Working miracles to control seizures and preserve brain power in newborns
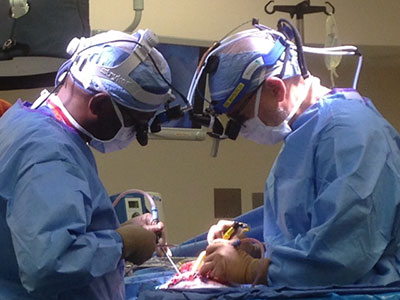
In the spring of 2017, a multidisciplinary team applied an innovative approach to help preserve function in the working right hemisphere of a baby who experienced her first seizure hours after birth.
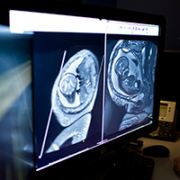
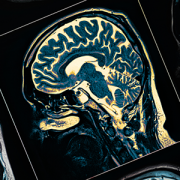
When orderly early fetal brain development is disturbed in one half of the brain, infants can be born with hemimegalencephaly—a rare occurrence—that results in one of the brain’s two hemispheres being oversized, heavy and malformed. This brain malformation arises early in the fetal period of life, is not inherited and is associated with seizures early in life.
Children with hemimegalencephaly can develop horrible seizures within the first hours or days of life. According to published research, every month these infants experience uncontrolled seizures correlates to a steep decline in IQ.
Because these types of seizures do not respond to multiple anti-seizure medications—medicines which may also cause worrisome side effects of their own in neonates—care teams attempt to schedule surgery as soon as feasible to remove or disconnect the hemisphere triggering the damaging seizures. “The ‘bad’ brain does not sustain any function and it interferes with the ‘good’ brain doing what it needs to do,” says William D. Gaillard, M.D., chief of Children’s division of Epilepsy and Neurophysiology and chief of Neurology.
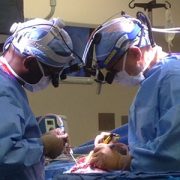
Hemispherectomy is intricate surgery on an organ that is softer than normal and crisscrossed with a tangle of blood vessels that supply the damaged hemisphere with blood. Because of the risks of life-threatening blood loss in very young infants, the dramatic surgery is usually not performed until babies are at least 3 months old and weigh at least 10 pounds.
The challenge: The vulnerable babies who most need relief, infants who have been seizing since early life, are too young for the operation.
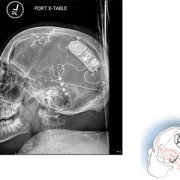
Neurosurgeons have clamped the carotid artery that supplies blood to the brain to minimize blood loss when the hemisphere is surgically removed. Dr. Gaillard says knowledge of that approach led the team to think: What if we use embolization—blocking blood supply to targeted locations in the brain—to achieve the same effect? The plan effectively destroys the malformed brain from within, neutralizing its ability to cause the seizures.
“It was eye-opening for us to think about actually inflicting brain injury as a way of treating something in the brain that was causing seizures. That is really novel in itself: We’re thinking out of the box in applying existing techniques in a different age group. The conventional thinking with newborns is to let them be; their seizures don’t look that bad,” says Taeun Chang, M.D., director of Children’s Neonatal Neurology and Neonatal Neurocritical Care Program.
“We have evidence to suggest this is a safe and effective way of avoiding recurrent seizures and minimizing the need to give these infants potentially toxic medications so early in life. Ultimately, this helps a select group of babies who need the surgery to get to the point of being old enough to have it—all the while, sparing the healthy part of their brain,” Dr. Gaillard adds.

Once the embolization ended Darcy’s most severe seizures, the little girl could make eye contact, started smiling, and then graduated from smiling to full laughs. In weekly physical therapy, the infant works on tummy time, head control and ensuring her eyes track.
In the spring of 2017, the multidisciplinary team applied the innovative approach to help preserve function in the working right hemisphere of a baby named Darcy Murphy. Darcy experienced her first seizure hours after she was born, and when she arrived at Children’s National had been in and out of two different emergency rooms in another state for the first few weeks of her life.
The team explained to the Murphy family that Darcy was on multiple medications, but her seizures continued unabated. The options included inducing a coma, sending Darcy home despite ongoing seizures or minimally invasive embolization.
“We would not have even posed this if we were not confident in our ability to do the procedure and deal with potential complications,” Dr. Chang says.
“Oh my gosh, as a parent you know what you’re doing is permanent,” says Rachel Murphy, 29, Darcy’s mom said of the decisions that she and husband Ryan, 33, faced for the youngest of their three children. “What if it’s not the right decision? What if in a week they come out with a new procedure you could have done? We were horrified all the time. The nice part with this procedure is the reward is apparent very quickly, and it just gets better. You don’t have to wait two years to know you made the right decision. You can see half a brain is better than the whole thing for this specific child.”
Once the embolization ended Darcy’s most severe seizures, the little girl could initiate and maintain eye contact with family members, started smiling and then graduated from smiling to full laughs. In weekly physical therapy, the infant works on tummy time, head control and ensuring her eyes track.
Children’s multidisciplinary care team includes experts in newborn intensive care (neonatologists) to aggressively manage seizures in the traditional fashion as they occur and to monitor vital signs; a neonatal neurologist/neurointensivist at the bedside and in the Angio suite monitoring Darcy’s brain activity; a neonatal epileptologist; a surgical epilepsy team; an interventional neuroradiologist; neurosurgeons to perform the delicate functional hemispherectomy to remove any residual brain tissue from the bad hemisphere; and physical therapists working to help Darcy achieve maximum function after surgery.
“We were just like one unit in the sense of being able to provide coherent, comprehensive care. It’s about blood pressure management, breathing, electrolytes, making sure everything is right for going to the operating room,” Dr. Chang explains. “Darcy’s case highlights the ways in which Children’s National is different and offers personalized care that is superior to other centers.”
The team, which recently published a case report of two previous serial embolizations followed by hemispherectomy, plans follow-up papers describing EEG manifestations during an acute stroke in a newborn, advice to the field on best practices for the embolization and using cooling to control the planned brain injury during embolization hemispherectomy.
Revised Nov. 7, 2017