Comprehensive study reveals long-term COVID-19 impacts on children
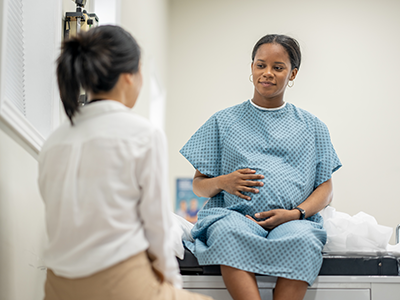
A new ongoing study is tracking the long-term impacts of COVID-19 on children, uncovering key differences in symptoms, physical fitness, and quality of life.
Long-term impacts of SARS-CoV-2 (COVID-19) infection on children remain poorly understood, especially compared to adults. This ongoing longitudinal study evaluates a diverse, prospective, multi-center cohort to track pediatric outcomes over three years, comparing children with a history of COVID-19 to uninfected peers. The initial cross-sectional analysis revealed infected children were more likely to report fatigue, respiratory and gastrointestinal symptoms, and showed reduced performance in areas such as physical function, sleep and cognitive health. These findings underscore the need for continued investigation to uncover the full scope of COVID-19’s effects on children’s health and development. This study is ongoing jointly at the National Institute of Allergy and Infectious Diseases (NIAID), National Institutes of Health (NIH) in Bethesda, MD, and Children’s National Hospital.
How will this work benefit patients?
In this initial analysis, researchers assembled a large and diverse cohort of children and adolescents representing a range of ages, sexes, races, and ethnicities, ensuring that the findings were generalized to the pediatric population affected by COVID-19. They discovered several notable findings specific to infected participants, compared to their uninfected peers that warranted closer monitoring. For instance, non-specific gastrointestinal symptoms appeared to be a unique feature of infected pediatric participants.
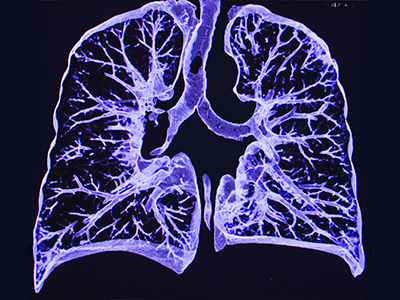
Reports of persistent fatigue and shortness of breath did not correlate with radiological findings or abnormalities in cardiopulmonary evaluations. However, older adolescent infected participants (>16 years) demonstrated poorer performance on the six-minute walk test (6MWT) compared to their uninfected peers. The 6MWT is a simple, age-validated test widely used in clinical settings to assess aerobic activity tolerance, endurance, and overall cardiopulmonary fitness in both adult and pediatric populations, including those with chronic cardiovascular and pulmonary conditions and post-COVID-19 syndromes. These findings merit further evaluation, as it could indicate early signs of reduced endurance or exercise tolerance in this group.
Overall, no statistically significant differences were observed between cohorts in radiographic imaging, pulmonary function or cardiac diagnostic findings. However, there were non-statistically significant trends, such as a higher frequency of ECG ST-segment abnormalities and a greater incidence of abnormal echocardiogram findings among infected participants. Additionally, no differences were observed between the two groups regarding cardiovascular symptoms, such as dizziness and fainting. Over the three-year evaluation period, researchers aim to determine whether signs of dysautonomia develop or if changes in cardiac function emerge in children recovering from acute COVID-19. Baseline psychosocial, quality-of-life and developmental survey data further highlight the importance of including uninfected participants for comparison.
While previous studies have suggested anxiety and depression as features of pediatric post-acute sequelae of COVID (PASC)/long COVID, our study shows that anxiety, depressive symptoms, and difficulties with peer relationships were reported by parents and participants in similar proportions across both cohorts. These findings may reflect the broader social isolation experienced during the pandemic. In contrast, other psychosocial domains—such as global health, physical functioning and mobility, cognitive functioning, pain interference, fatigue and sleep disturbances—showed worsening symptoms unique to infected participants. This study design allows for a more nuanced understanding of the psychosocial and developmental impacts specific to COVID-19.
How does this work move the field forward?
This study highlights that a proportion of children with COVID-19 develop post-acute sequelae of COVID infection, which is often underdiagnosed in medically underserved areas due to the greater burden of acute illness in these communities. By improving community education, diagnosis and management of pediatric PASC, this research aims to reduce health, educational and socioeconomic disparities, paving the way for more equitable care and outcomes for affected children.
What are you hoping to discover?
“Ongoing study of this cohort will help identify COVID-19’s long-term effects in children, assess immune responses and protective immunity, and uncover genetic or immunologic factors tied to outcomes,” said Roberta DeBiasi, MD, MS, chief of Pediatric Infectious Diseases. “Future research using the biorepository will also explore disease mechanisms and biomarkers of pediatric COVID-19, which may lead to identification of targeted treatments”
You can read the full study, Pediatric SARS-CoV-2 Long Term Outcomes Study: Baseline Characteristics, in the Pediatric Research Journal.
Additionally, Children’s National leads a unique multidisciplinary clinic for children experiencing Long COVID symptoms and has cared for over 300 children to date. For more information about the clinic, click here.










 A clinical trial testing a new drug to increase growth in children with short stature. The first ever high-intensity focused ultrasound procedure on a pediatric patient with neurofibromatosis. A low dose gene therapy vector that restores the ability of injured muscle fibers to repair. These were among the most popular articles we published on Innovation District in 2022. Read on for our full top 10 list.
A clinical trial testing a new drug to increase growth in children with short stature. The first ever high-intensity focused ultrasound procedure on a pediatric patient with neurofibromatosis. A low dose gene therapy vector that restores the ability of injured muscle fibers to repair. These were among the most popular articles we published on Innovation District in 2022. Read on for our full top 10 list.


 A group of children’s hospitals from across the country will coordinate on the response to future pandemics and other disasters through a new $29 million grant from the Health Resources and Services Administration (HRSA). The group, known as the Pediatric Pandemic Network (PPN), will focus on the unique needs and challenges to children during pandemics and disasters, ensuring that health equity is at the forefront of emergency planning.
A group of children’s hospitals from across the country will coordinate on the response to future pandemics and other disasters through a new $29 million grant from the Health Resources and Services Administration (HRSA). The group, known as the Pediatric Pandemic Network (PPN), will focus on the unique needs and challenges to children during pandemics and disasters, ensuring that health equity is at the forefront of emergency planning.
 Adolescents with attention-deficit/hyperactivity disorder (ADHD) report greater hesitancy and less confidence in COVID-19 vaccine safety compared to adolescents without ADHD, a
Adolescents with attention-deficit/hyperactivity disorder (ADHD) report greater hesitancy and less confidence in COVID-19 vaccine safety compared to adolescents without ADHD, a 







