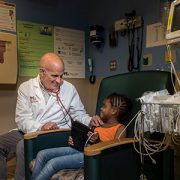Making the case for a comprehensive national registry for pediatric CKD

“It’s of utmost importance that we develop more sensitive ways to identify children who are at heightened risk for developing CKD.,” says Marva Moxey-Mims, M.D. “A growing body of evidence suggests that this includes children treated in pediatric intensive care units who sustained acute kidney injury, infants born preterm and low birth weight, and obese children.”
Even though chronic kidney disease (CKD) is a global epidemic that imperils cardiovascular health, impairs quality of life and heightens mortality, very little is known about how CKD uniquely impacts children and how kids may be spared from its more devastating effects.
That makes a study published in the November 2018 issue of the American Journal of Kidney Diseases all the more notable because it represents the largest population-based study of CKD prevalence in a nationally representative cohort of adolescents aged 12 to 18, Sun-Young Ahn, M.D., and Marva Moxey-Mims, M.D., of Children’s National Health System, write in a companion editorial published online Oct. 18, 2018.
In their invited commentary, “Chronic kidney disease in children: the importance of a national epidemiological study,” Drs. Ahn and Moxey-Mims point out that pediatric CKD can contribute to growth failure, developmental and neurocognitive defects and impaired cardiovascular health.
“Children who require renal-replacement therapy suffer mortality rates that are 30 times higher than children who don’t have end-stage renal disease,” adds Dr. Moxey-Mims, chief of the Division of Nephrology at Children’s National. “It’s of utmost importance that we develop more sensitive ways to identify children who are at heightened risk for developing CKD. A growing body of evidence suggests that this includes children treated in pediatric intensive care units who sustained acute kidney injury, infants born preterm and low birth weight, and obese children.”
At its early stages, pediatric CKD usually has few symptoms, and clinicians around the world lack validated biomarkers to spot the disease early, before it may become irreversible.
While national mass urine screening programs in Japan, Taiwan and Korea have demonstrated success in early detection of CKD, which enabled successful interventions, such an approach is not cost-effective for the U.S., Drs. Ahn and Moxey-Mims write.
According to the Centers for Disease Control and Prevention, 1 in 10 U.S. infants in 2016 was born preterm, prior to 37 weeks gestation. Because of that trend, the commentators advocate for “a concerted national effort” to track preterm and low birth weight newborns. (These infants are presumed to have lower nephron endowment, which increases their risk for developing end-stage kidney disease.)
“We need a comprehensive, national registry just for pediatric CKD, a database that represents the entire U.S. population that we could query to glean new insights about what improves kids’ lifespan and quality of life. With a large database of anonymized pediatric patient records we could, for example, assess the effectiveness of specific therapeutic interventions, such as angiotensin-converting enzyme inhibitors, in improving care and slowing CKD progression in kids,” Dr. Moxey-Mims adds.