President Biden, First Lady tour cardiac telehealth command center
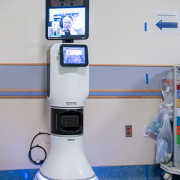
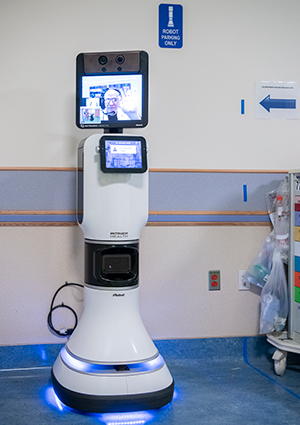
President Joe Biden and First Lady Jill Biden paid a recent visit to the Cardiac Intensive Care Unit (CICU) at Children’s National Hospital, where leaders of our cardiology services toured them through the state-of-the-art telehealth command center embedded on the unit.
The big picture
Children’s National is pioneering the integration of telemedicine into CICU care. It’s one of the few pediatric hospitals in the world to do this.
Experts liken the telehealth command center to an ‘air traffic control tower’ for the most vulnerable patients with critical heart disease. The President and First Lady saw how complex the environment is, with real-time monitoring of all 26 high-risk patients in the CICU. The system combines traditional remote monitoring, video surveillance and artificial intelligence tools.
What this means
“With this technology, we’re helping to predict and prevent major adverse events,” said Ricardo Munoz, M.D., executive director of the Telemedicine Program and chief of the Division of Critical Care Medicine at Children’s National. “For example, our neuromonitoring system can help signal an impending brain injury before it happens.”
Dr. Munoz says President Biden expressed interest in the prevention strategy of adverse events and this new approach to caring for children with critical cardiac illness.
What they’re saying
- “It was important to share with the Biden’s that caring for these kids is a long-term endeavor, not simply a single surgery or procedure to fix their heart abnormality,” said Yves d’Udekem, M.D., Ph.D., chief of Cardiac Surgery at Children’s National. “That means making sure they have the earliest diagnoses, the best treatments from surgeons and others who truly understand their condition, and a technologically advanced, attentive place to recover and heal as safely as possible.”
- “Many people don’t believe that ‘pediatrics’ and ‘innovation’ can co-exist,” said Annette Ansong, M.D., medical director of Outpatient Cardiology at Children’s National. “During the Biden’s visit, they were at the crux of a novel way to closely monitor some of our sickest children with the added ability to predict bad events before they happen.”
Dr. Ansong hopes bringing awareness of these cardiac capabilities to the President and First Lady is the first of many steps in seeking support for children with congenital and acquired heart disease.









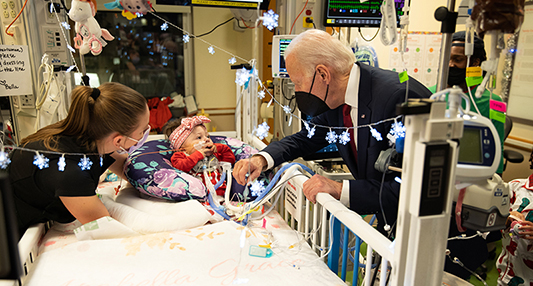



 Children’s National Hospital named
Children’s National Hospital named