Tag Archive for: Catherine Bollard
Personalized T cell therapy for HIV shows safety and early signs of impact

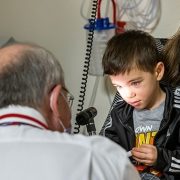
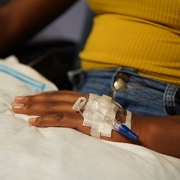
A new HIV-specific T cell therapy, tested in six adults living with HIV, used specially trained immune cells made from each person’s own blood — a personalized therapy designed to target the virus with precision.
An exciting small clinical trial led by the Center for Cancer and Immunology Research at Children’s National Hospital has shown that a new HIV-specific T cell therapy is safe and may help reduce hidden reservoirs of the virus in the body. This approach, tested in six adults living with HIV, uses specially trained immune cells made from each person’s own blood — a personalized therapy designed to target the virus with precision.
The results, published in Nature Communications, represent a step forward in the search for a long-term, drug-free way to control or even cure HIV.
A smarter way to fight HIV
Today, people living with HIV rely on anti-retroviral therapy (ART) to keep the virus under control. These medications are highly effective but must be taken daily and do not eliminate the virus entirely. That is because HIV can hide in a “reservoir” of cells where it remains dormant and invisible to both drugs and the immune system. If ART is stopped, the virus can quickly return.
To change that, scientists at Children’s National and partnering institutions developed a new type of cellular therapy called HST-NEETs — short for “HIV-specific T cells targeting conserved epitopes”. These T cells are trained in the lab to recognize parts of the virus that do not change much, even as HIV mutates. This makes it harder for the virus to escape. The goal is to help the immune system find and destroy the infected cells that are normally hidden.
Safe and promising results
In this phase 1 clinical trial, researchers created personalized HST-NEET therapy from each participant’s own immune cells. After training the cells to recognize HIV, they were infused back into the patients twice over a period of weeks.
The results showed that:
- No serious side effects were reported from the infusions.
- The treatment was well-tolerated by all six participants.
- In two people, the therapy led to stronger HIV-specific immune responses, including more virus-fighting T cells and antibodies.
- In two others, researchers saw a drop in the level of HIV hidden in their cells, a sign that the virus reservoir might be shrinking.
- In four participants, the infused T cells persisted in the bloodstream for up to 40 weeks, continuing to patrol for signs of HIV.
While not a cure, these findings show early evidence that the therapy may help the body better recognize and fight HIV, even the hidden forms that are hardest to treat.
Building toward a cure
“The fact that we saw HIV-specific T cell responses increase in some participants, even without additional immune-boosting drugs, is very encouraging,” said Catherine Bollard, MBChB, MD, senior author of the study and director of the Center for Cancer and Immunology Research at Children’s National. “It suggests that the immune system can be trained to go after parts of the virus that were previously out of reach.”
Unlike bone marrow transplants, which have led to a cure in a few people with both HIV and cancer but carry high risk, HST-NEET therapy is much safer and more scalable. That is important for the millions of people living with HIV worldwide.
This study also sets the stage for future clinical trials that could combine T cell therapy with other strategies, like latency-reversing drugs that “wake up” hidden HIV, to further shrink the reservoir. It also shows that personalized T cells can be safely made, infused and tracked over time and that they can continue working in the body for many months. Those lessons are valuable not just for HIV but also for developing safer, more targeted cancer immunotherapies in children and adults.
What’s next
The next phase of research will evaluate this therapy in larger groups and under different conditions, including in people undergoing stem cell transplants or with added immune system boosters. Clinical trials are already underway exploring these combinations.
By focusing on preserved parts of the virus, the regions that HIV cannot easily mutate, HST-NEETs could one day become part of a combination approach to eliminate HIV from the body altogether.
“Every step brings us closer to a functional cure,” said Dr. Bollard. “And the lessons we’re learning from HIV may also inform how we treat other chronic viral infections, and even cancer, in the future.”
Authors authors from Children’s National include Danielle K. Sohai, Michael D. Keller, Patrick J. Hanley, Fahmida Hoq, Divyesh Kukadiya, Anushree Datar, Emily Reynolds, Christopher Lazarski, Chase D. McCann, Jay Tanna, Abeer Shibli, Haili Lang, Anqing Zhang, Pamela A. Chansky, Cecilia Motta and Conrad Russell Y. Cruz.
REI Week 2025 empowers the future in pediatric research and innovation
Children’s National Hospital hosted its fifteenth annual Research, Education and Innovation Week from March 31–April 4, 2025, bringing together clinicians, scientists, educators and innovators from across the institution to celebrate discovery and collaboration. This year’s theme, “Empowering the Future in Pediatric Research and Innovation with Equity, Technology and a Global Reach,” served as a call to action for advancing science that improves child health both locally and around the world.
Each day of the week-long event featured thought-provoking lectures — now available to watch — dynamic panel discussions, interactive workshops and vibrant poster sessions, all highlighting the diverse and interdisciplinary work taking place across Children’s National.
Centering the patient and the planet
REI Week began on Monday with a powerful keynote lecture from Lynn R. Goldman, MD, MS, MPH, Michael and Lori Milken dean of the Milken Institute School of Public Health at the George Washington University. In her talk, “Children: Uniquely vulnerable to climate-related threats,” Dr. Goldman underscored the urgent need to protect children from the environmental hazards of a changing climate and to integrate climate science into pediatric care and advocacy.
At mid-morning, Mary-Anne “Annie” Hartley, MD, PhD, MPH, director of the LiGHT Laboratory at École Polytechnique Fédérale de Lausanne, introduced the “MOOVE” platform — Massive Open Online Validation and Evaluation of clinical LLMs. Her talk demonstrated how artificial intelligence, when rigorously validated, has the potential to transform clinical decision-making and global health equity.
Monday’s final keynote, “Zinc and childhood diarrhea,” was presented by Christopher Duggan, MD, MPH, director of the Division of Nutrition at Harvard Medical School. Dr. Duggan highlighted the global health impact of zinc supplementation in reducing childhood mortality — a reminder that simple, evidence-based interventions can save millions of lives.
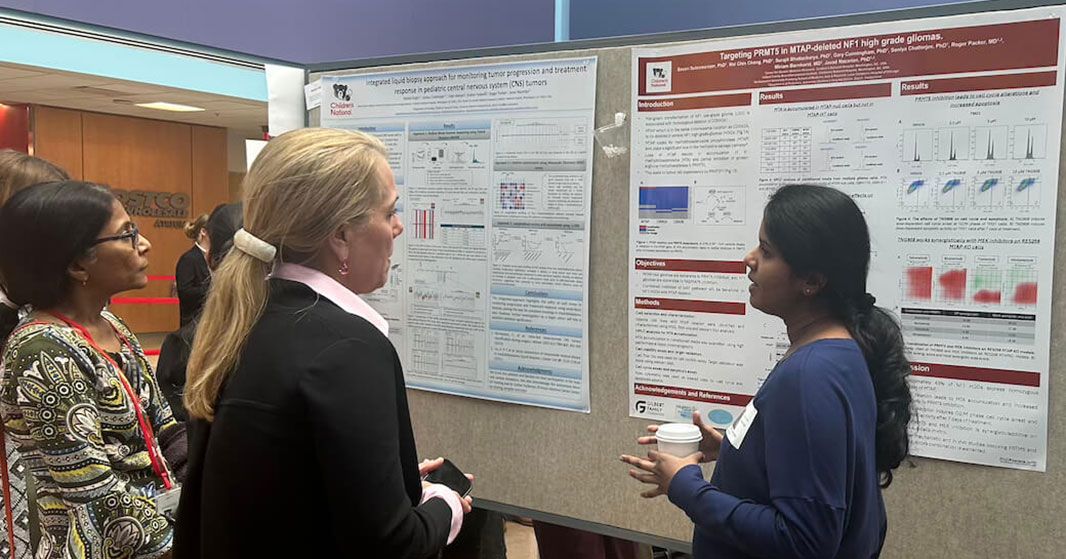
In that first day, the first poster session of the week showcased projects in adolescent medicine, global health, infectious diseases, oncology and more. The session reflected the full breadth of research taking place across Children’s National.
Ambroise Wonkam, MD, PhD, professor of genetic medicine at Johns Hopkins University, then delivered Tuesday’s Global Health Keynote Lecture, “Harnessing our common African genomes to improve health and equity globally.” His work affirmed that inclusive genomics is key to building a healthier world.
Later, the Global Health Initiative event and GCAF Faculty Seminar encouraged attendees to pursue collaborative opportunities at home and abroad, reflecting the growing global footprint of Children’s National research programs.
Transforming education and care delivery
On Wednesday, Larrie Greenberg, MD, professor emeritus of pediatrics, kicked off the day with a Grand Rounds keynote on educational transformation: “Shouldn’t teachers be more collaborative with their learners?” He followed with a CAPE workshop exploring the effectiveness of case-based learning.
