A look at the Children’s National Spina Bifida Program
The Spina Bifida Program at Children’s National Hospital, led by co-directors, Christina Ho, M.D., and Briony Varda, M.D., has seen impressive growth and there are plans to continue expanding the program. Drs. Ho and Varda share insights on the multidisciplinary care being provided, along with their plans for the future of the program.
Q: How would you describe the growth of the program?
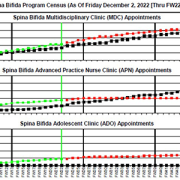
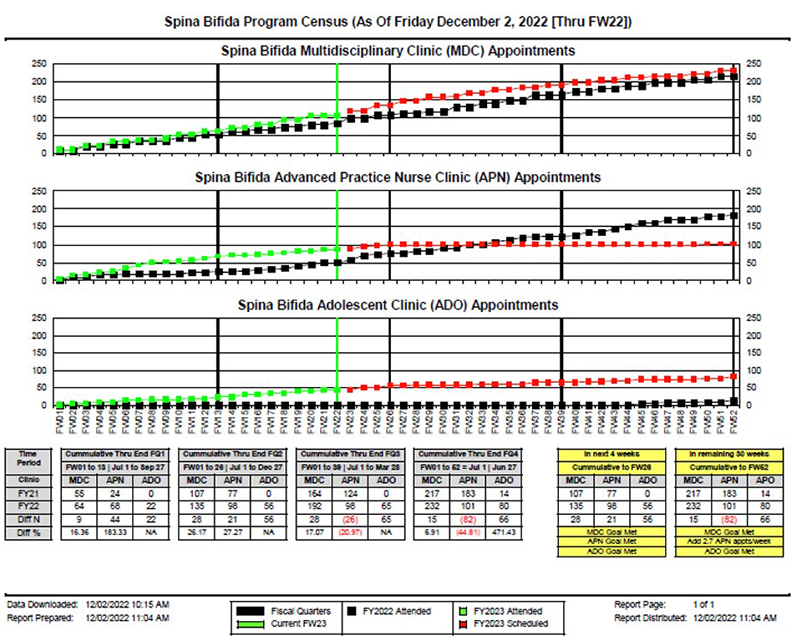
A: The growth of the Spina Bifida Program has been remarkable! The graph below really shows it all (more than a 25% increase in patient visits in the past year). We currently hold multidisciplinary programs including providers from neurosurgery (Robert Keating, M.D.), orthopaedic surgery (Matthew Oetgen, M.D.), physical medicine and rehabilitation (Mi Ran Shin, M.D.), urology (Briony Varda, M.D. and Christina Ho, M.D.), and expanded to include bowel management (Celicia Little, N.P.), gynecology (Allison Mayhew, M.D.) for our adolescent patients, as well as a dedicated nurse, Nicole Allentuck, R.N., and program associate, Christine Scott.
We are extremely proud of how the program has grown, particularly through the past two years, with the advent of our adolescent clinic and having a dedicated supportive team that ensures we have significant re-engagement of patients who had previously been lost to care. We are also working with the Prenatal Pediatrics Institute at Children’s National to enhance our prenatal care for patients diagnosed with spina bifida.
Q: What advancements is the spina bifida program making that benefit patients?
A: We have developed a transition clinic for our adolescent spina bifida patients to help address goals of care, independence with care and readiness for transition to adult providers. Our program coordinator, Celicia Little, N.P., also oversees our bowel management program to provide specialized bowel management care for our patients. We have been working on educational information specific to different areas within spina bifida, including how to catheterize, common medications, bowel management and anticipatory guidance. This helps to provide longevity for our patients as well. We are evaluating ways to decrease visits to the emergency department and ensure appropriate antibiotic usage with proper diagnoses of urinary infections in patients who perform CIC. To further our goal of providing longitudinal care within our program, we have engaged gynecology colleagues to see patients within our adolescent clinic and begin promoting independence through perpetuated discussions (e.g., are they able to schedule their own physician appointments or grocery shop for themselves?) in preparation for adult transitional care. Additionally, we readily offer telehealth visits for convenience and in hopes of easing access to care.
Q: Looking ahead, what’s next for the Spina Bifida Program? How will we continue to measure success?
A: We are excited to continue expanding our Spina Bifida Program. We currently care for more than 500 patients within the Washington, D.C., Maryland and Virginia areas. We want to continue to include patient narratives through our research initiatives to inform quality of care, including decreasing E.D. utilization and needless antibiotic use. We also want to expand our adolescent program to include sexual healthcare as they transition to adult care with our adult collaborators within MedStar and GWU. We would like to provide more comprehensive care, improve access to care, and ensure patients and families have utilization of the armamentaria of medical resources available at Children’s National.