Tag Archive for: nutrition
To understand the preterm brain, start with the fetal brain

“My best advice to future clinician-scientists is to stay curious and open-minded; I doubt I could have predicted my current research interest or described the path between the study of early oligodendrocyte maturation to in vivo placental development, but each experience along the way – both academic and clinical – has led me to where I am today,” Nickie Andescavage, M.D., writes.
Too often, medical institutions erect an artificial boundary between caring for the developing fetus inside the womb and caring for the newborn whose critical brain development continues outside the womb.
“To improve neonatal outcomes, we must transform our current clinical paradigms to begin treatment in the intrauterine period and continue care through the perinatal transition through strong collaborations with obstetricians and fetal-medicine specialists,” writes Nickie Andescavage, M.D., an attending in Neonatal-Perinatal Medicine at Children’s National.
Dr. Andescavage’s commentary was published online March 25, 2019, in Pediatrics Research and accompanies recently published Children’s research about differences in placental development in the setting of placental insufficiency. Her commentary is part of a new effort by Nature Publishing Group to spotlight research contributions from early career investigators.
The placenta, an organ shared by a pregnant woman and the developing fetus, plays a critical but underappreciated role in the infant’s overall health. Under the mentorship of Catherine Limperopoulos, Ph.D., director of MRI Research of the Developing Brain, and Adré J. du Plessis, M.B.Ch.B., MPH, chief of the Division of Fetal and Transitional Medicine, Dr. Andescavage works with interdisciplinary research teams at Children’s National to help expand that evidence base.
While attending Cornell University as an undergraduate, Dr. Andescavage had an early interest in neuroscience and neurobehavior. As she continued her education by attending medical school at Columbia University, she corroborated an early instinct to work in pediatrics.
It wasn’t until the New Jersey native began pediatric residency at Children’s National that those complementary interests coalesced into a focus on brain autoregulation and autonomic function in full-term and preterm infants and imaging the brains of both groups. In normal, healthy babies the autonomic nervous system regulates heart rate, blood pressure, digestion, breathing and other involuntary activities. When these essential controls go awry, babies can struggle to survive and thrive.
“My best advice to future clinician-scientists is to stay curious and open-minded; I doubt I could have predicted my current research interest or described the path between the study of early oligodendrocyte maturation to in vivo placental development, but each experience along the way – both academic and clinical – has led me to where I am today,” Dr. Andescavage writes in the commentary.
Getting micro-preemie growth trends on track
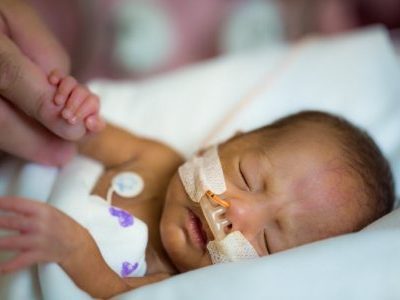
According to Children’s research presented during the Institute for Healthcare Improvement 2018 Scientific Symposium, standardizing feeding practices – including the timing for fortifying breast milk and formula with essential elements like zinc and protein – improves growth trends for the tiniest preterm infants.
About 1 in 10 infants is born before 37 weeks gestation. These premature babies have a variety of increased health risks, including deadly infections and poor lung function.
Emerging research suggests that getting their length and weight back on track could help. According to Children’s research presented during the Institute for Healthcare Improvement 2018 Scientific Symposium, standardizing feeding practices – including the timing for fortifying breast milk and formula with essential elements like zinc and protein – improves growth trends for the tiniest preterm infants.
The quality-improvement project at Children’s National Health System targeted very low birth weight infants, who weigh less than 3.3 pounds (1,500 grams) at birth. These fragile infants are born well before their internal organs, lungs, brain or their digestive systems have fully developed and are at high risk for ongoing nutritional challenges, health conditions like necrotizing enterocolitis (NEC) and overall poor development.
The research team measured progress by tracking the micro-preemies’ mean delta weight Z-score for weight gain, which measures nutritional status.
“In this cohort, mean delta weight Z-scores improved by 43 percent, rising from -1.8 to the goal of -1.0, when we employed an array of interventions. We saw the greatest improvement, 64 percent, among preterm infants who had been born between 26 to 28 weeks gestation,” says Michelande Ridoré, MS, Children’s NICU quality-improvement program lead who presented the group’s preliminary findings. “It’s very encouraging to see improved growth trends just six months after introducing these targeted interventions and to maintain these improvements for 16 months.”