The Nursing Sponsored Keynote Lecture by Vincent Guilamo-Ramos, PhD, MPH, LCSW, ANP-BC, PMHNP-BC, FAAN, explored “Redesigning the U.S. broken health system.” He offered an urgent and inspiring call to reimagine pediatric care by addressing social determinants of health.
In the Jill Joseph Grand Rounds Lecture, Deena J. Chisolm, PhD, director of the Center for Child Health Equity at Nationwide Children’s Hospital, challenged attendees to move beyond dialogue into action in her talk, “Health equity: A scream to a whisper?,” reminding researchers and clinicians that advocacy and equity must be foundational to care.
The day continued with a poster session spotlighting medical education, neonatology, urology and neuroscience, among other fields.
Posters and pathways to progress
Throughout the week, poster sessions highlighted cutting-edge work across dozens of pediatric disciplines. These sessions gave attendees the opportunity to engage directly with investigators and reflect on the shared mission of discovery across multiple disciplines, including:
- Neuroscience and Neuroprotection – Novel approaches to brain injury treatment and neurodevelopmental disorders.
- Genetics and Precision Medicine – Advances in understanding genetic predisposition and innovative therapies.
- Health Disparities and Global Health – Strategies to bridge gaps in pediatric healthcare access worldwide.
- Innovative Technology in Pediatrics – Breakthroughs in AI, bioinformatics and medical device development.
Honoring excellence across Children’s National
The REI Week 2025 Awards Ceremony celebrated outstanding contributions in research, mentorship, education and innovation. The winners in each category were:
POSTER SESSION AWARDS
Basic & Translational Research
Faculty: Benjamin Liu, PhD
“Genetic Conservation and Diversity of SARS-CoV-2 Envelope Gene Across Variants of Concern”
Faculty: Steve Hui, PhD
“Brain Metabolites in Neonates of Mothers with COVID-19 Infection During Pregnancy”
Faculty: Raj Shekhar, PhD
“StrepApp: Deep Learning-Based Identification of Group A Streptococcal (GAS) Pharyngitis”
Post docs/Fellows/Residents: Dae-young Kim, PhD
“mhGPT: A Lightweight Domain-Specific Language Model for Mental Health Analysis”
Post docs/Fellows/Residents: Leandros Boukas, MD, PhD
“De Novo Variant Identification From Duo Long-Read Sequencing: Improving Equitable Variant Interpretation for Diverse Family Structures”
Staff: Naseem Maghzian
“Adoptive T Lymphocyte Administration for Chronic Norovirus Treatment in Immunocompromised Hosts (ATLANTIC)”
Graduate Students: Abigail Haffey
“Synergistic Integration of TCR and CAR T Cell Platforms for Enhanced Adoptive Immunotherapy in Brain Tumors”
High School/Undergraduate Students: Medha Pappula
“An ADHD Diagnostic Interface Based on EEG Spectrograms and Deep Learning Techniques”
Clinical Research
Faculty: Folasade Ogunlesi, MD
“Poor Air Quality in Sub-Saharan Africa is Associated with Increase Health Care Utilization for Pain in Sickle Cell Disease Patients”
Faculty: Ayman Saleh, MD
“Growth Parameters and Treatment Approaches in Pediatric ADHD: Examining Differences Across Race”
Post docs/Fellows/Residents: Nicholas Dimenstein, MD, MPH
“Pre-Exposure Prophylaxis (PrEP) Eligibility in the Pediatric Emergency Department”
Staff: Tayla Smith, MPH
“The Public Health Impact of State-Level Abortion and Firearm Laws on Health Outcomes”
Graduate Students: Natalie Ewing
“Patterns of Bacteriuria and Antimicrobial Resistance in Patients Presenting for Primary Cloacal Repair: Is Assisted Bladder Emptying Associated with Bacteriuria?”
Graduate Students: Manuela Iglesias, MS
“Exploring the Relationship Between Child Opportunity Index and Bayley-III Scores in Young Children”
High School/Undergraduate Students: Nicholas Lohman
“Preliminary Findings: The Efficacy, Feasibility and Acceptability of Group Videoconference Cognitive Behavioral Therapy with Exposure and Response Prevention for Treating Obsessive-Compulsive Disorder Among Children and Young People”
Community-Based Research
Faculty: Sharon Shih, PhD
“Assessing Pediatric Behavioral Health Access in DC using Secret Shopper Methodology”
Post docs/Fellows/Residents: Georgios Sanidas, MD
“Arrested Neuronal Maturation and Development in the Cerebellum of Preterm Infants”
Staff: Sanam Parwani
“Intersectionality of Gender and Sexuality Diversity in Autistic and Non-Autistic Individuals”
Graduate Student: Margaret Dearey
“Assessing the Burden of Period Poverty for Youth and Adolescents in Washington, DC: A Pilot Study”
Quality and Performance Improvement
Faculty: Nichole L. McCollum, MD
“A Quality Improvement Study to Increase Nurse Initiated Care from Triage and Improve Timeliness to Care”
Post docs/Fellows/Residents: Hannah Rodriguez, MD
“Reducing Unnecessary Antibiotic Use in a Level IV NICU”
Staff: Amber K. Shojaie, OTD, OTR/L
“Implementing Dynamic Axilla Splints in a Large Burn Patient”
MENTORSHIP AWARDS
Basic Science Research
Conrad Russell Y. Cruz, MD, PhD
Clinical Research
Bench to Bedside Research
Ioannis Koutroulis, MD, PhD, MBA
ELDA ARCE TEACHING SCHOLAR AWARD
SUZANNE FEETHAM NURSING RESEARCH SUPPORT AWARD
Eileen P. Engh, PhD RN
“Rare Disease Organization Lifecycle” Role in Helping Parents with Everyday Life Information Seeking and Connection (RDO-HELIX)
EXPLORATIONS IN GLOBAL HEALTH PILOT AWARDS
Launchpad Awards
Mi Ran Shin, MD, MPH
“Establishing Interdisciplinary Rehabilitation for Birth and Burn Injuries in Ethiopia”
Susan Harvey, MSN, CPNP-AC
“Implementation of Sickle Cell Pilot Program in Ndhiwa Sub County, Kenya”
Meleah Boyle, PhD, MPH
“Understanding and Addressing Environmental Sustainability to Protect the Health of the Children’s National and Global Communities”
Eiman Abdulrahman, MD
“Research Capacity Building to Improve Pediatric Emergency and Critical Care in Ethiopia”
Pilot Awards
Alexander Andrews, MD
“EEG as a Diagnostic and Prognostic Marker in Severe Pediatric Malaria, Blantyre Malawi”
Daniel Donoho, MD & Timothy Singer, MD
“Feasibility Study of a Novel Artificial Intelligence-Based Educational Platform to Improve Neurosurgical Operative Skills in Tanzania”
Hasan Syed, MD
“Bridging the Gap an Educational Needs Assessment for Pediatric Neurosurgery Training in Pakistan”
Sofia Perazzo, MD & Lamia Soghier, MD, MEd, MBA
“QI Mentorship to Improve Pediatric Screening and Follow-up in Rural Argentina”
Benjamin Liu, PhD
“AI-Empowered Real-Time Sequencing Assay for Rapid Detection of Schistosomiasis in Senegal”
Rae Mittal, MD
“Assessment and Enhancement of Proficiency in Emergency Child Neurology Topics for Post-Graduate Emergency Medicine Trainees in India”
Innovation Day ignites bold thinking
Thursday, REI Week shifted to the Children’s National Research & Innovation Campus for Innovation Day, a celebration of how bold ideas and collaborative culture can accelerate progress in pediatric medicine.
Brandy Salmon, PhD, associate vice president of Innovation and Partnerships at Virginia Tech, opened the day with “The Alchemy of Innovation,” focusing on how institutions can build a culture that fuels transformative partnerships.
A multidisciplinary panel discussion moderated by Nathan Kuppermann, MD, MPH, and Catherine Bollard, MBChB, MD, featured Nehal Mehta, MD, Julia Finkel, MD, Kevin Cleary, PhD, Ioannis Koutroulis, MD, PhD, MBA, Francesca Joseph, MD and Patrick Hanley, PhD, who shared how innovation can be advanced and promoted, especially as a core institutional priority.
A shared vision for the future
REI Week 2025 reaffirmed the values that define Children’s National: a commitment to excellence, collaboration and equity in pediatric research and care. As discoveries continue to emerge from our hospital and our research campuses, the connections built and ideas sparked during this week will help shape the future of pediatric health — locally and globally.
By elevating voices from the bedside to the bench, with the support of the executive sponsors Nathan Kuppermann, MD, MBChB, Catherine Bollard, MBChB, MD, Kerstin Hildebrandt, MSHS, Linda Talley, MS, RN, NE-BC and David Wessel, MD, REI Week demonstrated that we must embrace the community in all aspects of our work. Because we know that there are answers we can only get from the patients that we serve—and we need to be their voice.
Research, Education & Innovation Week will be back next year on April 13-17, 2026.
Posters at the REI Week 2025 Monday, March 31 poster session.

