Tag Archive for: imperforate anus
Evidence to eliminate burdensome postop practice after imperforate anus repair
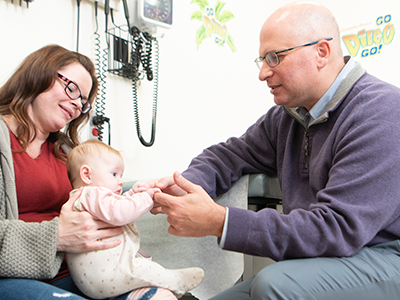
The study was co-led by Marc Levitt, M.D., who launched the division of Pediatric Colorectal and Pelvic Reconstructive Surgery at Children’s National Hospital in late 2019.
A prospective randomized controlled trial has given pediatric colorectal specialists the first evidence to reconsider a standard postoperative care practice: Routine anal dilations following a primary posterior sagittal anorectoplasty (PSARP), an operation to reconstruct a child born with imperforate anus. This treatment has been the standard of care following PSARP for more than thirty years and was believed to help prevent strictures after surgery for anorectal malformations (imperforate anus). However, it requires parents and caregivers to perform this uncomfortable procedure on their child daily, which can have a significant psychological impact on the child. Prior to this trial, a quality of life assessment found that postoperative dilations were the most stressful part of these patients’ care for both patient and parents.
“The PSARP procedure, performed for the first time in 1980, improves the lives of children born with imperforate anus by providing a safe and effective reconstruction technique,” says Marc Levitt, M.D., who led the study with co-author Richard Wood, M.D., of Nationwide Children’s Hospital, before joining Children’s National Hospital as chief of the division of Colorectal and Pelvic Reconstructive Surgery. “We are thrilled to have evidence that one of the top postoperative challenges for parents – a twice daily anal dilation for several months after the surgery is completed – can potentially be eliminated for most kids with no impact on their recovery.”
“We also found that if a stricture, or scar, develops, which occurs in only about 10 percent of cases, it can easily be managed with a minor operative procedure done at the same time as colostomy closure, which in most cases they already need. So, if a family had to choose between daily dilations for months or a one in 10 risk of needing a minor surgical procedure, they can now make that choice and avoid routine dilations.”
The prospective single institution randomized controlled trial was conducted between 2017 and 2019 and included 49 patients. The abstract of the results was accepted for presentation at the British Association of Paediatric Surgeons Annual International Congress, 2020, and its manuscript is to be published.
“The clinical benefit of routine dilation had never been studied in a formal way, it had been accepted as surgical dogma. Our cohort, who underwent a randomized controlled trial, gave us the ability to look at this practice in an evidence-based way,” Dr. Levitt says. “Revising this practice could be a real game-changer for parents and kids with anorectal malformations.”
Pediatric Colorectal and Pelvic Reconstructive Surgery textbook now available

The cover of the new Pediatric Colorectal and Pelvic Reconstructive Surgery textbook, edited by Marc A. Levitt, M.D., and Alejandra Vilanova-Sánchez, M.D.
The first edition of the Pediatric Colorectal and Pelvic Reconstructive Surgery textbook, edited by Marc A. Levitt, M.D., and Alejandra Vilanova-Sánchez, M.D., is now available.
The textbook provides comprehensive coverage of the anatomical and physiological aspects of complex colorectal and pelvic malformations presented in a practical and clinically focused way. Some of the topics explored include surgical protocols, the benefits of high-level collaboration between surgical services when treating these anomalies, treatment algorithms and care of complications.
The book also includes content on:
- Evaluation and management of the newborn
- Surgical interventions of the newborn, and when a primary repair versus a staged approach is required
- The value of laparoscopy and when to use it
- The importance of a transition program to adulthood
The Pediatric Colorectal and Pelvic Reconstructive Surgery, 1st edition textbook can be purchased here, and will benefit colorectal teams worldwide.
About the Editors

Marc Levitt, M.D., leads the colorectal program at Children’s National Hospital and is editor of the new Pediatric Colorectal and Pelvic Reconstructive Surgery textbook.
Marc Levitt, M.D., currently leads the colorectal program at Children’s National Hospital, the first in the mid-Atlantic region to fully integrate surgery, urology, gynecology and gastroenterology into one cohesive program for children. He has been the driving force around the world in enhancing the care of children with colorectal and pelvic reconstructive needs through the development of specialized, integrated and collaborative surgical centers. He is internationally recognized as specializing in conditions affecting the newborn, pediatric and adolescent population affected with anorectal malformations (imperforate anus), cloacal malformations, Hirschsprung disease, as well as a variety of conditions leading to fecal incontinence, such as spinal conditions and functional constipation. Dr. Levitt has written three textbooks, and has authored over 200 scientific articles on these subjects.
Dr. Levitt is the founder of the Colorectal Team Overseas (CTO), which is a group of international providers that travel to the developing world to provide care and teaching for patients with colorectal needs. He co-founded the creation of the Pediatric Colorectal and Pelvic Learning Consortium (PCPLC), which is an organization of collaborating colorectal centers across the globe.
Alejandra Vilanova-Sánchez, M.D., is a pediatric surgeon in the urogenital and colorectal unit at the University Hospital La Paz, Madrid. After finishing her training, she completed a fellowship in Pelvic Reconstruction Surgery at the Center for Colorectal and Pelvic Reconstruction at Nationwide Children’s Hospital. Her focus was on complex colorectal and pelvic surgery involving the gynecological and urological systems. Dr. Vilanova-Sánchez is a member of the Spanish Association of Pediatric Surgeons, European Pediatric Surgical Association (EUPSA) and ARM-net. She is a frequent speaker in international meetings and she has organized several national and international meetings on the topic of pediatric colorectal care. She participates annually in surgical brigades collaborating with nonprofit organizations, Colorectal Team Overseas and Helping Hands for Anorectal Malformations International, where she helps patients with colorectal conditions around the world.