Coming together as a team for the good of the baby

Children’s National has a new program to care for children who have severe bronchopulmonary dysplasia, a serious complication of preterm birth.
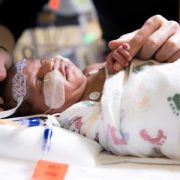
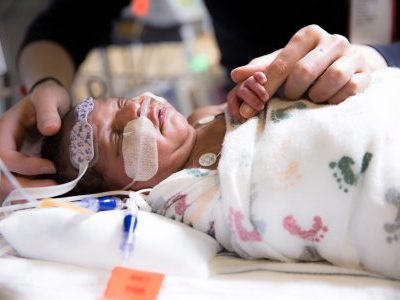
Around the 1-year-old’s crib is a tight circle of smiling adults, and at the foot of his bed is a menagerie of plush animals, each a different color and texture and shape to spark his curiosity and sharpen his intellect.
Gone are the days a newborn with extremely complex medical needs like Elijah would transfer from the neonatal intensive care unit (NICU) to the pediatric intensive care unit and transition through a couple of other hospital units by the time he was discharged. Gone are the days when he’d see a variety of new physician faces at every stop. And gone are the days he’d be confined to his room, divorced from the sights and sounds and scents of the outside world, stimulation that helps little baby’s neural networks grow stronger.
Children’s National has a new program designed to meet the unique needs of children like Elijah who have severe bronchopulmonary dysplasia (BPD), a common complication of preterm birth.
“It’s more forward-thinking – and I mean thinking for the future of each individual baby, and it’s allowing the baby to have one team and one location to take advantage of a deep knowledge of and relationship with that baby and family,” says Robin Steinhorn, M.D. Dr. Steinhorn is senior vice president of the Center for Hospital-Based Specialties and one of Children’s multidisciplinary team members who visited Elijah’s bed twice weekly during his lengthy hospitalization and who continues to see him regularly during outpatient visits.
“The pulmonologist, the neonatologist, the respiratory therapist, the physical therapist, the dietitian, the cardiologist – we all come as a team to work together for the good of the baby,” Dr. Steinhorn adds. “We stick with these babies through thick and thin. We will stick with that baby with this team and this location until they are ready to go home – and beyond.”
BPD, a serious lung condition, mostly affects extremely low birthweight preterm babies whose lungs were designed to continue developing inside the womb until the pregnancy reaches full term. Often born months before their due dates, these extremely vulnerable newborns have immature organs, including the lungs, which are not ready for the task of breathing air. Children’s program targets infants who experience respiratory failure from BPD. The respiratory support required for these infants ranges from oxygen delivered through a nasal cannula to mechanical ventilators.

“It’s more forward-thinking – and I mean thinking for the future of each individual baby, and it’s allowing the baby to have one team and one location to take advantage of a deep knowledge of and relationship with that baby and family,” says Robin Steinhorn, M.D.
About 1 percent of all preterm births are extremely low birthweight, or less than 1,500 grams. Within that group, up to 40 percent will develop BPD. While they represent a small percentage of overall births, these very sick babies need comprehensive, focused care for the first few years of their lives. And some infants with severe BPD also have pulmonary hypertension which, at Children’s National, is co-managed by cardiology and pulmonary specialists.
Children’s BPD team not only focuses on the child’s survival and medical care, they focus on the neurodevelopmental and social care that a baby needs to thrive. From enhanced nutrition to occupational and physical therapy to a regular sleep cycle, the goal is to help these babies achieve their full potential.
“These babies are at tremendous risk for long-term developmental issues. Everything we do is geared to alleviate that,” adds John T. Berger III, M.D., director of Children’s Pulmonary Hypertension Program.
“Our NICU care is more focused, comprehensive and consistent,” agrees Mariam Said, M.D., a neonatologist on the team. “We’re also optimizing the timing of care and diagnostic testing that will directly impact health outcomes.”
Leaving no detail overlooked, the team also ensures that infants have age-appropriate developmental stimuli, like toys, and push for early mobility by getting children up and out of bed and into a chair or riding in a wagon.
“The standard approach is to keep the baby in a room with limited physical or occupational therapy and a lack of appropriate stimulation,” says Geovanny Perez, M.D., a pulmonologist on the team. “A normal baby interacts with their environment inside the home and outside the home. We aim to mimic that within the hospital environment.”
Dr. Steinhorn, who had long dreamed of creating this comprehensive team care approach adds that “it’s been so gratifying to see it adopted and embraced so quickly by Children’s NICU caregivers.”