Within Children’s neonatal intensive care unit (NICU), micro-preemies live in an environment that mimics the womb, with dimmed lighting and warmed incubators covered by blankets to muffle extraneous noise. The multidisciplinary team relied on a number of interventions to improve micro-preemies’ long-term nutritional outcomes, including:
- Reducing variations in how individual NICU health care providers approach feeding practices
- Fortifying breast milk (and formula when breast milk was not available), which helps these extra lean newborns add muscle and strengthen bones
- Early initiation of nutrition that passes through the intestine (enteral feeds)
- Re-educating all members of the infants’ care teams about the importance of standardized feeding and
- Providing a decision aid about feeding intolerance.
Dietitians were included in the daily rounds, during which the multidisciplinary team discusses each infant’s care plan at their room, and used traffic light colors to describe how micro-preemies were progressing with their nutritional goals. It’s common for these newborns to lose weight in the first few days of life.
- Infants in the “green” zone had regained their birth weight by day 14 of life and possible interventions included adjusting how many calories and protein they consumed daily to reflect their new weight.
- Infants in the “yellow” zone between day 15 to 18 of life remained lighter than what they weighed at birth and were trending toward lower delta Z-scores. In addition to assessing the infant’s risk factors, the team could increase calories consumed per day and add fortification, among other possible interventions.
- Infants in the “red” zone remained below their birth weight after day 19 of life and recorded depressed delta Z-scores. These infants saw the most intensive interventions, which could include conversations with the neonatologist and R.N. to discuss strategies to reverse the infant’s failure to grow.
Future research will explore how the nutritional interventions impact newborns with NEC, a condition characterized by death of tissue in the intestine. These infants face significant challenges gaining length and weight.
Institute for Healthcare Improvement 2018 Scientific Symposium presentation
- “Improved growth of very low birthweight infants in the neonatal intensive care unit.”
Caitlin Forsythe, MS, BSN, RNC-NIC, NICU clinical program coordinator, Neonatology, and lead author; Michelande Ridoré, MS, NICU quality-improvement program lead; Victoria Catalano Snelgrove, RDN, LD, CNSC, CLC, pediatric clinical dietitian; Rebecca Vander Veer, RD, LD, CNSC, CLC, pediatric clinical dietitian; Erin Fauer, RDN, LD, CNSC, CLC, pediatric clinical dietitian; Judith Campbell, RNC, IBCLC, NICU lactation consultant; Eresha Bluth, MHA, project administrator; Anna Penn, M.D., Ph.D., neonatologist; Lamia Soghier, M.D., MEd, Medical Unit Director, Neonatal Intensive Care Unit; and Mary Revenis, M.D., NICU medical lead on nutrition and senior author; all of Children’s National Health System.
Connecting allied health professionals in pediatric nephrology

With the meeting in Washington this year, Children’s National Health System will be the local host, a distinct honor for an academic medical center that treats hundreds of nephrology patients each year, says pediatric Nephrologist Asha Moudgil, M.D., who directs Children’s kidney transplant service.
Pediatric nephrology is a relatively small specialty worldwide, encompassing just a few hundred doctors in the U.S. For each allied health field that provides collaborative care with these physicians – including nutrition, child-life, psychology and social work – the numbers of providers are even smaller. There are no national meetings for these individual subspecialty fields and no venues to meet new like-minded colleagues or learn about new research or protocols.
Six years ago, the American Society of Pediatric Nephrology (ASPN) aimed to help resolve this dilemma by launching a new multidisciplinary symposium that brings together allied health professionals of all kinds within pediatric nephrology.
Each year, the “ASPN Multidisciplinary Symposium” changes locations, allowing the meeting to target different regional groups of allied health professionals based on geography. With the meeting in Washington this year, Children’s National Health System will be the local host, a distinct honor for an academic medical center that treats hundreds of nephrology patients each year, says pediatric Nephrologist Asha Moudgil, M.D., who directs Children’s kidney transplant service.
There are multiple advantages to having the symposium in Washington, Dr. Moudgil explains. One is access to Children’s experts in this field, who have a wealth of experience in managing issues that affect patients who live in the greater Washington area. For example, the keynote address scheduled for the meeting’s opening night will be delivered by Jennifer Verbesey, M.D., Children’s surgical director of pediatric kidney transplantation, focusing on living donation in minority populations. Living kidney donors and recipients who are minorities have unique issues that can affect organ longevity, explains Dr. Moudgil, which may not be well known by all clinicians.