Panelists discuss innovation during REI Week 2025.

Global Health Initiative community engagement event during REI Week 2025.

Chris Rees presents his REI Week 2025 lecture.

Nathan Kuppermann listens to a presenter during the REI Week 2025 Tuesday, April 1, poster session.

Michelle Riley-Brown, Nathan Kuppermann, Catherine Bollard and Naomi Luban on stage during the REI Week 2025 awards ceremony.

Brandy Salmon presents on innovation programs at Virginia Tech during the REI Week 2025 Innovation Day.

Catherine Bollard listens to a presenter during the REI Week 2025 Monday, March 21 poster session.
Ambroise Wonkman poses for a picture with Children’s National staff.

Tanzeem Choudhury presenting during REI Week 2025.

Expanded partnership with Virginia Tech accelerates pediatric cancer research
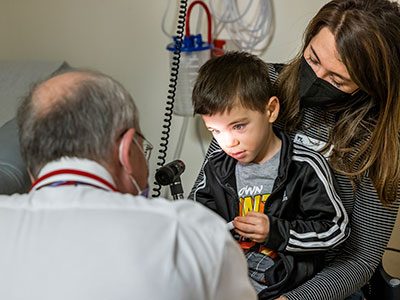
The new partnership will advance pediatric health through innovative discoveries and therapies, with an initial focus on pediatric cancers, including brain tumors.
Children’s National Hospital and Virginia Tech are expanding their research partnership, building on a successful collaboration established in 2019. This partnership will advance pediatric health through innovative discoveries and therapies, with an initial focus on pediatric cancers, including brain tumors.
The partnership brings together Children’s National, ranked among the nation’s top pediatric hospitals by U.S. News & World Report, and Virginia Tech, a leading academic research institution. Together, they aim to deliver transformative advancements to enhance outcomes for children facing devastating diagnoses.
The goals of the research-focused partnership include:
- Accelerating the understanding of the biology, improvements in prevention and treatment of pediatric cancers and other childhood diseases.
- Developing new diagnostic and therapeutic tools to improve care for children.
- Training the next generation of scientists and physician-scientists.
What they’re saying
- “Over the years, our partnership with Virginia Tech has demonstrated the power of combining top-tier research expertise with a shared commitment to improving pediatric health,” said Catherine Bollard, MBChB, MD, senior vice president and chief research officer and director of the Center for Cancer and Immunology Research. “This expansion underscores our belief that by working together, we can accelerate discoveries and develop life-changing therapies for children with cancer and other rare diseases.”
- “Children’s National Hospital has been an important partner for us in biomedical research and innovation,” said Michael Friedlander, PhD, Virginia Tech vice president for health sciences and technology. “Our collaboration deepened with the launch of Children’s National Research & Innovation Campus in Washington, D.C., and now, as our partnership grows even stronger, we’re poised together to take on some of the biggest challenges in cancer research to contribute to the health of children and adults.”
- “Partnering with Children’s National connects us to a world-class clinical trial institute that has been a pioneer in treating brain tumors with focused ultrasound technology, and this presents a unique opportunity to help children and families struggling with cancer,” said Cheng-Chia “Fred” Wu, MD, PhD, a member of the Children’s National Brain Tumor Research Institute and a principal investigator in cancer research and faculty member at the Fralin Biomedical Research Institute in Roanoke and in the Virginia Tech Carilion School of Medicine.“I can’t wait to see where this takes us.”
Big picture
The initial focus of the collaboration is pediatric cancers, including brain tumors — among the most challenging childhood diagnoses. By combining Virginia Tech’s leading-edge technology and research infrastructure with Children’s National’s expertise in pediatric care, the organizations aim to make significant strides in understanding these diseases.
An interdisciplinary approach is at the heart of the ongoing strategy. The collaboration first began with the launch of a 12,000-square-foot Virginia Tech biomedical research facility within the Children’s National Research & Innovation Campus, which opened in 2020. Located on a 12-acre portion of the former Walter Reed Army Medical Center in Washington, D.C., the campus was the nation’s first innovation hub focused exclusively on pediatric research.
Regional powerhouse: Cell and Gene therapy leaders from mid-Atlantic forge connections
Posters at the REI Week 2025 Monday, March 31 poster session.

Panelists discuss innovation during REI Week 2025.

Global Health Initiative community engagement event during REI Week 2025.

Chris Rees presents his REI Week 2025 lecture.

Nathan Kuppermann listens to a presenter during the REI Week 2025 Tuesday, April 1, poster session.

Michelle Riley-Brown, Nathan Kuppermann, Catherine Bollard and Naomi Luban on stage during the REI Week 2025 awards ceremony.

Brandy Salmon presents on innovation programs at Virginia Tech during the REI Week 2025 Innovation Day.

Catherine Bollard listens to a presenter during the REI Week 2025 Monday, March 21 poster session.

Ambroise Wonkman poses for a picture with Children’s National staff.

Tanzeem Choudhury presenting during REI Week 2025.

Nearly 200 biomedical leaders from Washington, D.C., Maryland, and Virginia gathered at the Children’s National Research & Innovation Campus for the 2nd annual Cell & Gene Therapy Symposium. The event showcased groundbreaking developments in rare disease treatments and underscored the importance of regional collaboration.
“By targeting diseases at the cellular level, we are on the cusp of breakthroughs in cell and gene therapy that will transform medicine,” said Catherine Bollard, M.D., M.B.Ch.B., director of the Center for Cancer and Immunology Research (CCIR) at Children’s National Hospital and a host of the symposium. “Progress will accelerate if we build partnerships beyond our own organizations.”
The big picture
Scientists and clinicians have worked for more than two decades to develop cell and gene therapies aimed at treating diseases on a cellular level. The past few years have been particularly promising as investment in science has led to advancements. Children’s National is at the forefront, as one of the first pediatric hospitals in the world to offer commercial gene therapies for sickle cell disease.
Many more treatments for rare diseases are in development at Children’s National and beyond. Leaders at CCIR are actively building collaborations with companies, academic institutions and enterprises across the mid-Atlantic region to accelerate these efforts.
During the symposium, Eugene Hwang, M.D., chief of Oncology at Children’s National, addressed the urgent need for more effective and less toxic treatments for pediatric brain tumors. He highlighted the potential of combining immunotherapies with innovations like low-intensity focused ultrasound, which can open the blood-brain barrier temporarily to improve drug delivery to tumors.
“With collaboration between the lab and clinic, alongside industry partners and even between hospitals, we can finally make strides I haven’t seen in my entire career,” Dr. Hwang said. “It’s an incredibly inspiring time for all of us.”
Why it matters
Experts from organizations as diverse as MaxCyte, ScaleReady, RoosterBio, PSC Biotech, Qiagen, FujiFilm and the Frederick County Office of Economic Development came together for the daylong conversation.
Michael Friedlander, Ph.D., executive director of the Fralin Biomedical Research Institute at Virginia Tech, emphasized the critical role of regional partnerships in fulfilling the potential of these emerging therapies. He pointed to the collaborative research between Children’s National and Virginia Tech on brain tumors, where bioengineers and cancer researchers are working side-by-side to create new treatments.
“We are now able to begin delivering these leading-edge therapies to patients,” Dr. Friedlander said. “For example, those who live in rural settings often have much less access to such frontline medical innovations. By collaborating with Children’s National and gaining access to urban pediatric populations, as well as patients in our more rural area, we can start to bring these therapies to a much broader audience.”
What’s next
Patrick Hanley, Ph.D., chief and director of the Cellular Therapy Program at Children’s National, observed that other regions in the U.S. are uniting to advance scientific discoveries with the backing of government, academia and industry. He hopes to see similar collaboration across the D.C., Maryland, and Virginia area, known as the DMV. Children’s National is leading an initiative called CHARM – the Capital Health and Mid-Atlantic Regenerative Medicine – to bring regional experts together for webinars, networking events and partnership opportunities.
“There’s significant interest in cell and gene therapy worldwide,” said Dr. Hanley, a symposium host. “I see an even greater interest in creating cell and gene therapy hubs. The time is right for our mid-Atlantic region, and I’m excited to see what unfolds in the next five years.”
Access4Kids: A new model to pay for pediatric cell and gene therapies
Science is pioneering cures for pediatric rare diseases in a coming wave of new cell and gene therapies. However, the biopharmaceutical industry’s insistence on large patient populations and high profit margins may prevent these life-saving treatments from reaching the children who desperately need them. When successful therapeutics fail to see commercialization, experts say they have fallen into the “Valley of Death.”
To address this, leaders from pediatric healthcare, federal organizations, academia, industry and patient advocacy groups gathered at the Children’s National Research & Innovation Campus. Their objective: build a new framework to deliver these transformative drugs to clinics worldwide.
Meet the team forming Access4Kids, a nonprofit whose mission is to build new pathways to pay for cures and provide hope to children with life-limiting diseases. This group is working to change medicine and how we pay for it, under the leadership of Catherine Bollard, M.D., M.B.Ch.B., director of the Children’s National Center for Cancer and Immunology Research, Crystal Mackall, M.D., director of the Stanford Center for Cancer Cell Therapy, Julie Park, M.D., Oncology Department chair at St. Jude Children’s Research Hospital, and Alan Wayne, M.D., pediatrician-in-chief at Children’s Hospital Los Angeles.
Expanding team innovates to take on pediatric brain tumors

