A new way to treat pediatric gliomas with BRAF V600 mutations
Gliomas account for 45% of all pediatric tumors of the central nervous system.
Gliomas, which can be classified according to histologic grade as high or low grade, account for 45% of all pediatric tumors of the central nervous system. Detection of the BRAF V600E mutation in pediatric low-grade glioma has been associated with a lower response to standard chemotherapy. In previous trials, dabrafenib (both as monotherapy and in combination with trametinib) has shown efficacy in recurrent pediatric low-grade glioma with BRAF V600 mutations, findings that researchers found warrant further evaluation of this combination as first-line therapy.
The big picture
In a recent study published in the New England Journal of Medicine, experts found that among a randomized cohort of 110 children with low-grade glioma with BRAF V600 mutations, dabrafenib plus trametinib resulted in significantly more responses, longer progression-free survival and a better safety profile than standard chemotherapy as first-line therapy.
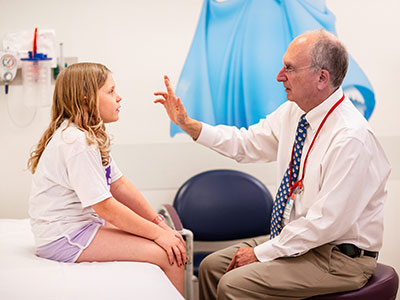
“For the past 20 to 30 years, the only effective safe therapy was chemotherapy. In older children, radiation can also be effective, but there’s reluctance on using radiation on a developing brain,” said Roger Packer, M.D., director of the Brain Tumor Institute at Children’s National Hospital and co-author of the study. “As we learned the specific molecular genetic makeups of these tumors, either high- or low-grade gliomas, we found it to be effective to use molecular therapies. These are safer and more effective than chemotherapy alone.”
Dr. Packer also added that there’s approval from the FDA, proving that the industry sees value in investing in pediatrics.
Why it matters
This randomized trial shows the superiority of dabrafenib plus trametinib as a first systemic therapy for pediatric patients with low-grade glioma with BRAF V600 mutations as compared with carboplatin plus vincristine, the standard chemotherapy approach. This benefit was evident in the higher independently determined response, longer progression-free survival and better side-effect profile as reflected in the lower frequency of treatment discontinuation because of toxicity.
“Children treated with a molecular targeted therapy could safely tolerate the therapy and had better outcomes than children who were treated with chemotherapy,” Dr. Packer added.
Overall, these findings show the value of early molecular testing in children with low-grade glioma to determine the presence or absence of BRAF V600 mutations.
You can read the full study “Dabrafenib plus Trametinib in Pediatric Glioma with BRAF V600 Mutations” here.