue trauma. After testing synthetic skin analogues and progressing animal models, the team is working toward a safer, more streamlined approach.
- Bearables, a tool that can secure gastrostomy tubes quickly and safely. The device can be applied in under five seconds and is manufactured in-house. The team is preparing for a pilot clinical study and plans to pursue FDA registration before bringing the product to market. Early trials have shown promising results.
- A proposed device seeks to offer faster, more actionable data during cardiac arrest. Currently, no device provides near-continuous diastolic blood pressure readings during resuscitation. Existing tools can be slow, limiting clinicians’ ability to adjust care in real time.

Finalist teams share their solutions with judges and attendees before three projects were selected to receive pilot funding support.
At the end, three projects were selected as the winners: HoloUS, CM-eX and Bearables, each receiving $25K.
These are not abstract concepts or distant possibilities. They are emerging technologies born from clinicians at Children’s National who see daily challenges and refuse to accept the status quo.
Through the Innovation Acceleration Network, Children’s National is doing more than funding devices. It is building a collaborative culture where pediatric-specific innovation thrives — and where ideas designed for the smallest patients can make the biggest difference.