Expanding team innovates to take on pediatric brain tumors

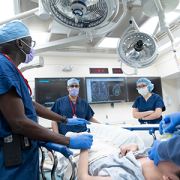
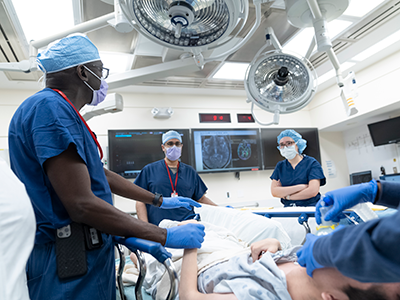
Cheng-Chia “Fred” Wu, M.D., Ph.D., joins the team at the campus as an assistant professor at Virginia Tech’s Fralin Biomedical Research Institute. Image credit: Fralin Biomedical Research Institute.
Experience, talent and technology are coming together at the Children’s National Research & Innovation Campus to solve the complex challenges of treating pediatric brain tumors through a growing partnership between Children’s National Hospital and Virginia Tech.
Cheng-Chia “Fred” Wu, M.D., Ph.D., joins the team at the campus as an assistant professor at Virginia Tech’s Fralin Biomedical Research Institute. He hopes to improve treatment for pediatric brain tumors and other cancers by leveraging technological advances in focused ultrasound and studying how this modality can be combined with other novel therapies. Children’s National physicians and scientists are collaborating with Virginia Tech scientists to develop these new approaches.
Why we’re excited
Catherine Bollard, M.D., M.B.Ch.B., director of the Center for Cancer and Immunology Research and interim chief academic officer at Children’s National, said collaborations — including the partnership between Children’s National and Virginia Tech — are essential to solving formidable scientific challenges.
“We are thrilled to be working with Dr. Wu to develop cutting-edge therapeutics for pediatric brain tumors,” Dr. Bollard said. “With Dr. Wu’s experience and the talents of our team at Children’s National, I have great hope that we will be able to combine our novel technologies and therapies to provide tremendous breakthroughs for treating pediatric patients with brain tumors.”
Before joining Virginia Tech, Dr. Wu was an assistant professor of radiation oncology at Columbia University Irving Medical Center in New York, where he treated pediatric cancers and central nervous system malignancies.
“Partnering with Children’s National connects us to a world-class clinical trial institute that has been a pioneer in treating brain tumors with focused ultrasound technology, and this presents a unique opportunity to help children and families struggling with cancer,” Dr. Wu said. “I can’t wait to see where this takes us.”
Dr. Wu played a key role in the Initiative for Drug Delivery Innovation for Childhood Brain Tumors at Columbia, developing a bench-to-bedside platform to facilitate the translation of promising technologies for targeted drug delivery in children with brain tumors.
Within three years, the team demonstrated the safety and feasibility of using focused ultrasound in the brainstem and adding radiation in preclinical models. They then opened two clinical trials for kids with relapsed diffuse midline glioma, an aggressive and difficult-to-treat brain tumor that occurs in the brain stem, thalamus and spinal cord.
What’s ahead
Dr. Wu will be involved in a wide range of research touching both organizations, including veterinary medicine and biomedical engineering at Virginia Tech.
Michael Friedlander, Ph.D., executive director of the Fralin Biomedical Research Institute at Virginia Tech Carilion and vice president for health sciences and technology at Virginia Tech, welcomed Dr. Wu’s experience as a pediatric radiation oncologist, translational physician-scientist and clinical trialist who has led an innovative drug delivery program.
“He is armed with a unique set of skills to identify promising new technology and implement it in areas of great need for treatment of pediatric cancers,” Dr. Friedlander said. “We are absolutely delighted to have Dr. Wu as part of the team. He represents a powerful new part of the strong partnership between Virginia Tech and Children’s National Hospital for addressing pediatric brain cancer.”