Children’s speakers also focus prominently in the main session on the second day, including:
- Angela Boadu, RD, LDN/LD, a registered dietitian, and Kaushalendra Amatya, Ph.D., a psychologist, are giving a talk about nutrition and the psychosocial aspects of obesity
- Surgeon Evan Nadler, M.D., director of Children’s Bariatric Surgery Program, is speaking about bariatric surgery before and after transplantation
- Nurse Practitioner Christy Petyak, CPNP-PC, and Social Worker Heidi Colbert, LICSW, CCTSW, NSW-C, are leading breakout sessions about the practical aspects of immunosuppressive therapy and resources for uninsured patients
- Amatya, the Children’s psychologist, also is leading a breakout session on internalizing psychological disorders in pediatric renal patients and
- Registered Dietitian Kristen Sgambat, Ph.D., RD, and Dr. Moudgil are co-leading a breakout session on nutritional challenges and enteral supplementation in chronic kidney disease.
Another advantage to holding the meeting in the nation’s capital is its close proximity to government research and federal regulatory agencies, such as the Food and Drug Administration (FDA) and the National Institutes of Health (NIH). Speakers from both agencies will be present, talking about how the FDA approves medicines for pediatric patients and offering details about the NIH’s rare disease program.
Besides the abundance of more formal knowledge-sharing, Dr. Moudgil adds, there will be plenty of opportunities for attendees to network, making connections within and outside their own respective fields.
“This is a platform for making long-term professional relationships,” Dr. Moudgil says. “Even if you’re the sole clinician representing your specialty at your own institution, you’ll be able to connect with other specialists at institutions across the country. You’re not only acquiring new information, you’re acquiring a group of colleagues you can connect with this year and those professional relationships can extend far into the future.”
Use of dietary supplements in children with Down syndrome

There is a widespread practice of parents giving dietary supplements to children with Down syndrome in the hope of improving intelligence or function, according to new research published in The Journal of Pediatrics. The study, conducted by experts at Children’s National Rare Disease Institute (CNRDI), examined the prevalence, perceived impact, cost and other factors related to dietary supplement use in children with Down syndrome.
The survey finds nearly half of 1,167 respondents – 49 percent – have given or currently give dietary supplements to their children in an effort to improve health and development. On average, children receive three of the more than 150 supplements reported, with nearly 30 percent of users beginning supplementation before the child’s first birthday.
Amy Feldman Lewanda, M.D., a medical geneticist at CNRDI and lead author on the study, notes that the results also reveal a troubling trend – nearly 20 percent of parents who report using dietary supplements do not inform their pediatrician.
“While we know supplements are given by parents in hopes of improving developmental outcomes for children with Down syndrome, many of these supplements contain concerning ingredient profiles that can have adverse effects in infants and children that are too young to communicate their symptoms,” says Dr. Lewanda. “Additionally, these supplements have no proven safety or efficacy, so it’s important for families to consult with their pediatrician or primary care provider to help determine any risk, ill effects or conflicts with existing treatment.”
Reasons for not informing pediatricians about supplement use vary, according to the study results. The most common reason reported was that the doctor has never specifically asked about nutritional supplements. While some parents indicate they do not view supplement use as important medical information to divulge, others feel that their pediatrician may not be knowledgeable about these types of supplements or may dismiss the practice entirely, as some reportedly have done in the past.

Amy Feldman Lewanda, M.D., a medical geneticist at CNRDI and lead author on the study.
The most popular class of products reported by 25.8 percent of respondents taking supplements are antioxidants, such as curcumin, a byproduct of turmeric, and epigallocatechin-3-gallate (ECGC), the polyphenol compound in green tea. Vitamins, both single and multivitamins, rank second, accounting for 18.9 percent of supplement use. B vitamins were the most popular among single vitamin use. The third most popular supplement category, reported by 15.8 active or previous supplement users, contains proprietary products or combination supplements, such as Nutrivene-D or HAP-CAPS (High Achievement Potential Capsules).
According to Dr. Lewanda, chemical analyses of herbal supplements find some contain anabolic steroids or pharmaceuticals that aren’t listed in the ingredients. Hepatoxicity has been cited among 60 herbs, herbal drugs and herbal supplements. The problem, she notes, is that these products aren’t regulated, like pharmaceuticals are, and similarly, they aren’t thoroughly tested for their safety and efficacy.