Cheng-Chia “Fred” Wu, M.D., Ph.D., joins the team at the campus as an assistant professor at Virginia Tech’s Fralin Biomedical Research Institute. Image credit: Fralin Biomedical Research Institute.
Experience, talent and technology are coming together at the Children’s National Research & Innovation Campus to solve the complex challenges of treating pediatric brain tumors through a growing partnership between Children’s National Hospital and Virginia Tech.
Cheng-Chia “Fred” Wu, M.D., Ph.D., joins the team at the campus as an assistant professor at Virginia Tech’s Fralin Biomedical Research Institute. He hopes to improve treatment for pediatric brain tumors and other cancers by leveraging technological advances in focused ultrasound and studying how this modality can be combined with other novel therapies. Children’s National physicians and scientists are collaborating with Virginia Tech scientists to develop these new approaches.
Why we’re excited
Catherine Bollard, M.D., M.B.Ch.B., director of the Center for Cancer and Immunology Research and interim chief academic officer at Children’s National, said collaborations — including the partnership between Children’s National and Virginia Tech — are essential to solving formidable scientific challenges.
“We are thrilled to be working with Dr. Wu to develop cutting-edge therapeutics for pediatric brain tumors,” Dr. Bollard said. “With Dr. Wu’s experience and the talents of our team at Children’s National, I have great hope that we will be able to combine our novel technologies and therapies to provide tremendous breakthroughs for treating pediatric patients with brain tumors.”
Before joining Virginia Tech, Dr. Wu was an assistant professor of radiation oncology at Columbia University Irving Medical Center in New York, where he treated pediatric cancers and central nervous system malignancies.
“Partnering with Children’s National connects us to a world-class clinical trial institute that has been a pioneer in treating brain tumors with focused ultrasound technology, and this presents a unique opportunity to help children and families struggling with cancer,” Dr. Wu said. “I can’t wait to see where this takes us.”
Dr. Wu played a key role in the Initiative for Drug Delivery Innovation for Childhood Brain Tumors at Columbia, developing a bench-to-bedside platform to facilitate the translation of promising technologies for targeted drug delivery in children with brain tumors.
Within three years, the team demonstrated the safety and feasibility of using focused ultrasound in the brainstem and adding radiation in preclinical models. They then opened two clinical trials for kids with relapsed diffuse midline glioma, an aggressive and difficult-to-treat brain tumor that occurs in the brain stem, thalamus and spinal cord.
What’s ahead
Dr. Wu will be involved in a wide range of research touching both organizations, including veterinary medicine and biomedical engineering at Virginia Tech.
Michael Friedlander, Ph.D., executive director of the Fralin Biomedical Research Institute at Virginia Tech Carilion and vice president for health sciences and technology at Virginia Tech, welcomed Dr. Wu’s experience as a pediatric radiation oncologist, translational physician-scientist and clinical trialist who has led an innovative drug delivery program.
“He is armed with a unique set of skills to identify promising new technology and implement it in areas of great need for treatment of pediatric cancers,” Dr. Friedlander said. “We are absolutely delighted to have Dr. Wu as part of the team. He represents a powerful new part of the strong partnership between Virginia Tech and Children’s National Hospital for addressing pediatric brain cancer.”
Closing the ‘Valley of Death’: Pioneering – and paying for – new therapies

