Setting a baseline for healthy brain development
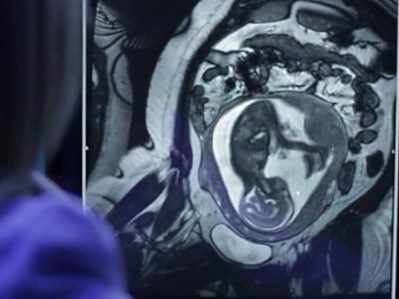
Catherine Limperopoulos, Ph.D., and colleagues performed the largest magnetic resonance imaging study of normal fetal brains in the second and third trimesters of pregnancy.
Starting as a speck barely visible to the naked eye and ending the in utero phase of its journey at an average weight of 7.5 pounds, the growth of the human fetus is one of the most amazing events in biology. Of all the organs, the fetal brain undergoes one of the most rapid growth trajectories, expanding over 40 weeks from zero to 100 billion neurons — about as many brain cells as there are stars in the Milky Way Galaxy.
This exponential growth is part of what gives humans our unique abilities to use language or have abstract thoughts, among many other cognitive skills. It also leaves the brain extremely vulnerable should disruptions occur during fetal development. Any veering off the developmental plan can lead to a cascade of results that have long-lasting repercussions. For example, studies have shown that placental insufficiency, or the inability of the placenta to supply the fetus with oxygen and nutrients in utero, is associated with attention deficit hyperactivity disorder, autism, and schizophrenia.
Recent research has identified differences in the brains of people with these disorders compared with those without. Despite the almost certain start of these conditions within the womb, they have remained impossible to diagnose until children begin to show clinical symptoms. If only researchers could spot the beginnings of these problems early in development, says Children’s National Health System researcher Catherine Limperopoulos, Ph.D., they might someday be able to develop interventions that could turn the fetal brain back toward a healthy developmental trajectory.
“Conventional tools like ultrasound and magnetic resonance imaging (MRI) can identify structural brain abnormalities connected to these problems, but by the time these differences become apparent, the damage already has been done,” Limperopoulos says. “Our goal is to be able to pick up very early deviations from normal in the high-risk pregnancy before an injury to the fetus might become permanent.”
Before scientists can recognize abnormal, she adds, they first need to understand what normal looks like.
In a new study published in Cerebral Cortex, Limperopoulos and colleagues begin to tackle this question through the largest MRI study of normal fetal brains in the second and third trimesters of pregnancy. While other studies have attempted to track normal fetal brain growth, that research has not involved nearly as many subjects and typically relied on data collected when fetuses were referred for MRIs for a suspected problem. When the suspected abnormality was ruled out by the scan, these “quasi-controls” were considered “normal” — even though they may be at risk for problems later in life, Limperopoulos explains.
By contrast, the study she led recruited 166 healthy pregnant women from nearby low-risk obstetrics practices. Each woman had an unremarkable singleton pregnancy and ended up having a normal full-term delivery, with no evidence of problems affecting either the mother or fetus over the course of 40 weeks.
At least one time between 18 and 39 gestational weeks, the fetuses carried by these women underwent an MRI scan of their brains. The research team developed complex algorithms to account for movement (since neither the mothers nor their fetuses were sedated during scans) and to convert the two-dimensional images into three dimensions. They used the information from these scans to measure the increasing volumes of the cerebellum, an area of the brain connected to motor control and known to mediate cognitive skills; as well as regions of the cerebrum, the bulk of the brain, that is pivotal for movement, sensory processing, olfaction, language, and learning and memory.
Their results in uncomplicated, full-term pregnancies show that over 21 weeks in the second half of pregnancy, the cerebellum undergoes an astounding 34-fold increase in size. In the cerebrum, the fetal white matter, which connects various brain regions, grows 22-fold. The cortical gray matter, key to many of cerebrum’s functions, grows 21-fold. And the deep subcortical structures (thalamus and basal ganglia), important for relaying sensory information and coordination of movement and behavior, grow 10-fold. Additional examination showed that the left hemisphere has a larger volume than the right hemisphere early in development, but sizes of the left and right brain halves were equal by birth.
By developing similar datasets on high-risk pregnancies or births—for example, those in which fetuses are diagnosed with a problem in utero, mothers experience a significant health problem during pregnancy, babies are born prematurely, or fetuses have a sibling diagnosed with a health problem with genetic risk, such as autism—Limperopoulos says that researchers might be able to spot differences during gestation and post-natal development that lead to conditions such as schizophrenia, attention deficit hyperactivity disorder and autism spectrum disorder.
Eventually, researchers may be able to develop fixes so that babies grow up without life-long developmental issues.
“Understanding ‘normal’ is really opening up opportunities for us to begin to precisely pinpoint when things start to veer off track,” Limperopolous says. “Once we do that, opportunities that have been inaccessible will start to present themselves.”