The study also notes potential concerns about consuming hyper-concentrated forms of fat-soluble vitamins, including vitamin E and vitamin K, which stay in the body until the vitamins are used. One particular supplement, Speak, provides 5,000 percent of the recommended daily value limits of vitamin E. Fat-soluble vitamins and/or herbal supplements pose unknown health risks – including liver damage.
Among study respondents who actively provide supplements to their children, roughly 87 percent feel they are effective. Those who stopped administering supplements to their children cite lack of efficacy and cost – approximately $90.53 per month on average – as leading reasons for discontinuing use. Approximately 17 percent of respondents note side-effects of supplement use, specifically gastrointestinal disturbance, which was the most common side effect among active and previous supplement users.
“This research gives pediatricians a bit of a wake-up call on what’s trending in the Down syndrome community and the dialogue taking place online, in parent support groups and outside of the doctor’s office,” says Marshall Summar, M.D., director of CNRDI and co-author on the study. “The goal is for pediatricians and parents to work as a team in providing the best care possible for every child, so we hope this research provides physicians greater insight and encourages more open dialogue with patient families about supplement use. Since many of these supplements have active ingredients, it is vitally important that the primary care provider be aware of them.”
Healthy Homes, Healthy Futures program receives national recognition

Children’s National expert Kofi Essel (far right) was one of the Children’s National physicians recognized as a health care pioneer at the Clinton Foundation’s Health Matters Activation Summit in Little Rock, Arkansas.
Children’s National Health System physicians were recognized as health care pioneers at the Clinton Foundation’s Health Matters Activation Summit in Little Rock, Arkansas, in early April for their creation of “Healthy Homes, Healthy Futures,” an obesity-centered home visitation curriculum for pediatric residents at Children’s National. The program received the first-ever Innovation Award for Health Care Provider Training and Education and was named the most innovative program for current health care professionals.
The award recognizes leading health professional training programs that promote nutrition, physical education and obesity counseling education to its students. Co-collaborators of the program include: Children’s National experts Kofi Essel, M.D., FAAP, Sirisha Yalamanchi, M.D., FAAP and Cara Lichtenstein, M.D., M.P.H., FAAP, as well as Erin Hysom, R.D.N., M.P.H., of the Maryland State Department of Education.
According to Dr. Essel, the team created the program to address the lack of knowledge providers have of the patient’s home and neighborhood environment, which is critical to understanding the barriers that families face when struggling with obesity.

Dr. Essel accepted the Innovation Award for Health Care Provider Training and Education on behalf of his team presented by former President Bill Clinton.
“Traditional medical training has been ineffective in equipping the next generation of providers with practical ways to manage or prevent obesity,” says Dr. Essel. “We created our program to address this issue and focus on the underlying sociocultural factors that are associated with obesity.”
To better equip providers, the program’s home visitation curriculum offers a unique approach to improve residents’ understanding of the social determinants of health, unpack how these underlying barriers can lead to obesity and strengthen critical goal-setting and obesity-management skills.
Dr. Essel and his team proudly accepted the award presented by former President Bill Clinton. Ultimately, Dr. Essel hopes to influence a national narrative around obesity, build empathy and reduce stigma toward families through immersion training, empower patients to improve their own health and help providers gain confidence in communicating about and managing obesity through the family context.
AAP presentations on feeding disorders
Irene Chatoor, M.D., vice chair of the Department of Psychiatry and Behavioral Sciences at Children’s National Health System, specializes in helping children work through their food anxieties and encourages parents to set aside dedicated time for family meals. That’s expertise she will share with peers at the American Academy of Pediatrics 2016 National Conference.
“I also want to help pediatricians to differentiate between toddlers who ‘no-no-NO’ to the few foods they don’t like – which is OK – and children whose food selection is quite limited,” she says. “They need to be aware of red flags, like a child who spits out food, gags, or grimaces in response to certain foods or refuses to eat other foods that may look similar or that have the same texture as the aversive foods.”
Their limited may lead to nutritional problems, and also may have emotional consequences, according to a 2015 article published in Pediatrics for which Dr. Chatoor was senior author.
