New prediction rules aim to improve care for febrile infants
When a baby younger than 3 months of age develops a fever, parents and pediatricians face serious challenges. While many fevers are harmless, some can signal invasive bacterial infections (IBIs) such as bacteremia or bacterial meningitis. For decades, the safest approach has been to test aggressively and hospitalize many of these infants while waiting for results. This can mean spinal taps, blood cultures, antibiotics and nights in the hospital — even when the infection risk is low.
For infants 61 to 90 days old, the guidance has been especially unclear. These babies fall just outside the age group covered by the American Academy of Pediatrics’ (AAP) current guidelines, leaving clinicians without evidence-based rules to support their decisions. A new multicenter study led by the Pediatric Emergency Care Applied Research Network (PECARN), with Nathan Kuppermann, MD, MPH, of Children’s National Hospital as senior author, is beginning to fill that gap.
Why this matters
IBIs occur in about 1–2% of febrile infants aged 61–90 days. Because there hasn’t been a reliable way to determine which infants are at higher or lower risk, emergency departments often take a one-size-fits-all approach. That can lead to unnecessary testing, antibiotic exposure and hospitalization for many families, even though most infants with fevers do not have serious bacterial infections.
Developing a safe, validated way to identify low-risk infants has the potential to reduce this burden while maintaining patient safety.
Inside the study
Researchers analyzed data from nearly 5,000 febrile infants ages 61–90 days who were evaluated across 17 PECARN emergency departments between 2012 and 2024. They looked at common variables such as urinalysis results, temperature, procalcitonin (PCT, a blood marker of inflammation) and absolute neutrophil count (ANC, a measure of immune response).
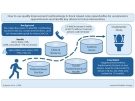
From this large dataset, the team created and internally validated two new prediction rules:
- Without obtaining blood: Infants with negative urinalysis and a maximum temperature of 38.9°C (102°F) or lower were at low risk for IBI.
- With obtaining blood: Infants with PCT ≤ 0.24 ng/mL and ANC ≤ 10,710 cells/mm³ were at low risk for IBI.
Both rules showed high accuracy, with negative predictive values above 99%. Notably, the PCT-based rule did not misclassify any infants with an IBI in the study sample.
What this means for families
If confirmed in prospective studies, these prediction rules could transform how pediatricians approach fevers in infants 61-90 days old. Instead of defaulting to hospitalization and antibiotics, clinicians may one day safely identify which infants can be managed with close follow-up at home. That could reduce stress for families, free up hospital resources and allow providers to target intensive care to the children who need it most.
For parents, this research offers hope that in the future, a fever in a 2- or 3-month-old won’t always mean a trip to the hospital and days of uncertainty. Instead, care could become more personalized, evidence-based and less invasive.
The road ahead
While the results are promising, these prediction rules are not ready for clinical practice just yet. The next step is external validation: testing the rules prospectively in diverse emergency departments, including community hospitals. Only then will pediatricians know whether these tools can be safely applied in real-world settings.
Read the full study, “Prediction Rule to Identify Febrile Infants 61-90 Day at Low Risk for Invasive Bacterial Infections” in the American Academy of Pediatrics.