“To cure brain tumors, sickle cell disease and scores of other illnesses that have an outsized impact on pediatric patients, we will need an innovative mechanism to ensure that money is not a barrier to scientific advancement and world-class care,” says Dr. Bollard.
With the advent of life-changing cell and gene therapies (CGTs) to treat pediatric diseases, price is becoming a significant obstacle to care and cures.
Successful therapies can wind up shelved or in hard-to-reach clinical trials for a litany of reasons: high manufacturing costs, significant regulatory burdens, a lack of enthusiasm from the pharmaceutical industry in the small pediatric market and the simple fact that insurance companies resist paying the price of $1 million or more for a therapeutic. When successful treatments are set aside and become victims of this market failure, leaders in pediatric medicine say the drug has been relegated to the “Valley of Death.”
Experts at Children’s National Hospital and other leading U.S. research institutions are working to ferry drugs across it.
A new way forward
The Access4Kids think tank is bringing together healthcare leaders to chart another way – with its hosts Catherine Bollard, M.D., M.B.Ch.B., director of the Children’s National Center for Cancer and Immunology Research, Crystal Mackall, M.D., director of the Stanford Center for Cancer Cell Therapy, Julie Park, M.D., Oncology Department chair at St. Jude Children’s Research Hospital, and Alan Wayne, M.D., pediatrician-in-chief at Children’s Hospital Los Angeles. Organized at the Children’s National Research & Innovation Campus, the think tank will include voices from Seattle Children’s Hospital in Washington state and the Moonshot Presidential Office in Washington, D.C., along with experts from academic institutions, the federal government and patient advocacy groups.
They explained their vision in their recent Nature Medicine perspective, “Enhancing pediatric access to cell and gene therapies.” One idea under consideration is to create a biotech enterprise – backed by public monies, foundations and philanthropies – to support the late-stage development and commercialization of pediatric CGTs. Called a Pediatric Advanced Medicines Biotech (PAMB), this new organization would follow a novel pathway outside the traditional biopharma development model.
“To cure brain tumors, sickle cell disease and scores of other illnesses that have an outsized impact on pediatric patients, we will need an innovative mechanism to ensure that money is not a barrier to scientific advancement and world-class care,” Dr. Bollard said. “My colleagues and I aren’t exaggerating when we say this is a ‘save the world’ effort. It’s an initiative to disrupt the pharmaceutical industry and impact medicine, ultimately saving lives and entire lifetimes.”
The think tank is the second in a series aimed at solving this formidable challenge. Led by scientists, the work goes to the heart of healthcare economics.
“We need to find a way to support the academic ecosystem by reducing costs, creating efficiencies in manufacturing and working with regulatory bodies to bolster business models that lead to safe and effective therapeutics,” Dr. Mackall said. “We went to school to study science and medicine. Now, our mission includes revamping business models, as we find ways to increase access to lifesaving treatments for children in need.”
Why it matters
Creating novel pathways to pay for CGTs presents a challenge and an opportunity for researchers in pediatrics and rare diseases. Drs. Mackall, Bollard and their colleagues are exasperated when scientists discover successful treatments for life-threatening illnesses, but market forces lock the drug away in hard-to-reach clinical trials or – even worse – land it on a shelf.
Consider just one example, laid out in the Nature Medicine perspective: Children with adenosine deaminase-deficient severe combined immunodeficiency (ADA-SCID) lack nearly all protection from viruses, bacteria and fungi, leaving them vulnerable to a world of opportunistic organisms. Researchers at San Raffaele Telethon Institute for Gene Therapy in Italy won U.S. and European regulatory approvals for a gene replacement therapy to treat the life-threatening disorder. Yet currently the therapy is only available in clinical trials, with support from research grants, philanthropic donations and institutional resources.
“This happens to successful therapeutics, and it’s heartbreaking. The current business model in medicine can lead to situations where successful therapies have extremely restricted availability, and there are no built-in guarantees of sustained access,” Dr. Bollard said. “We can and must do better – and we believe we have a way forward.”
Novel cell therapy treatments offer promise to immune-compromised children
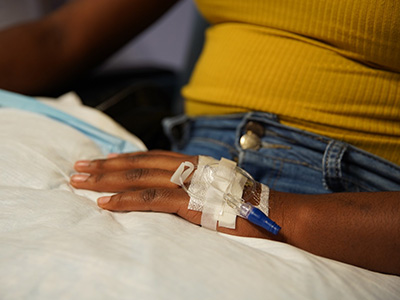
In a first-of-its-kind clinical trial, researchers found that intravenous therapies made from virus-specific T-cells (VST) can effectively treat immunocompromised pediatric patients, far surpassing the current standard of care, according to new research published in Nature Communications.
More than 60% of patients in the phase 2 clinical trial led by investigators from Children’s National Hospital and Huntsman Cancer Institute responded to the innovative VST therapy. This new treatment uses blood from healthy donors to manufacture a highly specialized immune therapy that, when given to immune-compromised patients, prompts their immune system to fight off potentially life-threatening viruses, including cytomegalovirus, Epstein-Barr and adenovirus. Without this therapy, estimates suggest that less than 30% of patients would recover, using standard protocols.
“A vast majority of our patients not only responded to the therapy, but they were able to come off their antivirals, which come with extensive side effects,” said Michael Keller, M.D., the paper’s first author and the Translational Research Laboratory director at the Children’s National Cell Enhancement and Technologies for Immunotherapy (CETI) program. “This promising data suggests hope for patients with rare immune-compromising diseases that leave them vulnerable to so much in the world.”
The study brings together experts from the Pediatric Transplantation and Cell Therapy Consortium (PTCTC) and the Primary Immune Deficiency Treatment Consortium (PIDTC) to create the first multi-center, pediatric-consortium trial of adoptive T-cell therapies for viruses. It also represents one of the first to include critically ill patients, who are often excluded from research.
Children’s National leads the way
Working alongside Catherine Bollard, M.D., M.B.Ch.B., director of the Center for Cancer and Immunology Research (CCIR), Dr. Keller and the CCIR team helped build an internationally recognized program, pioneering therapies to prevent complications from viral infections in immunocompromised patients. This includes patients with congenital immune deficiency and others who have undergone bone marrow transplantation for malignancies or non-malignant conditions, such as sickle cell disease.
While doctors can treat some immune-compromised patients for infections with standard antivirals, a small fraction don’t respond. Children’s National is one of a handful of hospitals in the country that has options. Over the last several decades, researchers have found ways to develop VST therapies made from banked T-cells, a more advanced application of how donated red blood cells are used to treat anemia.
In 2017, Drs. Keller and Bollard started collaborating with Michael Pulsipher, M.D.—now with Intermountain Primary Children’s Hospital and the Huntsman Cancer Institute at the University of Utah—to create a multi-institute clinical study. They combined the expertise at Children’s National in producing and banking cell therapy products with the community built around the PTCTC. Ultimately, they launched a clinical trial that was open to 35 centers in the U.S., enrolling 51 patients at 22 hospitals from 2018-2022.
“We wanted to prove that this potentially life-saving therapy could be given safely at regional pediatric centers that had never been able to use this approach before,” said Dr. Pulsipher, who served as the study’s co-principal investigator with Dr. Keller. “We united top experts in this area from the PTCTC and PIDTC and successfully treated some of the most challenging patients ever treated with this approach. Our findings helped define who can benefit the most from this therapy, paving the way for commercial development.”
The Good Manufacturing Practices (GMP) laboratory at Children’s National, led by Patrick Hanley, Ph.D., provided suitable VST therapies for 75 of 77 patients who requested to join the study. Clinical responses were achieved in 62% of patients who underwent stem cell transplants and in 73% of patients who were treated with VST and evaluated one month after their infusion. The paper laid out risks and clinical factors impacting outcomes when third-party donors are used to manufacture the VST therapies.
What’s ahead
Given that researchers are only beginning to develop cell therapies, work remains to understand the many ways they interact with the immune system. In a separate paper also recently published in Nature Communications, members of the multi-institute team documented a case of an infant with severe combined immune deficiency, who faced extremely rare side effects when the VST treatment interfered with her donor bone marrow graft. The case led the team to work with the Food and Drug Administration to identify criteria for VST donors enrolled in this study to mitigate complications.
In the decade ahead, Dr. Bollard sees promise in cell therapies for patients with cancer, immune deficiencies after transplant and dozens of other disorders, including genetic and autoimmune diseases. “Future studies will continue to look at ways to optimize the manufacturing, the administration and the long-term outcomes for these therapies—and to enhance the lifelong impact on our patients,” she said. “When we pair human ingenuity with the power of technology, I see tremendous potential.”
Acknowledgments: This study was funded with a nearly $5 million grant from the California Institute of Regenerative Medicine and was run through the operations center at the Children’s Hospital of Los Angeles, where Dr. Pulsipher was formerly on faculty.
NexTGen team assembles to delve into progress on CAR T-cell therapies
The international NexTGen team assembled at the Children’s National Research & Innovation Campus for their annual meeting to share progress made in their first full year of work on the $25-million Cancer Grand Challenge, focused on creating a CAR T-cell therapy for pediatric solid tumors.
“It was invigorating to bring the whole team together from our eight institutions in the U.S., U.K. and France, as we uncover opportunities in our research and share the headway that we have made,” said Catherine Bollard, M.D., M.B.Ch.B., director of the Center for Cancer and Immunology Research and interim chief academic officer at Children’s National Hospital. “Breakthroughs happen when Team Science collaborates, and that is exactly what is happening here with the NexTGen team.”
Why we’re excited
Over the course of two days, more than 85 team members met to discuss the six work packages that are coming together, with the ambitious goal of making CAR T-cell therapies the standard of care for solid tumors within the next decade:
- Discovery of new targets
- The tumor microenvironment
- Component engineering
- Integration and modeling
- Clinical studies
- Data integration
Each work package includes a patient advocate – individuals with a personal connection to cancer as a family member or survivor – who offers their invaluable perspectives on the research and treatment process. Many attended the meeting, sitting alongside the oncologists, immunologists, mathematicians, molecular biologists and other leading experts.
The big picture
The Cancer Grand Challenges are funded by grants from the National Cancer Institute, Cancer Research U.K. and the Mark Foundation for Cancer Research. Their goal is to drive progress against cancer by empowering global leaders in the research community to take on tough challenges and think differently.
“They call it a ‘grand challenge’ for a reason,” Dr. Bollard said. “It’s going to take the effort and expertise of all these individuals to make a new therapy a reality. I have confidence that we can do it.”
AI team wins international competition to measure pediatric brain tumors

Children’s National Hospital scientists won first place in a global competition to use artificial intelligence (AI) to analyze pediatric brain tumor volumes, demonstrating the team’s ground-breaking advances in imaging and machine learning.
During the International Conference on Medical Image Computing and Computer Assisted Intervention (MICCAI), the Children’s National team demonstrated the most accurate algorithm to study the volume of brain tumors – the most common solid tumors affecting children and adolescents and a leading cause of disease-related death at this young age. The technology could someday help oncologists understand the extent of a patient’s disease, quantify the efficacy of treatments and predict patient outcomes.
“The Brain Tumor Segmentation Challenge inspires leaders in medical imaging and deep learning to try to solve some of the most vexing problems facing radiologists, oncologists, computer engineers and data scientists,” said Marius George Linguraru, D.Phil., M.A., M.Sc., the Connor Family Professor in Research and Innovation and principal investigator in the Sheikh Zayed Institute for Pediatric Surgical Innovation. “I am honored that our team won, and I’m even more thrilled for our clinicians and their patients, who need us to keep moving forward to find new ways to treat pediatric brain tumors.”
Why we’re excited
With roughly 4,000 children diagnosed yearly, pediatric brain tumors are consistently the most common type of pediatric solid tumor, second only to leukemia in pediatric malignancies. At the urging of Linguraru and one of his peers at the Children’s Hospital of Philadelphia, pediatric data was included in the international competition for the first time, helping to ensure that children are represented in medical and technological advances.
The contest required participants to use data from multiple institutions and consortia to test competing methods fairly. The Children’s National team created a method to tap into the power of two types of imaging and machine learning: 3D convolutional neural network and 3D Vision Transformer-based deep learning models. They identified regions of the brain affected by tumors, made shrewd data-processing decisions driven by the team’s experience in AI for pediatric healthcare and achieved state-of-the-art results.
The competition drew 18 teams who are leaders from across the AI and machine learning community. The runner-up teams were from NVIDIA and the University of Electronic Science and Technology of China.
The big picture
“Children’s National has an all-star lineup, and I am thrilled to see our scientists recognized on an international stage,” said interim Executive Vice President and Chief Academic Officer Catherine Bollard, M.D., M.B.Ch.B., director of the Center for Cancer for Immunology Research. “As we work to attack brain tumors from multiple angles, we continue to show our exceptional ability to create new and better tools for diagnosing, imaging and treating these devastating tumors.”
Children’s National announces new professorships