This makes parents increasingly anxious, and they often try all kinds of distractions to get their child to eat. Dr. Chatoor has described this feeding disorder as infantile anorexia. Interestingly, research has shown that families who eat together at regular times help their children to outgrow their feeding problems.
AAP 2016 presentations:
Saturday, October 22, 2016
• F1069- “Food Refusal: From Picky Eating to Feeding Disorders”
9:30 a.m. to 10:15 a.m.
Sunday, October 23, 2016
• F2012- “Food Refusal: From Picky Eating to Feeding Disorders”
7:30 a.m. to 8:15 a.m.
Unbelievable survivability rates for short bowel patients

When other doctors ask Clarivet Torres, M.D., how she is getting the best survivability rates for patients with Short Bowel Syndrome (SBS), she says her success is because of teamwork.
The Intestinal Rehabilitation Program (IRP) at Children’s National, started in 2007 when Dr. Torres joined the health system and became the program’s director, has shown 98 percent survivability for patients with SBS over a period of nine years. That’s compared with a recent study from the Pediatric Intestinal failure consortium (Predictors of Enteral Autonomy in Children’s with Intestinal Failure: a Multicenter Cohort Study), which showed that 43 percent of the patients died or underwent transplantation over a median follow-up of 33.5 months.
Intestinal failure often prevents these patients from digesting enough nutrients and fluids to maintain proper growth, and they often require parenteral nutrition (PN). Dr. Torres’ team has helped to wean 91.3 percent of patients from PN, compared with the above study, which showed that enteral autonomy was achieved in 43 percent.
Based on the outcomes for the first 120 children with SBS treated in Children’s National’s IRP from 2007 to 2016, Dr. Torres says that with meticulous and aggressive medical/surgical management, even patients with advanced liver disease can show improvement in liver functions and nutritional parameters with the ability to discontinue parenteral nutrition and avoid the need for transplantation.
“These are very, very good results for any program and ours has been growing substantially in the last 10 years,” Dr. Torres says. “We are like a family, we are very good at teaching so everyone knows how to care for these patients.”
Cross-departmental collaboration
Her main focus as director has been spreading the word about SBS across the departments. For example, the ER knows to start IV fluids on these patients right away or to keep watch for sepsis symptoms. From nurses, pediatric residents, and surgeons to radiologists and the ER, Dr. Torres has encouraged the sharing of knowledge and teaching how to respond to SBS patients.
Dr. Torres also attributes the success of the Children’s National’s program to having a multidisciplinary intestinal rehabilitation team who are trained to follow up with these highly complex patients with SBS. “In general, these patients have a very high morbidity-mortality rate, and it’s important to be close to follow up.”
Members of the IRP includes, a dedicated surgeon, Anthony Sandler, M.D., and four supporting GI doctors (Parvathi Mohan, M.D., Vahe Badalyan, M.D., Sona Sehgal, M.D., and Muhammad Khan, M.D.).
Other important members are one physician assistant, two nurse practitioners, two coordinators, one dietitian, one social worker, one case manager, and devoted nurses who work in the specialized Intestinal Rehabilitation Unit.
Having a dedicated director and surgeon also is a new perspective. Focusing on this group of patients allows Drs. Torres and Sandler to become experts in the medical and surgical management of the patients with short bowel and intestinal failure.
A closer look inside the program
The goal of the IRP is to optimize bowel function through the use of multiple therapies and to eventually wean patients with intestinal failure from parenteral nutrition. The medical treatment focuses on comprehensive dietary management with very precise control of metabolic balance and prompt and effective treatment of complications.
Pro-adaptive surgery, such as stoma closure, ostomy in continuity, stricturoplasty, enteroplasty, and autologous gut reconstruction, with the longitudinal intestinal lengthening and tailoring (LILT) and serial transverse enteroplasty (STEP) procedures, may produce dramatic clinical improvement in patients with SBS.
The use of specialized enteral feeding programs by the experience medical team helps to maintain nutrition and hydration, which are important factors in long-term survival. Other important components of the program are ongoing parent education and support, and promoting an optimal quality of life. Intestinal transplantation with MedStar Georgetown University Hospital is an option for patients who fail treatment.
“The Intestinal Rehabilitation at Children’s National provides children with intestinal failure the chance to receive comprehensive medical and surgical care, giving them the chance for improved long-term survival, including weaning from parenteral nutrition and avoidance of the need for transplantation and long-term immunosuppression,” Dr. Torres says.