What’s Known
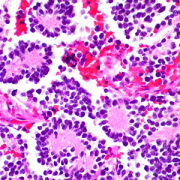
Following treatment, patients with leukemia, lymphoma, and other cancers may receive a transplant in order to restore their body’s natural ability to fight infection and, sometimes, such transplants are a component of leukemia treatment. (Leukemia is the second most common blood cancer, after lymphoma, and its incidence rate has increased by 0.2 percent annually from 2002 to 2011.) A stem cell or cord blood transplant restores the body’s ability to produce infection-fighting white blood cells. After such transplants, however, patients can face heightened risk of developing a life-threatening infection with such viruses as adenovirus, cytomegalovirus, or Epstein-Barr virus.
What’s New
A head-to-head comparison of two strategies to thwart such viral infections shows that both approaches leverage the power of multivirus-specific, donor-derived T-cells (mCTL), which are highly skilled at recognizing foreign invaders. The research team, made up of nine scientists and clinicians affiliated with Children’s National Health System, grew personalized T-cells from peripheral blood (PB) of adult donors who were seropositive for CMV and also coaxed T-cells to grow from naïve cord blood (CB). PB-derived cells have long memories of past battles; naïve CB-derived cells need additional training to acquire such skills. From 35 to 384 days after their stem cell or cord blood transplant, 13 patients were infused with PB mCTL and 12 patients were infused with CB mCTL. Within four weeks, patients experienced up to a 160-fold increase in virus-specific T-cells, which coincided with their response to therapy. Overall response rate was 81 percent.
Questions for Future Research
Q: Could T-cells be personalized to attack other viruses that infect patients post-transplant, such as human parainfluenza virus and BK polyomavirus, providing the potential to target five viruses in a single infusion?
Q: Could the proteins that are used to train T-cells to attack certain viruses also be used to create a personalized approach to tumor suppression?
Source: “A Phase 1 Perspective: Multivirus-Specific T Cells From Both Cord Blood and Bone Marrow Transplant Donors.” Hanley, P., M. D. Keller, M. Martin Manso, C. Martinez, K. Leung, C.R. Cruz, C. Barese, S. McCormack, M. Luo, R.A. Krance, D. Jacobsohn, C. Rooney, H. Heslop, E.J. Shpall, and C. Bollard. Presented during the International Society for Cellular Therapy 2016 Annual Meeting, Singapore. May 26, 2016.