Robert Keating, M.D., Brian Rood, M.D., and Catherine Bollard, M.D., M.B.Ch.B.
Children’s National Hospital named Robert Keating, M.D., as the McCullough Distinguished Professor of Neurosurgery. He serves as the chief of neurosurgery and co-director of the high-intensity focused ultrasound (HIFU) program at Children’s National.
Children’s National Hospital named Brian Rood, M.D., as the Kurt D. Newman, M.D., Professor of Neuro-Oncology. He serves as director of clinical neuro-oncology and medical director of the Brain Tumor Institute at Children’s National.
Children’s National Hospital elevated Catherine Bollard, M.D., M.B.Ch.B., to the Dr. Robert J. and Florence T. Bosworth Distinguished Professor of Cancer and Transplantation Biology Research. She is the Interim Executive Vice President and Chief Academic Officer and Interim Director, Children’s National Research Institute. She also serves as the director of the Center for Cancer and Immunology Research and director of the Program for Cell Enhancement and Technologies for Immunotherapy at Children’s National.
About the awards
Professorships at Children’s National support groundbreaking work on behalf of children and their families and foster new discoveries and innovations in pediatric medicine. These appointments carry prestige and honor that reflect the recipient’s achievements and donor’s forethought to advance and sustain knowledge. Children’s National is grateful for its generous donors, who have funded 47 professorships.
Dr. Keating is a longstanding leader in neurosurgery research and care. His areas of expertise include brain tumors, traumatic brain injuries, craniofacial anomalies, Chiari malformations and spinal dysraphism. With Dr. Keating’s leadership, the neurosurgery department is pioneering innovations such as HIFU, a non-invasive therapy using focused ultrasound waves to ablate a focal area of tissue. It can treat tumors located in difficult locations of the brain, movement disorders and epilepsy. Children’s National was one of the first pediatric hospitals in the nation to use HIFU for neuro-oncology patients.
“Our goal is to elevate our top-ranked program to even greater heights,” says Dr. Keating. “We will continue to use cutting-edge technology and non-invasive approaches to make the knife obsolete in pediatric neurosurgery and improve outcomes for children.”
Dr. Rood studies the biology of pediatric brain tumors. He focuses on protein signatures and biomarkers specific to different types of brain cancers. His study of neoantigens is informing the development of T-cell immunotherapies to target a tumor’s unique proteins.
“Immunotherapy is revolutionizing how we treat childhood brain tumors — safely, effectively and with the precision made possible by using a patient’s own cells,” says Dr. Rood. “This professorship enables our team to advance this revolution, which will save lives and improve lifetimes.”
Dr. Bollard received the Dr. Robert J. and Florence T. Bosworth Professor of Cancer and Transplantation Biology Research in 2018 to support her work to develop cell and gene therapies for patients with cancer and underlying immune deficiencies. Her professorship has been elevated to a distinguished professorship to amplify her research and celebrate her accomplishments in the field of immunotherapy.
About the donor
These appointments were made possible through an extraordinary $96 million investment from an anonymous donor family for rare pediatric brain tumor research and care. It is one of the hospital’s largest donations and will transform the hospital’s ability to give patients with rare brain cancer a better chance at healthy lifetimes.
The anonymous family brings a depth of compassion for children facing rare and often challenging diagnoses. Their partnership will immediately advance every aspect of our globally recognized leadership to create new, more effective treatments.
Their investment also endowed the Professorship in Molecular Neuropathology. We look forward to bestowing that honor on a Children’s National pediatric leader.
In the News: The challenges of pediatric clinical trials
 “Pediatric cancer is rare, when you compare it to other forms of cancer, especially adult solid tumors. Often pharma companies are not wanting to fund trials that are exclusively to support a pediatric cancer indication. This is a question that I get asked a lot: How to deal with the so-called ‘valley of death’? … You can successfully complete a phase 1/phase 2 trial, show a safety and efficacy signal, but then lack the funds to get FDA approval. Several of us in the field are looking at other strategies to fill this gap, like forming consortiums and using institutional support.”
“Pediatric cancer is rare, when you compare it to other forms of cancer, especially adult solid tumors. Often pharma companies are not wanting to fund trials that are exclusively to support a pediatric cancer indication. This is a question that I get asked a lot: How to deal with the so-called ‘valley of death’? … You can successfully complete a phase 1/phase 2 trial, show a safety and efficacy signal, but then lack the funds to get FDA approval. Several of us in the field are looking at other strategies to fill this gap, like forming consortiums and using institutional support.”
Catherine Bollard, M.D., M.B.Ch.B, director of the Center for Cancer and Immunology Research, joined Nature to talk about clinical trials for children, including the significant challenges she and her colleagues face to ensure potentially successful treatments have the funding to make it through the approval process. Learn more about her thoughts on the current landscape for pediatric clinical trials and her work on CAR-T cell therapies in her webinar.
In the news: Novel research to stop pediatric brain tumors
“The team is really bringing in very new ideas from mathematical modeling, engineering, all the way to cell therapy, immunotherapy and immunology…This is what really excites and energizes us to be part of this great team, to address the Cancer Grand Challenge, to better target pediatric solid tumors.”
The Cancer Letter connected with Catherine Bollard, M.D., M.B.Ch.B., director of the Center for Cancer and Immunology Research at Children’s National Hospital, for a conversation about her work as a leader of the Cancer Grand Challenges NexTGen team. The $25 million effort is funded by Cancer Research U.K. and the National Institute of Health’s National Cancer Institute and the Mark Foundation for Cancer Research. Its ambitious goal: find novel therapies to break the stalemate in the treatment of pediatric solid brain tumors in the next 10 years. Bollard shared her work plan and the “secret sauce” that gives the team its edge with The Cancer Letter. Find out more about the hope behind this effort in the full interview here.
In the news: People v. pediatric cancer
“I just want to hammer home the fact that, if you have a child with a pediatric solid tumor who relapses, most likely the chemotherapy that will be treating that child will be the same chemotherapy that a child diagnosed 20 years ago would have received. This is how little progress has been made…. This is what we are trying to change.”
Catherine Bollard, M.D., M.B.Ch.B., director of the Center for Cancer and Immunology Research at Children’s National Hospital, pulled the curtain back on her work fighting pediatric brain tumors at The Atlantic’s People V. Cancer summit. This annual event brings together leading voices from the front lines for in-depth conversations about how to stop this complex and lethal disease. Dr. Bollard discussed the unique importance of collaboration among pediatric oncologists and the optimism she has for using a patient’s immune system to go after solid tumors with CAR T therapies.
Research into a new way to combat solid tumors earns part of a $25M award

