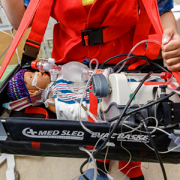
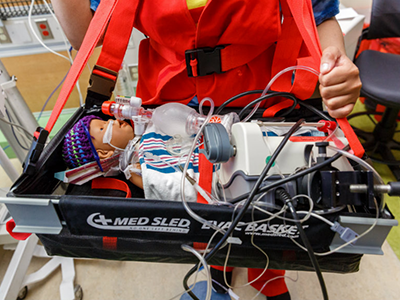
New robot helps care for kids in the emergency room at Children’s National Hospital
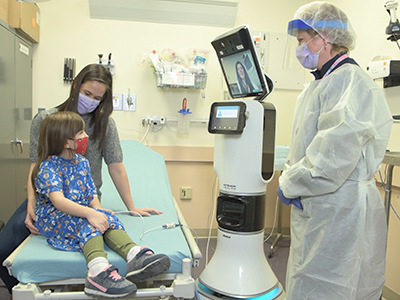
The robot, which is part of the FCC-funded COVID-19 Telehealth Program at Children’s National, is the latest innovation of the program that has rapidly evolved due to the ongoing pandemic.
Children and families who come into the emergency room at Children’s National Hospital may be surprised when their doctor comes in – in the form of a robot. Children’s National introduced a new robot to its Emergency Department (ED) for patients under evaluation for a COVID infection or being treated for other conditions. The robot, which is part of the FCC-funded COVID-19 Telehealth Program at Children’s National, is the latest innovation of the program that has rapidly evolved due to the ongoing pandemic.
“The robot can move in and out of spaces that otherwise we couldn’t get a significant number of providers in, especially with COVID-19 restrictions in place,” said Shireen Atabaki, M.D., M.P.H., associate medical director of Telemedicine, emergency medicine physician and program director for the COVID-19 Telehealth Program at Children’s National. “This is a really exciting program and it implements innovation that we might not have been able to do without the insights we’ve gained from the pandemic.”
The robot is Wi-Fi-enabled and can be remotely controlled by the physician providing the teleconsultation to monitor patient vitals — such as heart rate, body temperature or respiration rate. This allows doctors to work virtually with their team while also having the flexibility to attend to patients faster.
“The pandemic has made us aware of the need to protect patients, families and staff from infectious diseases,” said Alejandro Jose Lopez-Magallon, M.D., medical director of Telemedicine at Children’s National. The robot, he noted, spares clinicians from having to change their PPE, which saves time and gives them the ability to move on to the next patient while nurses and staff continue to provide bedside care.
“We have also seen that whenever a remote clinician is completely alone in the command center and can get on-screen without a mask, in a paradoxical way our patients may be more accepting of seeing a face on a screen that’s not covered with a mask and shield than a stranger using a mask in the same room,” Dr. Lopez-Magallon added.
Soon, the robot will also be used to coordinate subspecialty care — such as cardiac care — in the ED. This will provide more streamlined and expedited care for patients. Instead of leaving with a referral to set up a follow-up appointment with a specialist, patients would be able to receive the consult they need during the same appointment.
The robot is also presenting promising solutions for concerns around the number of restricted visitors. The team at Children’s National recently piloted using an iPad and other technology purchased with the FCC funds to remotely connect family members with patients.
“We downloaded the Zoom app to iPads in our ED to be able to coordinate calls between family members who can’t come in and see patients,” said Dr. Atabaki. “We are looking to implement this as a permanent solution keeping in mind how burdensome and emotionally stressful it has been for many not having the ability to be by the loved one’s side during such a challenging time.”
The FCC funds also covered the telehealth carts, tablets and other connected devices, the telehealth platform, telehealth equipment and innovative AI (augmented intelligence) to treat seriously ill COVID-19 pediatric patients.
The emergency department robot brings the robot-fleet at Children’s National up to three. The first robot was debuted in 2019 to serve children and families in the Cardiac Intensive Care Unit.