Q&A with Dr. Rokita: Building bioinformatics infrastructure at the Brain Tumor Institute

Jo Lynne Rokita, PhD, is the director of the new Bioinformatics Core housed within the Brain Tumor Institute at Children’s National Hospital.
Jo Lynne Rokita, PhD, is the director of the new Bioinformatics Core housed within the Brain Tumor Institute at Children’s National Hospital. Dr. Rokita is a cancer genomics leader with 20 years of combined research experience in academia, industry and the government. She’s also a technical and analytical expert in genomics research using microarrays and high-throughput sequencing.
“We are very excited that we were able to recruit Dr. Rokita as director of the Bioinformatics Core Facility,” says Muller Fabbri, MD, PhD, associate center director for Cancer and Immunology Research at Children’s National. “Her Bioinformatics Core will play a central role in providing the Brain Tumor Institute community with unique expertise spanning biology/genetics/genomics and bioinformatics and will propel Children’s National forward as a national and worldwide leader in pediatric brain tumor research.”
Dr. Rokita is overseeing the core’s creation, including bringing both bioinformatics staff and computing infrastructure to the program, which will support the data analysis needs of the institute’s investigators. She recently answered questions about the new core and also talked a little bit about the focus of her own research that will continue at Children’s National.
Q: Why is the Brain Tumor Institute establishing a Bioinformatics Core?
A: Growing the institute’s bioinformatics capabilities was one of the things that leadership wanted to make sure was built into the plan for the record-setting $96 million gift that was received in 2023. There was a clear need among the principal investigators for this type of research support which includes organization, analysis and interpretation of large-scale genetic sequencing and other “-omics” data.
Q: How did you decide to join Children’s National?
A: I was leading a pediatric brain tumor focused bioinformatics team at Children’s Hospital of Philadelphia (CHOP). As a part of the Children’s Brain Tumor Network (CBTN), I worked closely with a collaborator from Children’s National, Brian Rood, MD, medical director of the Brain Tumor Institute. He told me about the opportunity and I was very excited to apply.
Q: How did your previous work prepare you for this role?
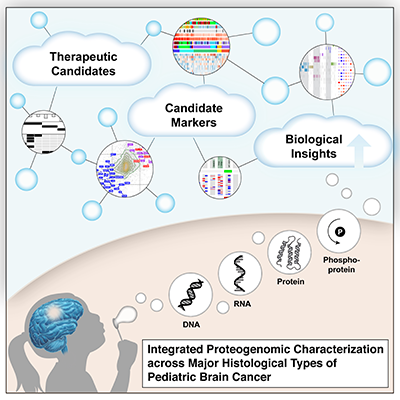
A: I’ve spent the past 10 years in the pediatric cancer field with the last six focused on brain tumor research. In my various roles at CHOP, I led multiple large-scale genomic analysis efforts, comprehensive data and methods for which we then provided openly to the community. During my postdoctoral fellowship, these efforts included a large neuroblastoma patient-derived cell line “ENCODE” as well as a resource led in collaboration with multiple institutes and the National Cancer Institute funded by Alex’s Lemonade Stand Foundation (ALSF). We further scaled these efforts to build open analytical platforms to empower researchers to build upon our work doing their own cancer genomic analysis. In collaboration with the Childhood Cancer Data Lab at ALSF, we built the platform that ultimately ballooned into the OpenPedCan includes large amounts of harmonized genomic, epigenomic and proteomic data for patients with pediatric cancer. What’s unique is that the data is all processed in the same way and easily accessible through multiple mechanisms. Researchers can use these data to ask questions about the cancer type they study or genes of interest. For example, genes over-expressed, absent and/or mutated in a specific tumor subtype may lead to a better understanding of how a patient’s cancer may respond to a treatment.
We’ll be bringing some of the workflows we created previously here to Children’s National, and that will allow us to join newly generated internal data with the thousands of data points we’ve already harmonized using these workflows.
