Sirtuin could repair common neonatal brain injury
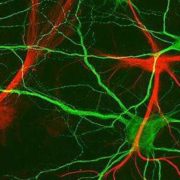
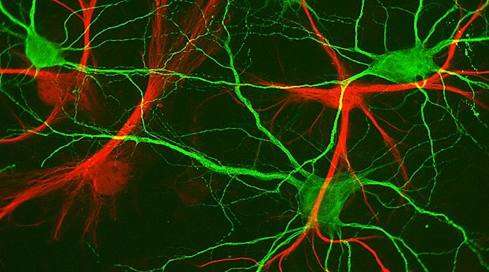
 A team of researchers investigated the molecular mechanisms behind oligodendrocyte progenitor cell proliferation in neonatal hypoxia. What’s knownHypoxia, or a lack of oxygen, is a major cause of diffuse white matter injury (DWMI). This condition leads to permanent developmental disabilities in prematurely born infants. The long-term abnormalities of the brain’s white matter that characterize DWMI are caused by the loss of a specific type of cells known as oligodendrocytes, which support nerve cells and produce myelin, a lipid and protein sheath that electrically insulates nerve cells. Oligodendrocytes are produced by a population of immature cells known as oligodendrocyte progenitor cells (OPCs). Previous research has shown that hypoxia can trigger OPCs to proliferate and presumably produce new oligodendrocytes. The molecular pathways that hypoxia triggers to make new OPCs remain unclear. What’s newA team of researchers led by Vittorio Gallo, Ph.D., director of the Center for Neuroscience Research and the Intellectual and Developmental Disabilities Research Center at Children’s National Health System, investigated the molecular mechanisms behind what prompts OPCs to proliferate in a preclinical model of neonatal hypoxia. The researchers found that a molecule known as Sirt1 acts as a major regulator of OPC proliferation and regeneration. Sirt1 is a sirtuin, a class of molecules that has attracted interest over the past several years for its role in stem cells, aging and inflammation. Hypoxia appears to induce Sirt1 formation. When the researchers prevented brain tissues in petri dishes from making Sirt1 or removed this molecule in preclinical models, these actions prevented OPC proliferation. What’s more, preventing Sirt1 production also inhibited OPCs from making oligodendrocytes. These findings suggest that Sirt1 is essential for replacing oligodendrocytes to repair DWMI after hypoxia. Additionally, finding ways to enhance Sirt1 activity eventually could provide a novel way to help infants recover after hypoxia and prevent DWMI. Questions for future researchQ: How can Sirt1 activity be enhanced in preclinical models and humans? Source: “Sirt1 regulates glial progenitor proliferation and regeneration in white matter after neonatal brain injury.” Jablonska, M., M. Gierdalski, L. Chew, T. Hawley, M. Catron, A. Lichauco, J. Cabrera-Luque, T. Yuen, D. Rowitch and V. Gallo. Published by Nature Communications on Dec. 19, 2016. |