Honor bestowed on Nathan Kuppermann, MD, MPH

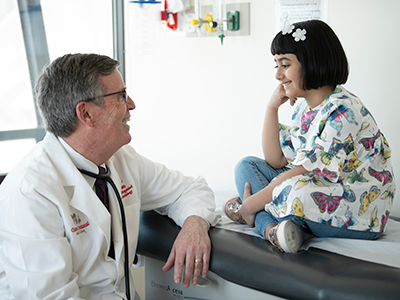
Children’s National Hospital named Nathan Kuppermann, MD, MPH, the Fight For Children Distinguished Chair of Academic Medicine at Children’s National.
Children’s National Hospital named Nathan Kuppermann, MD, MPH, the Fight For Children Distinguished Chair of Academic Medicine at Children’s National.
Dr. Kuppermann serves as executive vice president and chief academic officer at Children’s National. He is the director of the Children’s National Research Institute and the chair of the Department of Pediatrics and associate dean of Pediatric Academic Affairs at the George Washington University School of Medicine and Health Sciences.
The big picture
Dr. Kuppermann joins a distinguished group of Children’s National physicians and scientists who hold endowed chairs. Children’s National is grateful to generous donors who have funded 49 professorships.
Professorships support groundbreaking research and innovation on behalf of children and their families and foster new discoveries and therapies in pediatric medicine. These appointments carry prestige and honor that reflect the recipient’s achievements and donor’s commitment to advancing and sustaining knowledge.
Why it matters
Dr. Kuppermann is a pediatric emergency medicine physician, clinical epidemiologist and leader in emergency medical services for children. He specializes in clinical trials and clinical prediction rules using large cohorts of acutely ill and injured children. He is world-renowned for his research and mentorship.
“I was drawn to Children’s National by its nationally recognized work and dedication to innovation and team science,” says Dr. Kuppermann. “I’m eager to contribute to the remarkable work being done in both the research and education space to continue to improve the understanding, prevention and treatment of childhood diseases.”
Fight For Children’s support ensures that Dr. Kuppermann and future holders of this professorship will launch bold, new initiatives to rapidly advance pediatric medical research, elevate our leadership and improve the lives of children in our community and around the world.
Moving the field forward
Fight For Children was founded in 1990 by the late Joseph (Joe) E. Robert, Jr., with the mission of improving the lives of underserved children in the nation’s capital. The organization has impacted the lives of more than 400,000 young people throughout the D.C. metropolitan area.
Fight For Children endowed the Fight For Children Chair in Academic Medicine in 1997 to support the clinical research initiatives of the Chief Academic Officer. Most recently, in 2019, they made a $5M gift to create the Fight For Children Sports Medicine Center at Children’s National. It is the region’s first site dedicated to the orthopedic surgery, sports medicine and comprehensive concussion needs of young athletes.
Joe Robert was an entrepreneur and visionary who believed in the importance of investing in children through education and healthcare. His largest gift to Children’s National created and endowed our Joseph E. Robert, Jr., Center for Surgical Care. He was also instrumental in developing the Sheikh Zayed Institute for Pediatric Surgical Innovation at Children’s National, created in 2009 with a $150 million gift from the government of Abu Dhabi.
“Joe’s legacy continues to be represented through the incredible work being done at Children’s National,” says David Fensterheim, chairman and interim CEO of Fight For Children. “Dr. Kuppermann is a pioneer in pediatric healthcare. We are proud to honor his cutting-edge vision as the latest holder of this prestigious professorship.”
This professorship embodies Joe’s legacy and Fight For Children’s commitment to inspire others to think bigger and differently to advance pediatric healthcare for children in the community and beyond.