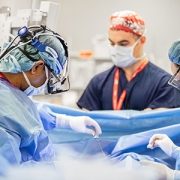
Socioeconomic disadvantage associated with higher long-term mortality after heart surgery
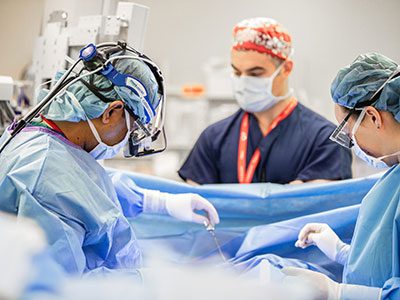
Children who had heart surgery and come from less advantaged neighborhoods in the Washington, D.C., region are much more likely to die in the long term than those from neighborhoods with more wealth and opportunity.
Children who had heart surgery and come from less advantaged neighborhoods in the Washington, D.C., region are much more likely to die in the long term than those from neighborhoods with more wealth and opportunity. The finding was part of a presentation, Socioeconomic Disadvantage Is Associated with Higher Long-Term Mortality After Cardiac Surgery, presented by Jennifer Klein, MD, MPH, cardiologist at Children’s National Hospital, during the Society of Thoracic Surgeons (STS) Annual Meeting in Los Angeles.
What is it?
Clinical and demographic data were collected for 2,546 people who underwent corrective surgery for congenital heart disease over a 15-year period (2007-2022) in a single-center retrospective analysis. Using the Child Opportunity Index (COI), an index that uses environmental/health, educational, and socioeconomic domains to assess patients’ neighborhoods, the two lowest COI quintile neighborhoods were designated as “disadvantaged” while the two highest COI quintile neighborhoods were designated as “advantaged.” Multivariable mixed model analyses were conducted to understand the factors associated with overall mortality.
The research showed that patients from disadvantaged neighborhoods suffered in a great proportion both overall mortality [n=168 (13.6%) vs 66 (8.4%), p< 0.001] and major complications [n=168 (13.6%) vs 81 (10.3%), p< 0.001]. The positive association between neighborhood disadvantage and long-term mortality was maintained in stepwise logistic regression multivariable analysis after controlling for differences between surgical complexity and other clinical risk factors.
What it means
“Previous research has shown disparities like this,” says Dr. Klein. “What’s significant here is that the disparity for children from disadvantaged neighborhoods grows over time. That means corrective interventions won’t be implemented in the operating room or within the first 30 days after surgery. They need to happen in a cardiologist’s office, in the schools, and in the community long after a child goes home from the hospital.”
The findings from this particular study are also noteworthy as they are the first to include significantly greater numbers of patients who are more likely to experience this risk (48.5% of the study group). Previous research has sought to look at this research question but analysis may have been skewed by an over-representation of socioeconomically advantaged patients.
What’s next
Differences in mortality risk continue to grow greater as more time passes, the authors note, indicating that the disparity is not a product of surgical technique or disparities in care delivery at the time of surgery.
Instead, their outcomes are being influenced by factors outside the operating room. This opens a new avenue of research focused on identifying the “why.”
“What happens after they go home?” Klein asks. “Can they access medications? Do they come back for follow-up appointments? Can they afford food?”
Read the abstract, Socioceconomic Disadvantage Is Associated with Higher Long-Term Mortality After Cardiac Surgery, which was presented during a speed session at the STS Annual Meeting. A full manuscript will be published soon.