Catherine Bollard, M.D., M.B.Ch.B., and Patrick Hanley, Ph.D.
Children’s National Hospital has developed multi-antigen specific T cells that have shown success in pre-clinical models in attacking pediatric solid tumors. Now the promising area of research earned a major boost from the Cancer Grand Challenges — founded in 2020 by the two largest funders of cancer research in the world – Cancer Research UK and the National Cancer Institute in the U.S.
This award supported the foundation of NexTGen, a team of scientists and clinicians with expertise in immunology, proteomics, mathematics and more, across eight institutions in the U.S., U.K. and France. Catherine Bollard, M.B.Ch.B, M.D., director of the Center for Cancer and Immunology Research at Children’s National, and Martin Pule, M.D., clinical associate professor at the University College of London are the co-leads of this effort.
The NexTGen team is one of four Cancer Grand Challenges’ new teams, representing a total investment of $100M to diverse, global teams to take on some of the toughest challenges in cancer research. NexTGen will create a new approach that performs clinical and basic research together to facilitate real-time knowledge exchange from the lab to the clinic and back again.
While the more widely known CAR T-cells have made tremendous progress for patients with B-cell leukemias, lymphomas and other blood cancers, the CAR T-cell field has not made the same impact for adult and pediatric solid tumors.
“A tumor cell is very clever because it tries to hide from the immune system by deleting or down regulating targets that the T cell is directed towards,” said Dr. Bollard.
Dr. Bollard further discusses the importance of having patient voices during the decision-making process in this quest, her hopes for their program and the concept of the combining tumor antigen-specific T cells with CAR-T cells that her team will develop.
Q: Can you explain the NexTGen vision?
A: The overall vision is that we will have developed the next generation of cell therapies to cure children with refractory solid tumors by the end of the five years. It is important to move the field forward, so we wanted to be innovative in our approach to this grand challenge for these children who have no other therapeutic options left.
Q: What are the most three important components of this project?
A: First, science and diplomacy played a significant role in bringing in the right set of investigators from diverse scientific backgrounds. What started as a conversation using the universal language of science, it quickly became an international project to address this complex issue. Second, we worked very hard with our patient advocates during the writing process, and they will be working side by side with the investigators at the bench and clinic. Third, we were the only group to have clinical trials in our proposal starting very early in the grant funding period, which is unprecedented.
Q: Can you describe NexTGen’s research model?
A: From our experience in leukemia, we know that progress is greatly accelerated if discovery occurs hand-in-hand with clinical development. Therefore, unlike classical programs where years of pre-clinical discovery and developmental work is required before the clinical translation, we will take a non-conventional non sequential approach.
Specifically, in the NexTGen Program, clinical development will start early with three cutting-edge clinical studies evaluating engineered T-cell technologies that we have recently developed understanding that there are some questions that can ONLY be answered in the clinic. To that end, clinical and translational data from these clinical trials will be able to feed into and enrich the discovery and pre-clinical science throughout the NexTGen Program in a circular fashion to promote this research program that goes from bedside to bench and back.
Q: How is Children’s National leading the way?
A: Children’s National is leading one of the three clinical trials that combine our non-gene engineered tumor antigen-specific T-cell platform with gene engineered T cells to generate a novel T-cell therapy against relapsed /refractory solid tumors. Combining tumor antigen specific T cells with the CAR T-cell platform represents a novel concept that may have more potency against these hardest to treat tumors in children.
Q: Why is it so important to include the patient voice during the discussion and decision making?
A: Because we are also physicians and scientists, we do not forget the patient and their families. Thus, we have a robust patient advocacy group embedded in this vision. The group will co-develop summaries explaining the challenges NextGen will address, how this will be achieved and how results will be used, with major input in clinical trial design and consent documents as well as key input into how patient tissue samples can be used to facilitate research discoveries. The patient advocacy team will also help find broad representation from multiple geographical locations of advocates with lived experience of different cancer types, including bereaved relatives and cancer survivors. These and many more strategies applied with patient advocacy groups will elevate the call for a broader and accelerated adoption of CAR-T clinical trials to broaden access to all patients.
Q: What excites you most about this?
A: What excites me the most is working with this incredible group of scientists, physicians and patient advocates all with rich and deep expertise who bring together an extensive and diverse knowledge base. The fact that we will be all working together toward a common goal of curing pediatric solid tumors in the next five to 10 years is extraordinarily energizing. This sizeable international collaboration comprises the right talent to get this done. It is also highly exciting to simultaneously have three clinical trials running in parallel with the discovery science and the pre-clinical work. I am extremely optimistic that we will realize NexTGen’s vision to bring next generation engineered T-cell therapies to the routine care of children with solid tumors within a decade.
Catherine Bollard, M.D., M.B.Ch.B., selected to lead global Cancer Grand Challenges team

Cancer Grand Challenges NexTGen team members (left to right): Amy Hont, M.D., AeRang Kim, M.D., Nitin Agrawal, Ph.D., Catherine Bollard, M.D., M.B.Ch.B., Conrad Russell Cruz, M.D., Ph.D., Patrick Hanley, Ph.D., and Anqing Zhang.
A world-class team of researchers co-led by Catherine Bollard, M.D., M.B.Ch.B., director of the Center for Cancer and Immunology Research at Children’s National Hospital, has been selected to receive a $25m Cancer Grand Challenges award to tackle solid tumors in children. Cancer Grand Challenges is a global funding platform, co-founded by Cancer Research UK and the National Cancer Institute in the U.S., that supports a community of diverse, global teams to come together, think differently and take on some of cancer’s toughest challenges.
The Cancer Grand Challenges NexTGen team, co-led by University College London’s Martin Pule, M.D., will be working to develop next-generation cell therapies for children with solid cancers. Cancer is a leading cause of death by disease in children worldwide. Although survival has increased for some pediatric cancers, such as blood cancers, survival for some solid tumors has seen little improvement for more than 30 years. The team hopes to build a much deeper understanding of childhood cancers and develop and optimize novel therapies for children with solid tumors, ultimately hoping to improve survival and diminish the lifelong toxicities often experienced by survivors.
“With our Cancer Grand Challenge, we hope to bring next-generation CAR T-cell therapies to children with solid tumors,” said Dr. Bollard. “What excites me most is the energized, passionate group of people we’ve brought together to take this challenge on. Big problems remain to be addressed, but we believe they can be solved, and that we’re the team to solve them.”
“NexTGen represents crucial and overdue work. It has hope written all over,” said Sara Wakeling, patient advocate on the team and CEO and co-founder of Alice’s Arc, a children’s charity for rhabdomyosarcoma. “NexTGen hopes to transform the way these aggressive solid tumors are treated with less toxic side-effects, giving the children a real chance at growing up and realizing their potential. I’m so proud to be part of this exceptional team of scientists, clinicians and advocates who want to change the story for those diagnosed.”
The NexTGen team unites scientists and clinicians with expertise in immunology, proteomics, mathematics and more, across eight institutions throughout the U.S., U.K. and France. The Children’s National investigators that will also join are:
- Nitin Agrawal, Ph.D., associate professor in the Center for Cancer and Immunology Research at Children’s National.
- Conrad Russell Cruz, M.D., Ph.D.,principal investigator for the Program for Cell Enhancement and Technologies for Immunotherapies at Children’s National.
- Patrick Hanley, Ph.D., chief and director of the cellular therapy program at Children’s National and leader of the Good Manufacturing Practices laboratory.
- Amy Hont, M.D., oncologist in the Center for Cancer and Immunology Research at Children’s National.
- AeRang Kim, M.D., oncologist in The Center for Cancer and Blood Disorders at Children’s National.
- Holly Meany, M.D., oncologist in The Center for Cancer and Blood Disorders at Children’s National.
- Anqing Zhang, biostatistician in the Biostatistics and Study Methodology Department at Children’s National.
The team, co-funded by Cancer Research UK, the National Cancer Institute and The Mark Foundation for Cancer Research, aims to bring much needed new treatments to children with solid cancers.
The NexTGen team is one of four new teams announced today as part of Cancer Grand Challenges, representing a total investment of $100m to diverse, global teams to take on some of the toughest challenges in cancer research.
“Cancer is a global issue that needs to be met with global collaboration. This investment in team science encourages diverse thinking to problems that have long hindered research progress,” said David Scott, Ph.D., director of Cancer Grand Challenges, Cancer Research UK. “Cancer Grand Challenges provides the multidisciplinary teams the time, space and funding to foster innovation and a transformative approach. NexTGen is one of four newly funded teams joining a scientific community addressing unmet clinical needs across cancer research.”
Find out more
Cancer Grand Challenges supports a global community of diverse, world-class research teams with awards of £20m/$25m to come together, think differently and take on cancer’s toughest challenges. These are the obstacles that continue to impede progress and no one scientist, institution or country will be able to solve them alone. Cancer Grand Challenges teams are empowered to rise above the traditional boundaries of geography and discipline.
Founded by the two largest funders of cancer research in the world – Cancer Research UK and the National Cancer Institute* in the U.S. – Cancer Grand Challenges aims to make the progress against cancer we urgently need. Cancer Grand Challenges currently supports more than 700 researchers and advocates across 10 countries, representing 11 teams are supported to take on 10 of the toughest challenges in cancer research.
The Cancer Grand Challenges NexTGen team, announced June 16, 2022, is taking on the initiative’s Solid Tumours in Children challenge. It is led by Dr. Bollard (Children’s National) and Dr. Pule (University College London), along with 23 co-investigators and 7 patient advocates, and is spread across eight institutions across the U.S., U.K. and France: Cardiff University; Children’s Hospital of Philadelphia; Children’s National Hospital; INSERM; the Institute of Cancer Research; Stanford Medicine; Stanford University; University College London. The Cancer Grand Challenges NexTGen team is funded by Cancer Research UK, the National Cancer Institute in the U.S. and The Mark Foundation for Cancer Research.
*The National Cancer Institute is part of the National Institutes of Health.
Developing next-generation T cells to fight cancer

