AI for good: Children’s National wins global competitions for measuring brain tumors

Meet the winners (left to right): Syed M. Anwar, Ph.D., M.S., principal investigator at Children’s National; Daniel Capellan Martin, M.Sc., Polytechnic University of Madrid; Abhijeet Parida, data scientist at Children’s National; and Austin Tapp, Ph.D., postdoctoral research fellow at Children’s National.
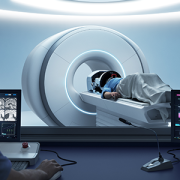
Using an award-winning artificial intelligence (AI) algorithm developed at Children’s National Hospital, researchers ranked first in the world in the Brain Tumor Segmentation-Africa (BraTS-Africa) challenge for their approach to identifying different parts of deadly gliomas. The details of their innovative method were recently published on arXiv, a curated research-sharing platform.
“Technology can bridge the gap in healthcare between high- and low-resource countries,” said Marius George Linguraru, D.Phil., M.A., M.Sc., the Connor Family Professor in Research and Innovation and principal investigator in the Sheikh Zayed Institute for Pediatric Surgical Innovation (SZI). “By tailoring methods we created at our hospital to fit the needs of specific regions, such as sub-Saharan Africa, our research helps improve medical imaging and diagnosis in challenging environments.”
Dr. Linguraru was the program chair of the International Conference on Medical Image Computing and Computer Assisted Intervention (MICCAI) 2024 in Marrakesh, Morocco, the leading global meeting on AI in medical imaging.
Children’s National leads the way
Gliomas are a type of brain tumor with a high death rate and are especially difficult to diagnose in low- and middle-income countries. Given the increased need in Africa, researchers worldwide came together in Morocco to compete over the best way to accurately detect and measure tumors using MRI data and AI.
By applying advanced machine-learning techniques, the researchers adapted tools initially designed for well-resourced settings to work in countries with far fewer.
The study focused on transfer learning, a process in which an AI model is trained in advance on a large number of brain tumor images and then adjusted to work with smaller sets of new data. In this case, the models were adapted to work with local sub-Saharan African data using a strategy to combine different models’ strengths.
When tested, the approach achieved impressive accuracy scores. The Children’s National team, which included a colleague from the Polytechnic University of Madrid, ranked first in the BraTS-Africa 2024 challenge for identifying different parts of gliomas.
“To make the method widely available, the winning algorithm is shared online for others to use and improve upon,” Dr. Linguraru said. “My favorite part of these competitions is how they highlight the way innovation and collaboration can reduce global healthcare inequalities.”
The big picture
Children’s National researchers consistently lead global events using AI and advanced imaging to tackle complex healthcare challenges. In 2023, the team won a global contest to measure pediatric brain tumors at the MICCAI 2023 Conference. This year’s success in the BraTS-Africa challenge builds on this knowledge base and expands its use to adult gliomas.
At the Radiological Society of North America 2024 annual meeting, which drew 50,000 attendees, Zhifan Jiang, Ph.D., a staff scientist in the Precision Medical Imaging Lab at SZI, also won the Cum Laude Award for his scientific poster on applying AI to radiological images to predict severe outcomes for children with brain tumors caused by neurofibromatosis type 1.
“These achievements show how our science is leading the world in using AI for good,” Dr. Linguraru said. “Every day, we’re building on our knowledge of advanced imaging, brain tumors and AI to improve the diagnosis, measurement and treatment of deadly tumors — on a global scale.”