International projects spearheaded by Children’s National Neurology leaders
NIH approves grant for clinical trial on pediatric cerebral malaria in Malawi
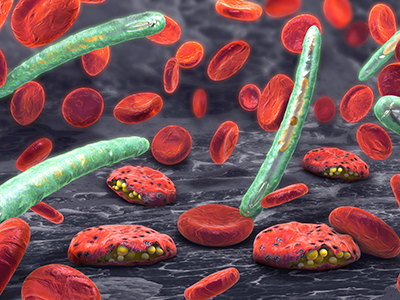
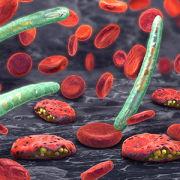
Cerebral malaria, when patients lapse into coma after developing a malaria infection, is the most severe neurological complication of infection with Plasmodium falciparum.
The National Institutes of Health (NIH) approved a $5.8 million grant for a Phase I/IIa randomized clinical trial of 6-diazo-5-oxo-L-norleucine (DON), a new medication for pediatric cerebral malaria. Douglas Postels, M.D., neurologist at Children’s National Hospital, will serve as the trial’s principal investigator. The clinical trial will enroll participants in Blantyre, Malawi.
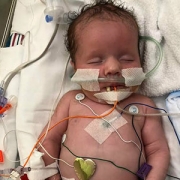
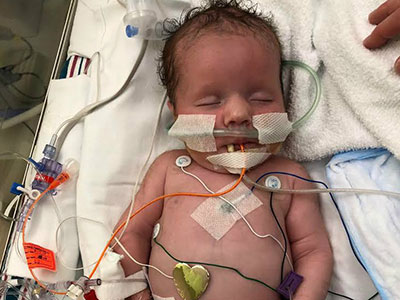
More than 400,000 people die each year from malaria. Cerebral malaria, when patients lapse into coma after developing a malaria infection, is the most severe neurological complication of infection with Plasmodium falciparum. Many children who survive are left suffering from neurological complications because of the disease, leaving some unable to walk, see or go to school. Dr. Postels and others are seeking to initiate this clinical trial with the primary goal to save lives and improve the quality of life for children who survive the disease.
“The purpose of this study is to see if DON is safe in the Malawian population,” Dr. Postels said, noting that adult participants will be enrolled in the first year and children subsequently. “Once the medication has proven to be safe, our intention is to expand this research elsewhere in Africa allowing us to enroll more children and evaluate whether DON decreases the likelihood of death or neurological disability in pediatric cerebral malaria.”
DON was originally tested 50 years ago as an anti-cancer agent but was recently repurposed by the National Institute of Allergy and Infectious Diseases (NIAID) for pediatric cerebral malaria. The current clinical trial is a collaborative project with the NIAID scientists who performed the pre-clinical testing with DON.
“There are currently no adjunctive treatments, used in combination with intravenous anti-malarial medications, that decrease death or disability in pediatric cerebral malaria,” Dr. Postels said. “Our hope is that DON will be the “magic bullet” that helps these critically ill children.”
Improving access to epilepsy care in Ethiopia
Over the next three years, Tesfaye Zelleke, M.D., neurophysiologist at Children’s National Hospital, the Comprehensive Pediatric Epilepsy Program team and the Children’s National Global Health Initiative will create a sustainable program to reduce the epilepsy treatment gap in Ethiopia in collaboration with the Ethiopian Ministry of Health.
In a three-tier approach, the program is looking to help children in the country benefit from the increased access to the treatment and care for epilepsy, the most common neurologic disorder affecting about 1% of the population.
Ethiopia is one of the poorest countries in Africa with very limited access to epilepsy care — there are a handful of pediatric neurologists for a population of over 120 million. Only few referral hospitals have neurology clinics and those clinics are largely concentrated in Addis Ababa, the capital city. Improving access to epilepsy care in resource poor countries like Ethiopia would require utilizing non-neurologist providers, a task-shifting model.
“In the first year, we will focus on creating an epilepsy center of excellence, training of trainers (local non-neurologist providers), create treatment guidelines for epilepsy, and produce health education material for families and public,” said Dr. Zelleke. “In the subsequent years, we plan to expand to other areas outside of Addis Ababa — the Ethiopian capital — and collaborate with epilepsy advocacy groups to continue to increase access to care.”
After the three years, Dr. Zelleke and the team have envisioned working closely with the country’s Ministry of Health to further the impact of the project at a national level.