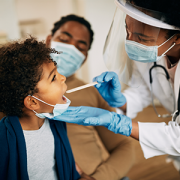
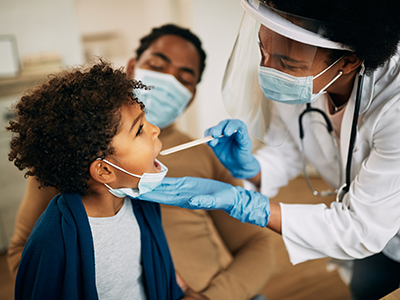
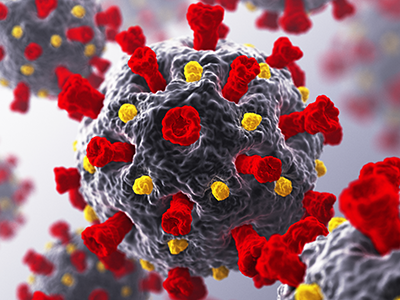
Genomic medicine, diversity, equity and inclusion (DEI), a world post-COVID-19 and pediatric research funding were among the topics discussed during the “Special Fireside Chat” keynote lecture at the 2021 Children’s National Hospital Research, Education and Innovation Week.
Francis S. Collins, M.D., Ph.D., director at the National Institutes of Health (NIH), is well known for his landmark discoveries of disease genes and his leadership of the international Human Genome Project, which culminated in April 2003 with the completion of a finished sequence of the human DNA instruction book.
The President and CEO of Children’s National, Kurt Newman, M.D., joined Dr. Collins during the “Special Fireside Chat” keynote lecture. Dr. Newman posed several health care-related questions to Dr. Collins over the course of 30 minutes. Dr. Collins’s responses shed light on what it takes to advance various research fields focused on improving child health and develop frameworks that advocate for DEI in order to foster a more just society.
Q: You have been involved with genomic medicine since its inception. You discovered the gene causing cystic fibrosis and led the Human Genome project. What do you see as the future of genomic medicine, especially as it relates to improving child health?
A: Thank you for the question, Kurt. First, I wanted to say congratulations on your 150th anniversary. Children’s National Hospital has been such a critical component for pediatric research and care in the Washington, D.C., area, and at the national and international levels. We at the NIH consider it a great privilege to be your partner in many of the things that we can and are doing together.
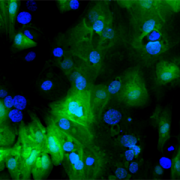
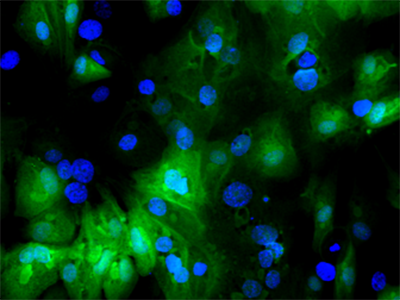
Genomic medicine has certainly come a long way. The word genomics was invented in 1980, so we have not been at this for that long. Yet, the success of the Human Genome Project and the access to cost-effective tools for rapid DNA sequencing have made many things possible. It took a lot of effort, time and money to discover the gene that causes cystic fibrosis. Kurt, if you look at what we did, while it was rewarding, it was a challenging problem that occupied the hearts of the scientific community in 1980. Now, a graduate student at Children’s National that has access to DNA samples, a thermal cycler, a DNA sequencer and the internet could do in about a week what it took us a decade and with 50 people.
We have been able to rocket forward as far as identifying the genetic causes of 6,500 diseases, where we know precisely the molecular glitch responsible for those conditions. While most of those are rare diseases, it leads to the opportunity for immediate diagnosis, which used to be a long and troubled journey.
DNA sequencing has increasingly become an essential tool in newborns, especially when trying to sort out puzzling diagnosis for specific syndromes or phenotypes that are not immediately clear. Additionally, DNA sequencing significantly impacted clinical care in cancer because it made it possible to look at the mutations driving the malignancy and its genetic information that can lead to interventions. This approach is going forward in the next few years in ways that we can see now. Although I am a little reluctant to make predictions because I have to be careful about that, it may be possible to obtain complete genome sequences that can be yours for life and place them into the medical record to make predictions about future risks and choices about appropriate drugs. This path costs less than any imaging tests.
Q: The racial justice movement that was brought back to the forefront this past year has, once again, reaffirmed that this country has so much more work to do in order to end systemic racism. You have been at the forefront of promoting diversity, equity and inclusion in research and at the NIH. What do you and the NIH plan to do further DEI efforts in research and in general so that we can be a more just and equitable society?
A: I appreciate you raising this, Kurt. Diversity, equity and inclusion (DEI) is an issue where everyone should be spending a lot of time, energy and passion. You are right. 2020 will be remembered for COVID-19. I also think it will be remembered for the things that occurred around the killing of George Floyd, and the recognition of the very foundation that is still infected by this terribly difficult circumstance of structural racism. I convened a group of about 75 deep thinkers about these issues, many of them are people of color from across the NIH’s different areas of activities. I asked the group to come forward with a bold set of proposals. This effort is how the program UNITE came together to work hard on this, which is now making recommendations that I intend to follow. We are determined to close that gap and pursue additional programs that will allow us to be more successful in recruiting and retaining minority groups, for example. We need to do something with our health disparity and research portfolio as well to ensure that we are not just looking around the edges of the causes for racial inequities. We are digging deeper into what the structural racism underpinnings are and what we can do about it. I am particularly interested in supporting research projects that test intervention and not just catalog the factors involved. We have been, at times, accused and maybe rightly so of being more academic about this, and, less kindly, we have been accused of admiring the problem of health disparities as opposed to acting on it. We are ready to act.
Q: COVID has affected us all in so many ways. Could you tell us what this past year has been like for you? Also, how is the NIH preparing for a soon-to-be post-COVID pandemic?
A: This is the time to contemplate the lessons learned as everyone knows that the last worst pandemic happened over a century ago. One thing that maybe will vex us going forward, which we already started to invest in a big way, is this whole long COVID syndrome, also referred to post-acute sequelae, to understand precisely the consequences and mechanisms like Multisystem Inflammatory Syndrome in Children (MIS-C). Before moving to the next pandemic, we must think about how we will help understand those who suffer from long COVID syndrome. As far as the broader lessons learn, Kurt, we must expect that there will be other pandemics because humans are interacting more with animals, so zoonosis is likely to emerge. We need to have a clear sense of preparation for the next one. For instance, we are working on this right now, but we need to have a stronger effort to develop small molecules of anti-viral drugs aimed at the major viral classes, so we do not have to start from scratch. We also need clinical trial networks warm all the time, ready to go and to learn how valuable public partnerships can be to get things done in a hurry.
Editor’s Note: The responses in this Q+A have been modified to fit the word count.