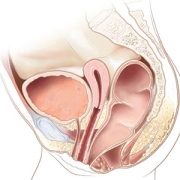
Patient-reported outcomes for children with anorectal malformation
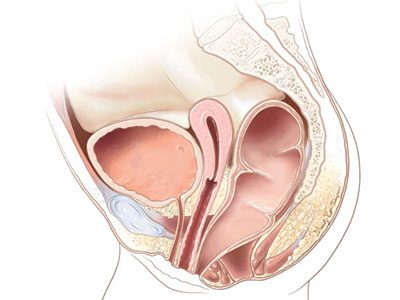
Before this study, little has been documented about how anorectal malformation type, sacral ratio, age and bowel regimen affect continence and quality of life.
A large, multi-institutional study including patient-reported outcomes for children who have anorectal malformations found that the type of malformation and whether a child is clean/continent and not soiling can have a significant impact on the assessment of a patient’s quality-of-life. The study also highlights that patients and their families seem to benefit from access to a specialized center offering multi-disciplinary care in a single location.
What it means
The study is one of the first to collect input from patients and their families at two multi-disciplinary centers for colorectal care. The authors, including Marc Levitt, MD, chief of Colorectal and Pelvic Reconstruction at Children’s National Hospital, who collaborated with colleagues at Nationwide Children’s Hospital in Columbus and Royal Children’s Hospital in Melbourne Australia, sought to understand the impact of the anorectal malformation type and the development of the sacrum bone on continence outcomes in children. Additionally, the team aimed to compare continence outcomes by age group and determine the quality of life with different bowel regimens, including medications like laxatives or the use of enemas.
The researchers found that continence in patients taking laxatives to manage their bowels varied depending on the type of malformation, but that sacral ratio or a measure of the growth of a key pelvic bone correlating with pelvic floor development, did not seem to play a role in continence.
Additionally, patients (and patient families) had similar perceptions of their overall quality of life, as long as the child was clean/continent. Quality-of-life scores were lower, however, if a child was managed using enemas but continued to experience soiling/incontinence. This vital component was a measure of patient reported outcomes, or how the patient perceives their care is going.
Why it matters
Before this study, little has been documented about how anorectal malformation type, sacral ratio, age and bowel regimen affect continence and quality of life. For the first time, these reports are coming from the patient and family point of view. In their conclusion, the authors note that the study’s findings provide important discussion points for counseling patients on long term management strategies for children with anorectal malformations. The findings also identify new areas for research driven by what patients and their families report are most important.
Read the full study, Patient-reported outcomes of Children with an Anorectal Malformation in the Annals of Surgery.