Q: Can you give us some examples of how data harmonization benefits the field of pediatric brain tumor research?
A: Harmonizing across institutions and databases will help us increase the number of data points available for study. This is really important for rare types of tumors and are major foci of institute collaborator Adriana Fonseca, MD, and her International Rare Brain Tumor Registry program. The Bioinformatics Core will support data organization and analysis for this effort, which aims to sequence the rarest brain tumors — those that make up between only 3% and 5% of all brain tumors. If all the data is analyzed the same way, we can combine multiple studies to increase our total dataset, which in turn may reveal new biomarkers and new subtypes of those tumors. It is critical that we continue to build these data resources in a way that they can be accessed by everyone doing this work. Having dedicated support systems for these functions will push the research farther, faster.
Q: As this work gets underway, what is the core’s main function?
A: As this initiative gets underway, the Bioinformatics Core’s primary goal is to empower investigators by streamlining and centralizing data analyses. We help researchers transfer sequencing data into secure cloud storage, organize newly generated records and prepare those datasets for in-depth study. Our bioinformatics scientists then perform downstream analyses to address the specific questions posed by each investigator. On the backend, we collaborate with information technology at Children’s National to develop a robust infrastructure that supports these activities efficiently. By offering these services in-house, we aim to ensure our investigators have seamless, comprehensive support—ultimately driving innovation and accelerating research progress.
Q: What is “open science” and why is it important in bioinformatics?
A: One of our big focus areas is open science, meaning our goal is to push data and code out into the community so that researchers can easily reproduce and build upon our findings. I’m excited to bring the principles of open science, code sharing and data sharing to the Bioinformatics Core.
Making resources open makes it easier for teams to work together across institutions and research programs. It is also going to benefit patients because people can reuse the code and move towards cures faster. For example, we try to package an entire manuscript’s code when we provide our data so it’s clear how the analyses were done.
Q: What is your particular research passion?
A: I work in several research areas and with many brilliant collaborators. One of our focus areas is understanding how RNA splicing can contribute to pediatric brain tumors to create a change in a protein. We have recently identified tumor-specific splice events in some pediatric brain tumor types and will be partnering with Dalia Haydar, PharmD, PhD, to create therapeutic approaches to targeting these. We are also developing a user-friendly application for mining the large amount of splicing data in pediatric brain tumors.
Another focus of our lab is understanding how the patient’s host genome (alterations inherent in their blood DNA) influences the tumor’s genetics. For example, we’ve just preprinted a study connecting inherited variants to tumor genetics and patient outcomes.
Finally, we are interested in how differences in race, ethnicity and social determinants of health influence survival and treatment outcomes for children with brain tumors.
I am passionate about data sharing, code reproducibility and promoting open science in general.
Q: Is there any specific reason you decided to focus your work around brain tumors and pediatric brain tumors?
A: My cousin passed away from a brain tumor when I was in high school. They didn’t have molecular diagnosis then, but he had a brainstem glioma, likely a diffuse midline glioma. In graduate school, I studied addiction genetics and became fascinated with the brain and towards the end, cancer. As an alumna of Penn State, I was actively involved in philanthropic events raising money for their Dance MaraTHON supporting children with cancer. I was lucky to land a postdoc at CHOP and lean into subsequent roles which allowed my passion for this field to grow.
Q: Last question — What do you do with your time when you are not studying pediatric brain tumor data?
A: I enjoy being with my family, observing my children learn and grow, and listening to music.



 Children’s National Hospital announced a $96 million investment from an anonymous donor family to transform rare childhood brain tumor research and care. The donation, which strengthens our globally recognized leadership in the field, is one of the largest in the hospital’s history.
Children’s National Hospital announced a $96 million investment from an anonymous donor family to transform rare childhood brain tumor research and care. The donation, which strengthens our globally recognized leadership in the field, is one of the largest in the hospital’s history.