In the last decade, researchers have witnessed significant advances in the immunotherapy field. Most recently, a study in Nature claimed a novel CAR T-cell therapy “cured” a patient.
In the last decade, researchers have witnessed significant advances in the immunotherapy field. Most recently, a study in Nature claimed a novel CAR T-cell therapy “cured” a patient. Given the landmark scientific achievement for patients with different types of leukemia and lymphoma, Children’s National Hospital experts chimed in on the technology they have developed beyond CAR T cells.
Catherine Bollard, M.D., M.B.Ch.B., director of the Center for Cancer and Immunology Research at Children’s National Hospital, discusses the implications of this research, how it relates to the work she’s doing at Children’s National and the future of T-cell therapies.
Q: What did the research published in Nature find?
A: It reported a decade-long experience with this novel T-cell therapy called CD19 CAR T cells. These were used to treat patients with a type of leukemia or lymphoma that expresses the CD19 on its surface. While the article reported the experience of Children’s Hospital of Philadelphia and the University of Pennsylvania, multiple groups throughout the country did similar trials that have used these unique CD19 CAR T cells to treat children and adults with these refractory blood cancers.
Q: What are your thoughts on the implications of this research?
A: We now have three FDA-approved commercial CD19 CAR T-cell products developed by several academic institutions. This is revolutionary for our patients who have B-cell leukemias and lymphomas. It’s incredibly exciting for our T-cell therapy field in general because this was the first time the FDA approved a T-cell therapy. What it means now is the field is extremely excited to develop similar effective therapies for other patients with cancer.
Q: How does this relate to your work at Children’s National?
A: While CAR T cells have made tremendous progress for patients with B-cell leukemias, lymphomas and other blood cancers, the CAR T-cell field has not made the same impact for adult and pediatric solid tumors. We think the field is going to expand the type of T-cell therapies we’re generating beyond just CAR T cells. That’s where the work we’re doing comes in – not only by developing new T cells that don’t need gene engineering but also T cells that can be used as a platform for next-generation engineering approaches. We think the technology we’ve developed at Children’s National will help make an impact, especially in the solid tumor space. I hope in the next 10 years, we’ll be having a conversation not just about CAR T cells, but about other types of T cells that are now making an impact for solid tumors.
Q: How are the CAR T cells you develop different than those in the Nature article?
A: We think our multi-antigen specific T cells are complimentary and could have more potency than conventional CAR T cells for solid tumors especially when used in combination. This is in part because they can identify multiple targets on a tumor cell. Tumor cells are very clever and try to hide from T-cell therapies by down regulating the target that the T cell is directed towards. However, our novel T-cell therapies get around that escape by targeting multiple targets in a single product, making it much harder for the cancer cell to hide from the immune attack by the T cells.
Additionally, we’re excited by our approach because not all of our products require gene engineering, unlike CAR T cells. We have effectively used our T cells to target viruses in the “off-the-shelf” setting and we’re now about to start a first human clinical trial at Children’s National using an off the shelf T-cell product for children with solid tumors. It makes the T-cell therapy more like an “off-the-shelf” drug therapy that will allow us to treat many more children and adults nationally, as well as we hope, internationally.
Manufactured leukemia-specific T cells may help increase survival rates

Infusion of a novel, multi-targeted donor-derived T-cell therapy is safe and well-tolerated in patients with high-risk or relapsed leukemia after a donated bone marrow transplant, according to a new study published in Blood Advances.
Infusion of a novel, multi-targeted donor-derived T-cell therapy is safe and well-tolerated in patients with high-risk or relapsed leukemia after a donated bone marrow transplant, according to a new study published in Blood Advances. The findings suggest that this strategy may make a difference in these patients, as will be evaluated in later phase trials.
“A tumor cell is very clever because it tries to hide from T-cell therapies by deleting or down regulating targets that the T cell is directed towards,” said Catherine Bollard, M.D., M.B.Ch.B., director of the Center for Cancer and Immunology Research at Children’s National Hospital and co-senior author. “This novel cell therapy has the potential to get around that escape by targeting multiple proteins in a single product, making it much harder for the cancer cell to hide from the immune attack by the T cells.”
The tumor-associated antigen-specific T cell (TAA-T) product targets WT1, survivin and PRAME, which are proteins that play a role in cancer cell proliferation and survival. They are overexpressed in leukemia and many other human malignancies. The researchers chose to expand the T cells to target many malignancies through at least one expressed antigen. The manufactured TAA-T products are derived from peripheral blood mononuclear cells (PBMCs) obtained from the patient’s own BMT donor.
The hold-up in the field
Conventional therapies for patients with high-risk or relapsed malignancies often fail due to toxicity associated with additional chemotherapy and second transplant, particularly in those who relapse early after transplant. This novel cellular immunotherapy approach is shown to be safe and targets antigens that are found in CD19 positive and negative blood cancers, which may broaden the applicability to other cancer types, such as acute myeloid leukemia, that are currently lacking effective T cell therapy options.
What’s next
“Evaluation and tracking of unique T cell receptor clonotypes in patients following TAA-T cell infusion demonstrated expansion and persistence of some clonotypes up to 6 months to one-year post-infusion,” said Hannah Kinoshita, M.D., oncology fellow at Children’s National and co-lead author. “In future studies, we are hoping to identify and track unique target antigen-specific clonotypes from the T cell product infused to better understand the immunobiological effect of the infused T cells and how that can be translated into improved clinical outcomes.”
Children’s National Hospital leads the way
The Cell Enhancement and Technologies for Immunotherapy (CETI) program at Children’s National specializes in developing and analyzing novel cellular therapeutics such as this one.
You can read the full study “Outcome of Donor-derived TAA-T cell therapy in Patients with High-risk or Relapsed Acute Leukemia Post Allogeneic BMT,” in Blood Advances. Children’s National researchers worked in partnership with Rick Jones, M.D., co-senior author and Kenneth Cooke, M.D., Ph.D., co-lead author, both at Johns Hopkins Medicine.
Study with largest cohort in the Western world sheds light on Epstein-Barr virus
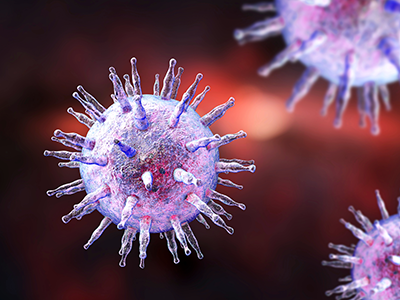
Epstein-Barr virus is a member of the herpes family and it spreads primarily through saliva.
Children’s National Hospital experts provided a contemporary description of the epidemiology, clinical presentation and management of chronic active Epstein-Barr virus (CAEBV), shedding light on this very rare disease. The paper, published in Blood Advances, assessed 57 patients outside of Asia — the biggest international retrospective cohort study published in the Western world.
Epstein-Barr virus is a member of the herpes family and it spreads primarily through saliva. Once a person is infected with Epstein-Barr virus, the immune system will control the infections, but the virus lies in a dormant state in the patient’s B Cells. However, in some patients, there is a failure of the body to control the infection, and the virus is found inside the patient’s T and/or NK cells. These rare patients are diagnosed with CAEBV. The hallmark of the disease is proliferation of Epstein-Barr virus-infected T or NK cells that infiltrate tissues, leading to end-organ damage. Patients most often experience fevers, hepatosplenomegaly, liver inflammation, cytopenias and lymphoproliferation that may progress to lymphoma.
Given it is most prevalent in Asia, little is known about the disease in the Western world. There has only been one published paper regarding the outcomes of patients in the U.S., which included 19 patients amassed over 28 years, and was published a decade ago.
Multiple treatments have been attempted to control the disease, but none have resulted in consistent remission. Historically, the consensus is to use steroids and/or antiviral drug in combination with proteasome inhibitor agents. In some cases, clinicians also use cytotoxic chemotherapy to reduce disease burden and improve the patient’s condition before HSCT. Still, this approach is limited because most patients die due to the progression of their disease despite these interventions.
Ultimately, most of these patients are referred for allogeneic hematopoietic stem cell transplantation (HSCT), which is the only known curative therapy for CAEBV. However, the best approach to control disease prior to HSCT, as well as the optimal conditioning regimen, are unknown.
“For the first time in many years, we provide insight on contemporary treatment options to consider for patients with CAEBV, as well as identifying risk factors for worse outcomes,” said Blachy Dávila Saldaña, M.D., blood and marrow transplant specialist at Children’s National and lead author of the study. “HSCT is curative, but patients need to be considered prior to the evolution of more advanced disease, particularly lymphoma. We also provide a new platform that will inform research on new interventions and therapies for this population.”
“CAEBV remains a challenging disorder to treat, especially once severe complications develop,” said Catherine Bollard, M.D., M.B.Ch.B., director of the Center for Cancer and Immunology Research at Children’s National. “However, our data suggests that T cell modulating therapies may enhance disease control, and future studies should address this question in a controlled setting.”
Future steps also include performing genetic studies to identify those at risk of developing the disease, and developing new platforms for treatment, including checkpoint inhibitors and cytotoxic lymphocyte therapies (CTL’s), which is a form of adoptive immunotherapy that employs virus-specific T cells.
The cohort includes patients treated in CNH and multiple institutions around the world, including Texas Children’s and the National Institutes of Health. “This work was only possible through our collaborative research in anti-EBV cellular therapies,” said Dr. Dávila.