Children’s National uses HIFU to perform first ever non-invasive brain tumor procedure

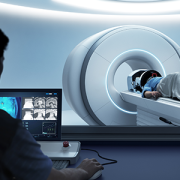
Children’s National Hospital successfully performed the first-ever high-intensity focused ultrasound (HIFU) procedure on a pediatric patient with neurofibromatosis (NF). This is the youngest patient to undergo HIFU treatment in the world. Image provided by Insightec.
Children’s National Hospital successfully performed the first-ever high-intensity focused ultrasound (HIFU) procedure on a pediatric patient with neurofibromatosis (NF). This is the youngest patient to undergo HIFU treatment in the world. The advancement of children’s medical devices in the U.S. continues to significantly lag behind adult devices. This is why this milestone marks a significant advance in making pediatric surgery more precise and less invasive.
The hospital is offering this treatment to patients under an ongoing research clinical trial. Children’s National is one of the first pediatric hospitals in the nation to use HIFU for neuro-oncology patients. It’s also the first hospital in the world to use it to treat a pediatric patient with NF. NF is a condition that occurs in approximately 1 in 3,500 births and causes tumors to form in the brain, spinal cord and nerves.
“Using HIFU to treat our pediatric patients is a quantum leap towards non-invasive surgery for kids,” said Robert Keating, M.D., division chief of Neurosurgery and co-director of the HIFU program at Children’s National. “It’s exciting because the future is now here and it’s significantly better for our kids, in terms of non-invasive surgery with lower risk of complications and no exposure to radiation.”
Focused ultrasound (FUS) is a non-invasive therapeutic technology with the potential to transform the treatment of many medical disorders by using ultrasonic thermal energy to specifically target tissue deep in the body. The technology can treat without incisions or the need of radiation.
FUS, which has been used for adult clinical trials for many decades, can be delivered through high- or low-intensity focused ultrasound (LIFU). HIFU uses non-invasive therapy that uses focused ultrasound waves to thermally ablate a focal area of tissue. Children’s National will now use HIFU to treat low-grade type tumors located in difficult locations of the brain, such as hypothalamic hamartomas and pilocytic astrocytoma, as well as for movement disorders and epilepsy.
An alternative approach, LIFU uses lower levels of energy to disrupt the blood-brain barrier. Unlike medications, which often have difficulty crossing the blood-brain barrier, LIFU can transiently open the blood-brain barrier to chemotherapy. This may allow more effective treatment of tumors and offer opportunities to treat, for the first time, the entire extent of a malignant brain tumor.
“Having focused ultrasound technology as a tool and conducting clinical trials will allow our neurologists and oncologists to offer a non-invasive treatment option to many patients who suffer from neurological conditions,” said Hasan Syed, M.D., co-director of the HIFU program at Children’s National. “The milestone of performing this first HIFU procedure will lead the way to better understanding of the effect of this technology and provide patients with more options.”
At Children’s National, the HIFU program is being led by Dr. Keating and a multidisciplinary team, including clinicians and investigators from the Sheik Zayed Institute for Pediatric Innovation, radiology, oncology, surgery and orthopedics. In an effort to collaborate with the region’s adult hospitals, Children’s National will also treat adult patients on a selective basis who have movement disorders such as essential tremor and Parkinson’s. There is a scarcity of similar resources in the metro region. Many adult patients face one-year wait periods for treatment of their movement disorders, requiring many to travel out of state for treatment.
The LIFU program is scheduled to be operational in 2022. It will likely be the first in the U.S. to treat high-grade pediatric brain tumors with disruption of the blood-brain barrier and provide more effective routes for chemotherapy as well as potential immunotherapy and molecular approaches.
“The use of LIFU with microbubbles to open up the blood-brain barrier is an exciting, potentially game-changing approach for children with these tumors,” said Roger Packer, M.D., senior vice president of the Center for Neurosciences and Behavioral Medicine at Children’s National. “It should safely allow the blood-brain barrier to open and allow delivery of potentially life-saving personalized therapy to the tumor and spare the rest of the brain. It is the most exciting, new development in brain tumor therapy for these malignant midline tumors in the past 50 years.”
Children’s National continues to be a leader in pediatric HIFU use. In 2015, Children’s National doctors became the first in the U.S. to use MR-HIFU to treat pediatric osteoid osteoma – a benign, but painful bone tumor. Successful clinical trial results led to FDA approval in early 2021 for the use of the technology for this treatment. In 2020, the Focused Ultrasound Foundation also designated Children’s National as the first global pediatric Center of Excellence for using this technology to help patients with specific types of childhood tumors.