Children’s National performs first ever HIFU procedure on patient with cerebral palsy
HIFU is a non-invasive therapy that utilizes focused ultrasound waves to thermally ablate a focal area of tissue.
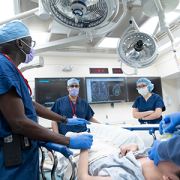
In January, a team of multidisciplinary doctors performed the first case in the world of using bilateral high intensity focused ultrasound (HIFU) pallidotomy on Jesus, a 22-year-old patient with dyskinetic cerebral palsy.
The procedure is part of a clinical trial led by Chima Oluigbo, M.D., pediatric neurosurgeon at Children’s National Hospital.
“The primary objective of the study is to evaluate the safety of ExAblate Transcranial MRgFUS as a tool for creating bilateral or unilateral lesions in the globus pallidus (GPi) in patients with treatment-refractory secondary dystonia due to dyskinetic cerebral palsy,” Dr. Oluigbo explained. “The secondary purpose is to assess the impact of HIFU pallidotomy on dyskinetic cerebral palsy movement disorder in pediatric and young adult patients.”
In addition, the impact of bilateral pallidotomy on motor development, pain perception, speech, memory, attention and cognition in these patients will be assessed.
“We hope that the trial will help us find results that lead to treatments that can reduce the rigidity and stiffness which occurs in cerebral palsy so we can help these children who do not have any effective treatment,” Dr. Oluigbo added.
“This new, first of its kind, non-invasive therapeutic approach – without even a skin incision – will open the door to offering hope for a number of kids with movement disorders who have failed conventional therapy,” said Robert Keating, M.D., chief of neurosurgery at Children’s National. “We are at the beginning of a new era for treating functional disorders in the pediatric patient.”
How it works
HIFU is a non-invasive therapy that utilizes focused ultrasound waves to thermally ablate a focal area of tissue. In the past, Children’s National successfully used HIFU to treat low-grade type tumors located in difficult locations of the brain, such as hypothalamic hamartomas and pilocytic astrocytoma, as well as for epilepsy and other movement disorders.
This most recent procedure was another successful milestone for the hospital, discharging Jesus the following day without any complications.
The team comprised neurosurgeons, MRI techs, anesthesiologists and radiologists, to name a few.
Originally, Jesus came to Children’s National in 2006 when he started working with the Physical Medicine and Rehabilitation team to help him with his muscle hypertonia management as well as equipment, orthoses and therapy concerns.
“As he continued to grow, his muscle hypertonia became more pronounced and caused difficulty with his care, positioning and comfort,” said Olga Morozova, M.D., pediatric rehabilitation specialist at Children’s National. “We have tried multiple oral medications however he has had significant side effects from the majority of the medications.”
Dr. Morozova and Julie Will, M.S.N., F.N.P., the nurse practitioner that worked with Jesus, referred him to Dr. Oluigbo after they learned about HIFU being an option to treat Jesus using a non-invasive approach.
Moving the field forward
This clinical trial highlights the expanding indications for focused ultrasound.
“We are excited about the potential for these innovative treatment strategies in neurosurgery to transform the lives of pediatric patients who suffer from challenging diseases, such as brain tumors, epilepsy, and movement disorders,” said Hasan Syed, M.D., co-director of the Focused Ultrasound Program at Children’s National. “We are redefining what is possible in neurosurgery.”
From low-intensity focused ultrasound (LIFU) treatments for our young DIPG patients to now the groundbreaking research on HIFU for pediatric movement disorders, the dedication to cutting-edge techniques highlights the team’s commitment to patients and transforming pediatric neurosurgical care.