Rewriting the script for sickle cell disease
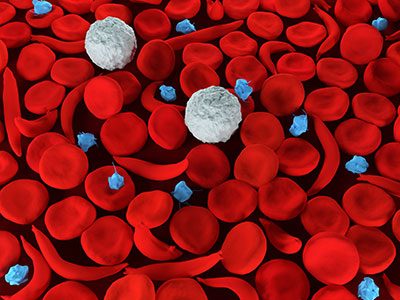
More than 100,000 Americans have sickle cell disease, an inherited blood disorder that can cause excruciating pain crises and shorter life expectancies.
Children’s National has one of the largest sickle cell programs in the United States. We are pioneering treatments and provide specialized care to about 1,500 patients each year. We participate in clinical trials to improve outcomes, shorten treatment time, reduce complications and minimize the need for opioids and chemotherapy.
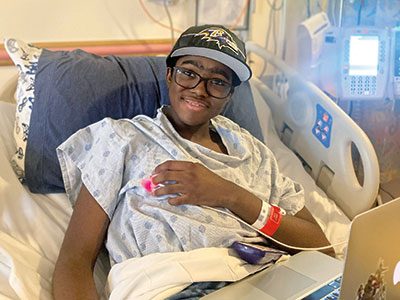
Kendric receives care at Children’s National.
In recognition of our clinical and research excellence, Children’s National was one of a few U.S. pediatric hospitals selected to offer two promising new FDA-approved gene therapies.
Hematologist Robert Sheppard Nickel, M.D., leads a study to reduce toxicities in bone marrow transplants. “Years of development led to these curative therapies,” Dr. Nickel says. “I hope in the future we can safely cure more children with sickle cell disease.”
“The future looks promising to revolutionize the lives of our patients and make these therapies accessible worldwide,” says Andrew Campbell, M.D., director of our Comprehensive Sickle Cell Disease Program.
Kendric and Nasir find hope
In May 2024 at Children’s National, 12-year-old Kendric of Clinton, Maryland, became the world’s first patient with sickle cell disease to begin a commercially approved gene therapy that could dramatically reduce or even eliminate his pain. It involved extracting his bone marrow stem cells; genetically modifying them in a specialized lab to reduce the risk of sickling; and then, after chemotherapy, infusing them back into his bloodstream.
Expert, compassionate care empowered Kendric to understand the science behind his treatment and chart a path to recovery. “My care team taught me how to deal with my disease and everything that I need to know for the future,” he says. “They gave me hope that I could be cured.”

Nasir and his care team.
Nasir, age 20, spent his childhood waiting to find a match for a stem cell transplant to address his sickle cell disease. Finally, in 2023, at Children’s National, he found an answer in gene therapy to alter his own cells.
Due to painful episodes and the need for frequent blood transfusions, both Kendric and Nasir missed out on a lot of school, important moments with friends and simply being kids. Now, they can explore a world in which patients like themselves can overcome this disease and reclaim their health.
“I have all of this oxygen and energy that came out of nowhere,” Nasir says. “It’s really a new life. I feel reborn.”
“The network of doctors at Children’s National gave us reassurance and lots of hope,” says Kendric’s mom, Deborah. “They made us feel like family. We are in awe of how quickly things moved and how much compassion they have shown us.”
Read more stories like this one in the latest issue of Believe magazine.